Pituitary Tumors
If you have a pituitary tumor or are close to someone who does, knowing what to expect can help you cope. Here you can find out all about pituitary tumors, including risk factors, symptoms, how they are found, and how they are treated.
About pituitary tumors
Pituitary tumors are abnormal growths that start in the pituitary gland. Almost all pituitary tumors are benign (noncancerous) tumors called pituitary adenomas. Pituitary cancers, called pituitary carcinomas, are very rare.
The pituitary gland
The pituitary is a small gland at the base of the skull, just below the brain and above the nasal passages and soft palate (the fleshy back part of the roof of the mouth). The pituitary sits in a tiny bony space called the sella turcica. The nerves that connect the eyes to the brain, called the optic nerves, pass just above it.
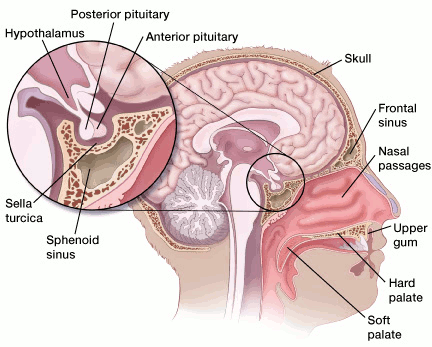
The pituitary is connected directly to part of the brain called the hypothalamus. This links the brain and the endocrine system, a collection of glands and organs in the body that make hormones. Hormones are substances released into the blood that control how other organs work.
The pituitary is considered the “master control gland” because it makes hormones that control the levels of other hormones made by most of the endocrine glands in the body.
The pituitary gland has 2 parts, the anterior pituitary and the posterior pituitary. Each part has distinct functions.
The anterior pituitary
Most pituitary tumors start in the larger, front part of the pituitary gland known as the anterior pituitary. This part of the gland makes several hormones.
Growth hormone (GH, also known as somatotropin) promotes body growth during childhood. If a child or teen's body makes too much growth hormone, they will grow very tall – a condition called gigantism. If an adult's body makes too much growth hormone, the bones of the hands, feet, and face can grow larger than normal, distorting their features. This condition is called acromegaly.
Thyroid-stimulating hormone (TSH, also called thyrotropin) stimulates the thyroid gland to release thyroid hormones, which regulate metabolism. Too much of these hormones makes you hyperactive and shaky, and too little makes you sluggish. If a pituitary tumor makes too much TSH, it can cause hyperthyroidism (an overactive thyroid gland).
Adrenocorticotropic hormone (ACTH, also known as corticotropin) causes the adrenal glands to make steroid hormones, such as cortisol. Too much ACTH from a pituitary tumor causes Cushing disease, the symptoms of which can include rapid weight gain, the buildup of fat in certain parts of the body, high blood pressure, and diabetes.
Luteinizing hormone (LH) and follicle-stimulating hormone (FSH) are also called gonadotropins. In women, their main effects are on the ovaries, where they control ovulation (the release of eggs) and the production of the hormones estrogen and progesterone. In men, LH and FSH control testosterone and sperm production in the testicles.
Prolactin causes milk production in the female breast. Its function in men is not known. Pituitary tumors that make prolactin can cause reproductive problems, as well as milk production in both women and men.
The posterior pituitary
The smaller, back part of the pituitary gland is an extension of brain tissue from the hypothalamus. The posterior pituitary stores and releases the hypothalamus hormones vasopressin and oxytocin into the bloodstream.
Tumors rarely start in the posterior pituitary.
Vasopressin (also called antidiuretic hormone, or ADH) causes the kidneys to keep water in the body, rather than losing it all in the urine. When vasopressin levels are low, a person urinates too much and becomes dehydrated. This condition is called arginine vasopressin deficiency (AVP-D), formerly known as diabetes insipidus. Vasopressin can also raise blood pressure by constricting blood vessels.
Oxytocin causes the uterus to contract in women during childbirth and the breasts to release milk when a woman nurses her baby. It might also have other functions in both men and women.
Types of pituitary tumors
Almost all pituitary tumors are benign pituitary adenomas. In rare cases, they might be cancerous pituitary carcinomas.
Pituitary adenomas
Pituitary adenomas are also known as pituitary neuroendocrine tumors (PitNETs). These benign tumors usually stay in the sella turcica (the tiny space in the skull that the pituitary gland sits in). They usually don’t grow very large, but they can still have a big impact on a person’s health because:
- They might press on nearby parts of the brain and important nerves.
- Some might invade nearby structures like the skull, the sinuses, or nearby nerves or blood vessels.
- Many pituitary adenomas make excess hormones.
There is very little room for tumors to grow in this area. If a tumor gets larger than about a centimeter (about half an inch) across, it might grow upward, where it can press on and damage nearby parts of the brain and the nerves that arise from it. This can lead to problems like vision changes or headaches. (See Signs and Symptoms of Pituitary Tumors.)
Microadenoma vs. macroadenoma
Pituitary adenomas can be classified by size.
Microadenomas are smaller than 1 centimeter (cm) across (less than half an inch). Because these tumors are small, they rarely damage the rest of the pituitary or nearby tissues. But they can still cause symptoms if they make too much of any of the pituitary hormones. Many people have small adenomas that are never found because they don't grow large enough or make enough hormones to cause any problems.
Macroadenomas are tumors that are at least 1 cm across. Macroadenomas can cause symptoms if they press on nearby structures such as normal parts of the pituitary or on nearby nerves. They can also sometimes cause symptoms if they make too much of a certain hormone.
