Nasopharyngeal Cancer
If you have nasopharyngeal cancer or are close to someone who does, knowing what to expect can help you cope. Here you can find out about nasopharyngeal cancer, including risk factors, symptoms, how it's found, and how it's treated.
About nasopharyngeal cancer
Nasopharyngeal cancer starts in the nasopharynx, the upper part of the throat behind the nose and near the base of the skull.
It is one of many different types of head and neck cancers. Each type is named depending on where the cancer starts. Ask your cancer care team to explain or show you exactly where your cancer is. You can also explore the 3D interactive model below.
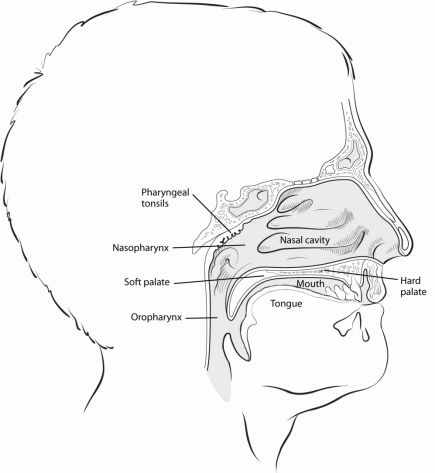
The nasopharynx
The nasopharynx is a box-like chamber about 3/4 of an inch (2 cm) wide and 1½ inches (4 cm) long. It lies just behind the nasal cavity and above the soft part of the roof of the mouth (soft palate). The nasopharynx is in the upper part of the throat (pharynx). The oropharynx is just below the nasopharynx and the hypopharynx is just below the oropharynx.
The nasopharynx serves as a passageway for air traveling from the nose to the throat.
Types of nasopharyngeal tumors
Several types of tumors can develop in the nasopharynx. Some of these tumors are benign (not cancer) and some are malignant (cancer).
Nasopharyngeal carcinoma (NPC)
Nasopharyngeal carcinoma (NPC) is the most common cancer of the nasopharynx. Carcinomas are cancers that start in epithelial cells, which are cells that line the surface of the body's organs.
There are 3 different types of NPC, as classified by the World Health Organization (WHO). They all start from epithelial cells that line the nasopharynx, but the cells of each type of NPC look different when they are examined closely in the lab.
- Keratinizing squamous cell carcinoma is the most common type of NPC in places with low rates of the disease, like the US.
- Non-keratinizing carcinoma is further divided into differentiated carcinoma and undifferentiated carcinoma. Non-keratinizing undifferentiated carcinoma is the most common type in areas with high rates of NPC. It is often associated with Epstein-Barr virus (EBV).
- Basaloid squamous cell carcinoma is a rare and very aggressive type of NPC.
Treatment is the same for all types of NPC. When doctors predict a person's outlook, the stage of their cancer (how far it has grown and spread) is often more important than the type of NPC they have.
Other cancers in the nasopharynx
Other types of cancers can also be found in the nasopharynx.
Lymphomas: About 5% of cancers that start in the nasopharynx are lymphomas. Lymphoma is a cancer of the lymphocytes, a type of immune system cell found throughout the body, including in the nasopharynx. See Non-Hodgkin Lymphoma.
Sarcomas and melanomas: Less than 5% of cancers that start in the nasopharynx are sarcomas or melanomas. Unlike NPCs, these cancers don't start in epithelial cells. See Soft Tissue Sarcoma and Melanoma Skin Cancer for more on these.
Salivary gland-type cancers: A small percentage of cancers that start in the nasopharynx are salivary gland-type tumors. These cancers develop from the minor salivary glands located in the lining of the nasopharynx, rather than from the surface epithelial cells. Examples include mucoepidermoid carcinoma and adenoid cystic carcinoma. See Salivary Gland Cancer to learn more.
Benign nasopharyngeal tumors (not cancerous)
Benign nasopharyngeal tumors are rare and tend to develop in children and young adults. They are not cancerous and don’t spread to other parts of the body. Usually, they are not life-threatening.
These tumors include:
- Tumors or malformations of the vascular (blood-carrying) system, such as angiofibromas and hemangiomas
- Benign tumors of minor salivary glands within the nasopharynx
Benign nasopharyngeal tumors don't always need treatment. When they do, the treatment is not the same as for nasopharyngeal cancer. If you have a benign tumor, ask your health care team what to expect.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Chang ET, Ye W, Zeng YX, Adami HO. The Evolving Epidemiology of Nasopharyngeal Carcinoma. Cancer Epidemiol Biomarkers Prev. 2021;30(6):1035-1047. doi:10.1158/1055-9965.EPI-20-1702.
Leeman JE, Katabi N, Wong RJ, Lee NY and Romesser PB. Ch. 65 - Cancer of the Head and Neck. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa. Elsevier; 2020.
Müller E, Beleites E. The basaloid squamous cell carcinoma of the nasopharynx. Rhinology. 2000 Dec;38(4):208-11.
WHO Classification of Tumours: Head and Neck Tumours, 5th ed, IARC Press, 2024. Vol 9.
Last Revised: March 3, 2026
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
This information is possible thanks to people like you.
We depend on donations to keep our cancer information available for the people who need it most.









