Your gift is 100% tax deductible.
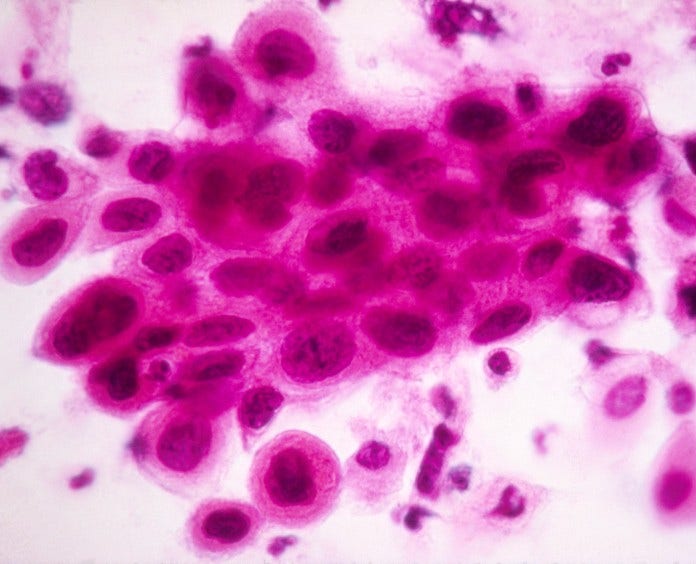
Cervical Cancer
Cervical cancer can often be found early, and sometimes even prevented, by having regular screening tests. If detected early, cervical cancer is one of the most successfully treatable cancers.
Quick Guides
This information is possible thanks to people like you.
We depend on donations to keep our cancer information available for the people who need it most.