The ACA's Effect on Access to Cancer Screening and Care — The First 10 Years
When the Patient Protection and Affordable Care Act (ACA), or Obamacare, was signed into law on March 23, 2010, it was a historic moment — in fact, it was the biggest change to US health care since Medicare and Medicaid were launched in 1965. Over the past 10 years, the ACA has lowered the number of uninsured people living in the US, including people with pre-existing health conditions, and made many preventive services free. It has truly transformed the US healthcare system. So what, specifically, has its effect been on cancer — from prevention and screening to diagnosis, treatment, and survivorship? How has Obamacare improved life for cancer patients?
A team of researchers at the American Cancer Society (ACS) tracked the answers to these questions by reviewing a variety of studies that looked at how the ACA impacted access to health care for people with cancer. “We found that 3 parts of the ACA have been studied the most so far,” said Jingxuan Zhao, MPH, who lead the research team.
- Allowing young people to stay on their parents’ health insurance until age 26 (called dependent coverage expansion)
- Allowing for Medicaid expansion, which provides health insurance coverage to people with low incomes, to cover more people in some states
- Making many preventive health services — including cancer screenings like colonoscopies and mammograms — available at no extra out-of-pocket cost for people with most types of health insurance (also known as elimination of cost-sharing for preventive services).
“These parts of the ACA have significantly helped people who are trying to prevent cancer or detect it early. They have also helped cancer patients,” Zhao said. In their review, the researchers also highlighted areas where there are gaps in data and in research, as well as some changing policy issues — like work requirements for Medicaid — that may affect access to cancer care. The study was published in CA: A Cancer Journal for Clinicians.
Improving Cancer Care for Young Adults Ages 19 to 26
Raising the age for young adults to stay on their parents’ health insurance from age 19 to 26 was one of the first parts of the ACA that took effect in 2010, so researchers have data from a number of years to study.
Before the ACA, the age group most likely to be uninsured were 18 to 24. In 2009, for example, nearly 9.7 million didn’t have health insurance. That changed significantly after the ACA was introduced. By 2018, the number of uninsured people in this age group dropped to 4.7 million, and more 19- to 25-year-old people diagnosed with cancer had health insurance than they did before the ACA.
“We know that having health insurance is linked with improved access and quality of cancer care,” said Robin Yabroff, PhD, senior scientific director of the ACS health services research team. Being able to stay on their parents’ health insurance meant new cancer patients were more likely to be diagnosed early, or at an early stage, before the cancer had grown and spread.
An early diagnosis for any type of cancer may allow for less extensive treatment, with fewer side effects and fewer long-term health issues according to Xuesong Han, PhD, an ACS senior principal scientist. “That can have a huge, positive effect on patients and families,” she said.
One study found a significant decrease in late-stage cervical cancer diagnosis for women 21 to 25 years old after the ACA took effect compared to 26- to 34-year-old women, who were not eligible to remain on their parents’ health insurance.
There was also evidence of improvement in some types of cancer prevention and cancer care for young adults.
- Better cervical cancer prevention. More women 19- to 25-years old got vaccinated for HPV compared to the same age group before the ACA. HPV infection is the most important risk factor for developing cervical cancer. While getting the HPV vaccine as a young girl is an important step toward preventing most types of cervical cancer, young adult women who weren’t vaccinated or who didn’t finish the series of vaccines at an earlier age can still be vaccinated up to age 26, Han said.
The data was less clear on Pap testing. Cervical cancer screening was recommended for young women starting at age 21. One study didn’t find much change in Pap testing rates. But Han said that’s because there were some changes to the guidelines for cervical cancer screening at about the same time, including the recommendation to start screening at a later age and with less frequent Pap testing. So, it’s hard to tell if there was an impact on cervical cancer screening in this age group because of the ACA. “That meant we didn’t have the same information to compare before and after more young adults had health insurance,” she said. - More age-appropriate treatment for cervical cancer. After the ACA, more women ages 21 to 25 diagnosed with cervical cancer had treatment that preserved their fertility.
- Higher quality treatment for colorectal cancer. Another ACS study found that some patients between 19 to 25 with certain types and stages of colorectal cancer were more likely to get chemotherapy after surgery, which lowers the chance of the cancer coming back.
It’s still true that young adults get cancer less often than older adults. But evidence from the past couple of decades shows that young adults are being diagnosed more often with certain cancers. And cancer survival rates in young adults aren’t improving as much as those in children and older adults.
“To see improvements in survival, young adults will need to get recommended cancer screenings and high-quality cancer treatment—and for most people, that’s only feasible with health insurance,” Han said.
Expanding Medicaid Allows Health Insurance Coverage To Be More Equitable
“Poverty can adversely affect health,” said Yabroff. Historically, poorer people with cancer in the US don’t do as well as those with more money, largely because they frequently lack health insurance, she said.
