Surgery for Pituitary Tumors
Surgery is the main treatment for many pituitary tumors. How the surgery is done and how well it works depends on several factors, including the type of tumor, its size and location, and if it has grown into nearby structures.
In general, smaller pituitary tumors are easier to treat with surgery. The larger and more invasive the tumor, the less likely it is that the tumor can be removed completely. Side effects also tend to be more likely after surgeries that remove larger, invasive tumors.
Planning surgery
Image guidance with MRI or CT scans will most likely be done before surgery to learn as much as they can about the tumor and nearby structures.
Image guidance helps doctors know:
- How big the tumor is
- Exactly where it is in the pituitary gland
- Whether it has spread beyond the pituitary gland
- Where important nearby structures are
This helps plan the best way to do the surgery and gives an idea of how likely it is that the tumor can be removed completely.
Transsphenoidal surgery
This is the most common way to remove pituitary tumors. Transsphenoidal surgery is done through the sphenoid sinus, a hollow space in the skull behind the nasal passages and below the brain. The back wall of the sinus is just below the pituitary gland.
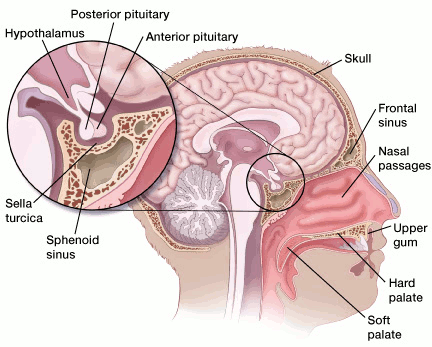
Who does the surgery
This surgery is often done by a team of surgeons that includes a neurosurgeon and an otolaryngologist, also known as an ear, nose, and throat (ENT) doctor or head and neck surgeon.
How it’s done
To reach the pituitary, the surgeon first makes a small cut deep inside the nose and then opens the bony walls of the sphenoid sinus with small surgical instruments. Other small tools are then passed through the opening to remove the tumor.
The surgeon can look at the tumor and nearby structures with an endoscope, a thin tube with a camera at the tip. The surgeon often uses a neuronavigation system, in which the surgical tools are virtually ‘attached’ to preoperative MRI or CT images. This lets the surgeon see the exact position of the tools in relation to the tumor and important nearby structures during the operation.
Important considerations
No part of the brain is touched during transsphenoidal surgery, so the chance of damaging the brain is very low. There are fewer side effects with this approach than with a craniotomy, and there's no visible scar.
When this surgery is done by an experienced neurosurgeon and the tumor is small (a microadenoma), the chances that it can be removed completely are high.
If the tumor is large or has grown into the nearby structures such as nerves, brain tissue, or the tissues covering the brain, the chances of removing the tumor completely are lower, and the chance of damaging nearby brain tissue, nerves, and blood vessels is higher.
Craniotomy
If the pituitary tumor is larger or more complicated, a craniotomy might be needed. This surgery is done through an opening in the front of the skull, off to one side. The surgeon has to work carefully beneath and between the lobes of the brain to reach the tumor.
Important considerations
A craniotomy has a higher chance of brain injury and other side effects than transsphenoidal surgery for small tumors, but it’s safer for large and complex tumors because the surgeon is better able to see and reach the tumor as well as nearby nerves and blood vessels.
Rarely, if a tumor is very large or has spread to nearby tissues, both types of surgery might be used at the same time to try to remove all of it.
Possible side effects of surgery
Some complications can occur during or after any type of surgery. These are rare, but they can happen. They include:
- Bleeding
- Infections
- Reactions to anesthesia (the drugs that make you sleep during surgery)
Risks and side effects of pituitary surgery
You will be watched closely after surgery, and your blood levels of hormones and other important substances will be checked often. Talk to your doctor about what you should watch for and what you should do if you have any problems.
Sinus headaches and congestion can occur for up to 2 weeks after transsphenoidal surgery.
Meningitis is inflammation of the meninges (the thin protective layers covering the brain). During transsphenoidal surgery, a temporary opening between the nasal passages and the brain is created. Until this heals, a person can get meningitis.
Leakage of cerebrospinal fluid (CSF, the fluid that bathes and cushions the brain) out of the nose can occur due to damage to the meninges. The chance of this happening depends on the size and type of tumor.
Arginine vasopressin deficiency, formerly known as diabetes insipidus, happens when not enough vasopressin is released by the posterior pituitary. This might occur right after surgery, but it usually improves on its own within a few weeks. If it doesn't, it might need to be treated with a desmopressin nasal spray.
Symptoms from a lack of pituitary hormones can occur due to damage to other parts of the pituitary. This is rare after surgery for small tumors, but it might be unavoidable when treating some larger tumors. Low hormone levels after surgery can be treated with medicines to replace certain hormones normally made by the pituitary and other glands.
Vitamin and mineral levels might change after surgery. If so, you might need supplements for a while. For instance, potassium levels often drop, so you might need to get it IV (in a vein) right after surgery.
Possible damage to nearby structures might occur because surgery for pituitary tumors is done in a very small space that is surrounded by important structures. Surgeons are extremely careful to limit any problems both during and after surgery. Still, very rarely, pituitary surgery might result in damage to the large arteries, brain tissue, or nerves near the pituitary. This could result in complications such as brain damage, stroke, or vision problems.
More information about surgery
For more general information about surgery as a treatment for cancer, see Cancer Surgery.
To learn about some of the side effects listed here and how to manage them, see Managing Cancer-related Side Effects.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Alzhrani G, Sivakumar W, Park MS, Taussky P, Couldwell WT. Delayed complications after transsphenoidal surgery for pituitary adenomas. World Neurosurg. 2018 Jan;109:233-241.
Graillon T, Castinetti F, Fuentes S, et al. Transcranial approach in giant pituitary adenomas: results and outcome in a modern series. J Neurosurg Sci. 2017 Jan 12.
Kuo JS, Barkhoudarian G, Farrell CJ, et al. Congress of Neurological Surgeons Systematic Review and Evidence-Based Guideline on Surgical Techniques and Technologies for the Management of Patients With Nonfunctioning Pituitary Adenomas. Neurosurgery. 2016 Oct;79(4):E536-8.
Lillehei KO, Travers S, Barkhoudarian G, et al. Congress of Neurological Surgeons Systematic Review and Evidence-Based Guidelines for the Role of Surgery for Patients With Functioning Pituitary Adenomas. Neurosurgery. 2025 Aug 15;97(3S):S24-S35.
National Cancer Institute. Pituitary Tumors Treatment (PDQ®)–Health Professional Version. 2024. Accessed at https://www.cancer.gov/types/pituitary/hp/pituitary-treatment-pdq on March 2, 2026.
Swearingen B. Transsphenoidal surgery for pituitary adenomas and other sellar masses. UpToDate. 2026. Accessed at https://www.uptodate.com/contents/transsphenoidal-surgery-for-pituitary-adenomas-and-other-sellar-masses on February 24, 2026.
You L, Li W, Chen T, et al. A retrospective analysis of postoperative hypokalemia in pituitary adenomas after transsphenoidal surgery. Peer J. 2017;5:e3337.
Last Revised: May 8, 2026
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.


