Cancer Connections
Cancer News, Stories, and Conversations
Our team of experts brings you cancer-related news, features, and survivor stories.
Published on: May 14, 2026
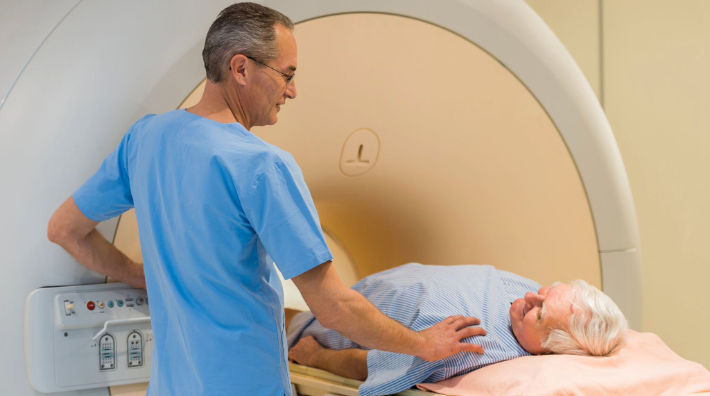
Most experts don’t recommend full-body MRIs as a way to detect cancer early for the general public. Get the facts about these scans, which can be pricey and cause anxiety.
Published on: May 7, 2026
Waiting to get tests and their results can cause a stressful feeling called scanxiety. Learn several methods to help manage this stress.
Published on: April 29, 2026
A Hope Lodge guest, Neil Erickson, turns sticky notes into messages of hope while facing cancer treatment in Houston.
Published on: April 23, 2026
Lymphedema, a swelling in the head and neck, can be a side effect of some cancers and cancer treatments. Learn more about how to cope with lymphedema.
Published on: April 22, 2026
After a lung cancer diagnosis, Duane Steiner found hope through a clinical trial and Hope Lodge, using his journey to advocate for cancer research.
Published on: April 16, 2026
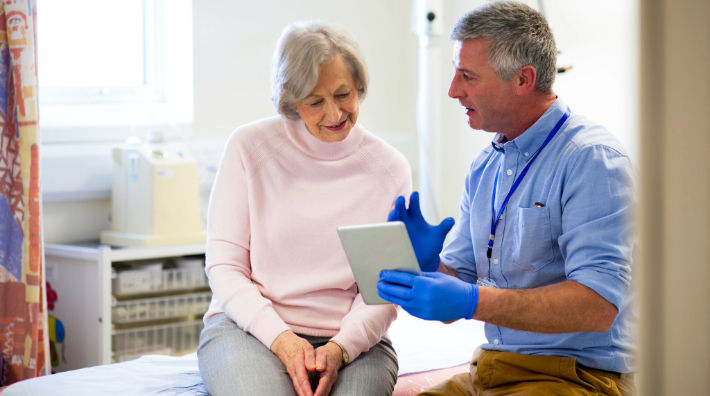
With simple tests and questions, geriatric assessments can help improve cancer care for people 65 and up. Learn more about these assessments.
Published on: April 9, 2026
A common problem during cancer treatment is fatigue, but research shows walking can help you get your energy back. Get tips to make walking work for you.
Published on: March 26, 2026
GLP-1 medicines are FDA-approved to treat type 2 diabetes and obesity. Find out more about what studies show about how they can affect cancer risk.