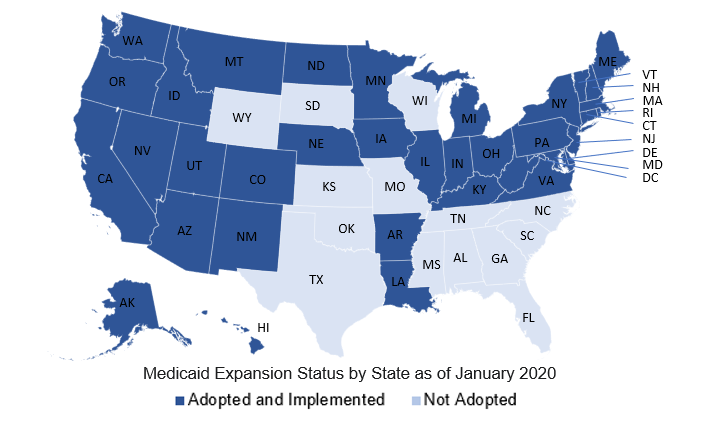
Starting in 2014, Medicaid expansion helped states pay the costs for increasing the number of people with lower incomes who qualify for Medicaid. Specifically, it allowed adults without dependent children to be eligible for Medicaid, and it raised the amount of money people could have and still qualify. Not every state decided to make these changes. Currently there are 37 expansion states (including Washington, DC) with 14 that have not yet adopted expansion.
Compared to states that didn’t expand Medicaid, expansion states had:
- More cancer preventive care. More people with low incomes had a colonoscopy to screen for colorectal cancer, and more women had a Pap test to screen for cervical cancer.
- Fewer people diagnosed with cancer who didn’t have health insurance. Although the number of new cancer patients 18 to 64 years old without health insurance dropped overall, it dropped more in expansion states.
- More cancers found at an early stage. People in expansion states were more likely to be diagnosed with cancer when it was still at an early stage. Screening increases the chances of detecting certain cancers early, when they might be easier to treat.
- More cancer survivors with health insurance. The percentage of uninsured survivors dropped from 13.1% in 2013 to 5.5% in 2015 in expansion states. Some cancer survivors are at risk of having additional health problems—and second cancers. “So, it’s really important that they’re able to have health insurance, can afford to see their doctors, and get the care that’s recommended for them,” Han said.
- More equitable cancer care. Medicaid expansion helped reduce some disparities in health insurance coverage for cancer care. Disparities are health differences closely linked with economic, social, or environmental disadvantage. For example, people with lower socioeconomic status, which is measured by a person’s social, financial, and work statuses, have higher cancer death rates than those with higher socioeconomic status.
Through the ACA, the number of uninsured cancer patients in expansion states declined more for racial and ethnic minorities, people with low incomes, and people who live in rural areas. In nonexpansion states, declines in insurance rates were similar across those socioeconomic groups. “In nonexpansion states, the same disparities in health insurance in cancer patients that existed before the ACA didn’t change much after it,” Han said.
Questions About Free Preventive Care
Eliminating cost-sharing for preventive services meant most private insurance plans, as well as Medicare and Medicaid, are required to cover recommended preventive services free of charge. Pre-ACA copays, coinsurance, or deductibles that insured people paid out-of-pocket for getting many types of preventive care — including cancer screenings and smoking cessation — were eliminated.
Understanding how much this provision has helped prevent or detect cancer early hasn’t been easy. “Some studies showed an increase in colorectal cancer screening, mammography, and Pap tests — but others showed little or no change,” said Stacy Fedewa, PhD, an ACS senior principal scientist.
It could be that cancer screening is simply not a top priority for people who recently gained health insurance. “Some people may have health problems that need to be taken care of before they even think about preventive care, including getting screened for cancer,” Fedewa said. Over time, as people have continuous health insurance coverage, the screening rates may rise, she said.
The Full Picture of How the ACA Affects Cancer Is Still Emerging
Different starting dates for parts of the ACA mean that data are not yet available to fully evaluate all parts of the law and its longer-term effects. There have been very few ACA studies about many parts of cancer care —treatment, survivorship care, and end-of-life care. “We want to study how long it takes people to get treated after they’re diagnosed with cancer, whether they’re able to complete their treatment, whether more people survive — and whether they’re able to get the right care as survivors,” Yabroff said.
Changing policy issues affect the ACA, too, she said. High-deductible health plans and work requirements for Medicaid are just some of the new, yet-to-be-evaluated elements that may threaten the improvements that have been made in health care.
Everything ACS researchers learn and publish is shared with the American Cancer Society Cancer Action Network (ACS CAN), the nonprofit, nonpartisan advocacy affiliate of the American Cancer Society. “We provide evidence about the effect health insurance has on cancer, and ACS CAN can use that information to help protect existing laws, advocate for cancer research funding, and influence development of new evidence-based health policies,” Yabroff said.
“That’s how ACS and ACS CAN worked together to help the ACA become law more than 10 years ago, and that’s what we’ll keep doing,” said Keysha Brooks-Coley, vice president, federal advocacy and strategic alliance for ACS CAN. “Because defeating cancer depends on improving access to affordable, quality health care, we need policymakers at all levels of government to prioritize access to health coverage that gives people a fair and just opportunity to prevent, detect, and treat cancer, no matter where they live,” she said.
ACS will continue to conduct research to gain more knowledge about how the ACA may improve access to, and the quality of, care for cancer patients and survivors, Yabroff added.
Last Revised: March 16, 2026



