ACS Research News
Healthy Lifestyle Improves Survival from Obesity-Related Cancers
Published on: June 24, 2025
CPS-II Nutrition data shows that people with obesity-linked cancers lower their risk of death by sticking with the ACS Nutrition & Physical Activity Guideline.
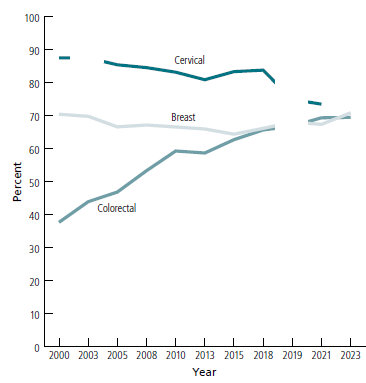
Not Enough Females Are Being Screened for Cervical Cancer
Published on: April 25, 2025
Cancer Prevention & Early Detection report says cervical cancer prevention needs urgent attention. Good news: Fewer people smoke than ever before.
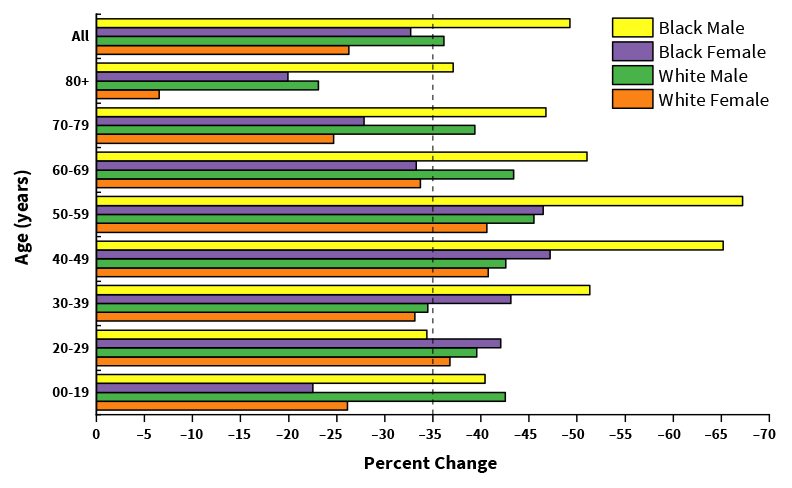
New Study Calls for Action to Reverse Course of Racial Disparities
Published on: February 24, 2025
Stark racial inequities in cancer incidence and survival spur the need for scientists, clinicians, and policymakers to unite and drive for meaningful change.