Functional vs. non-functional adenomas
If a pituitary adenoma makes too much of a hormone, it's called a functional or functioning adenoma. If it doesn’t make enough hormones to cause symptoms, it's called a non-functional or non-functioning adenoma.
Functional adenomas often cause symptoms by making excess hormones.
- Lactotroph adenomas (prolactinomas) make prolactin. They account for about 4 out of 10 pituitary tumors.
- Somatotroph adenomas make growth hormone (GH). They make up about 2 in 10 pituitary tumors.
- Corticotroph adenomas make ACTH. They account for about 1 in 10 pituitary tumors.
- Gonadotroph adenomas make LH and FSH. Functional gonadotroph adenomas are very rare.
- Thyrotroph adenomas make TSH. They are very rare.
- Plurihormonal adenomas make more than one hormone. The most common of these are lactotroph/somatotroph adenomas, which make both prolactin and growth hormone.
The kind of hormone an adenoma makes strongly affects what signs and symptoms it causes. It also affects which tests are used to diagnose and follow these tumors and treatment options.
Non-functional adenomas don’t make enough hormones to cause symptoms. Most often these are gonadotroph adenomas that don’t make enough hormones to cause any problems.
Non-functional adenomas account for about 3 in 10 of all detected pituitary tumors. By the time they are found, they usually have grown to be macroadenomas, causing symptoms because of their size as they press on nearby structures.
Aggressive pituitary tumors
While nearly all pituitary adenomas are benign and don’t grow outside of the pituitary, a very small portion grow more aggressively, invading into nearby structures and sometimes coming back after treatments such as surgery or radiation therapy. These are sometimes referred to as aggressive pituitary tumors (APTs).
Pituitary carcinomas
Cancers of the pituitary gland, known as pituitary carcinomas or metastatic PitNETs, are very rare. They can occur at any age, but most are found in older people. These cancers usually make hormones, just like many adenomas do.
Pituitary carcinomas look like pituitary adenomas under a microscope, so doctors have trouble telling them apart. The only way to know for sure that a pituitary tumor is a carcinoma and not an adenoma is when the tumor is found to have spread to another part of the body.
Most often, pituitary carcinomas spread to the brain, spinal cord, meninges (the covering of the brain and spinal cord), or bone around the pituitary. Rarely, these cancers spread to other organs such as the liver, heart, or lungs.
Other tumors of the pituitary region
Other types of benign and malignant (cancerous) tumors can grow in the region of the pituitary. All of these are much less common than pituitary adenomas.
These rare tumors develop from germ cells, which normally form egg cells in women and sperm cells in men. Before birth, germ cells usually travel to the ovaries or testicles and develop into egg or sperm cells. But sometimes some germ cells don’t move where they should and end up in the brain near the pituitary. Germ cell tumors include germinomas, teratomas, choriocarcinomas, embryonal carcinomas, yolk sac tumors, and mixed germ cell tumors. They are usually cancerous. They occur most often in teens or young adults.
These slow-growing tumors start above the pituitary gland but below the brain itself. They sometimes press on the pituitary and the hypothalamus, causing hormone problems. They're more common in children, but they can be seen in older adults. For more on these tumors, see Brain and Spinal Cord Tumors in Children.
Meningiomas are tumors that begin in the meninges, the thin layers of tissue that cover the brain and spinal cord. Most meningiomas are benign. While they can start anywhere along the meninges, some develop near the pituitary.
These are rare, usually slow-growing tumors that start in cells in the posterior pituitary. While these tumors are usually benign (not cancer), they can cause symptoms by pressing on nearby structures or affecting hormone levels.
These are benign, fluid-filled growths in or just above the pituitary. They are usually found in adults.
Rarely, other cancers such as chordomas and primary central nervous system (CNS) lymphomas can affect the pituitary region.
Cancers that start in other parts of the body, like the breast or lung, can sometimes spread to the pituitary. These cancers are classified and treated based on where they started (their primary site) and are not thought of as pituitary tumors.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Asa SL, Mete O, Perry A, Osamura RY. Overview of the 2022 WHO Classification of Pituitary Tumors. Endocr Pathol. 2022;33(1):6-26. Epub 2022 Mar 15.
Calvanese F, Jannelli G, Feuvret L, et al. Aggressive pituitary tumors and pituitary carcinomas: Definition, management, and overview for clinical practice. Neurooncol Adv. 2025 Jan 2;7(Suppl 1):i17-i28.
Dorsey JF, Salinas RD, Dang M, et al. Chapter 63: Cancer of the central nervous system. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa. Elsevier: 2020.
National Cancer Institute. Pituitary Tumors Treatment (PDQ®)–Health Professional Version. 2024. Accessed at https://www.cancer.gov/types/pituitary/hp/pituitary-treatment-pdq on February 11, 2026.
Snyder PJ. Causes, presentation, and evaluation of sellar masses. UpToDate. 2026. Accessed at https://www.uptodate.com/contents/causes-presentation-and-evaluation-of-sellar-masses on February 11, 2026.
Snyder PJ. Clinical manifestations and diagnosis of gonadotroph and nonfunctioning pituitary adenomas. UpToDate. 2026. Accessed at https://www.uptodate.com/contents/clinical-manifestations-and-diagnosis-of-gonadotroph-and-nonfunctioning-pituitary-adenomas on February 11, 2026.
Last Revised: May 8, 2026
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.


