Your gift is 100% tax deductible.
Brain Tumors in Children
Combined, brain tumors are the most common solid tumor in children and teens. About 4,9000 children are diagnosed with a brain tumor each year in the United States. (For information on adult tumors see Brain and Spinal Cord Tumors in Adults.)
About childhood brain tumors
Brain tumors are clusters of abnormal cells in the brain. The brain is made up of multiple types of cells, each with its own function. Brain tumors are a group of different types of tumors that can have distinct symptoms and respond differently to treatment based on several factors, including:
- The type (or types) of brain cell the tumor started from
- The location of the brain tumor
- The grade of the tumor (how fast the tumor cells appear to be growing)
- Gene changes present in the tumor cells or the presence of a family cancer syndrome
- The child’s age
- Any signs or symptoms of damage caused by the tumor
If you or your child has a brain tumor, knowing what to expect may be helpful. Here you can find out more about brain tumors that can affect children and young adults, including risk factors, symptoms, and how tumors may be found and treated.
Are brain tumors always cancer?
Tumors can be non-malignant (not cancer) or malignant (cancer):
- Non-malignant tumors do not invade nearby tissues or spread to distant areas. They grow slowly, so they are almost never life-threatening in other parts of the body.
- Malignant tumors (cancers) are more dangerous because they can spread to other parts of the body and grow quickly.
- Brain tumors rarely spread to other parts of the body, but many of them are considered malignant because they can spread through the central nervous system (brain and spinal cord tissue).
In most other parts of the body, it’s very important to distinguish between non-malignant and malignant tumors. But in the brain, both non-malignant and malignant tumors can be dangerous, so the difference between them is less important. For this reason, doctors often talk about “brain tumors” instead of “brain cancer.”
How serious are brain tumors and spinal cord tumors?
Brain tumors rarely spread to other parts of the body, but they can still be very serious. Even non-malignant tumors can press on and destroy normal brain tissue as they grow, which can lead to serious or sometimes life-threatening damage.
The main concerns with brain and spinal cord tumors are:
- How fast they grow
- Where they are located and what important structures are nearby
- How readily they can spread through the rest of the brain or spinal cord
- Whether they can be removed or treated and not come back
Both non-malignant and malignant tumors in the brain and spinal cord can be life-threatening.
Are brain and spinal cord tumors different in children?
Brain and spinal cord tumors in children and teens tend to be different from those in adults. They often form in different places, develop from different cell types, and may have a different treatment and prognosis (outlook).
To learn more about the differences between childhood cancers and adult cancers in general, see Childhood Cancer.
About the brain and spinal cord
The brain and spinal cord are made up of many different types of cells, including:
- Neurons
- Glial cells
- Endothelial cells
- Neuroectodermal cells
- Meningeal cells
Tumors can form in almost any kind of brain cell or tissue, but tumors of the glial, neuroectodermal, and meningeal cells are more common. Some tumors have more than 1 type of brain cell in them.
Neurons
Neurons are brain cells that create thoughts, memories, emotions, speech, muscle movements, and sensations by sending chemical and electrical signals through their nerve fibers (axons). Axons in the brain are usually short, while those in the spinal cord can be several feet long. Unlike most cells that can grow and divide to repair damage from an injury or disease, most neurons in the brain and spinal cord stop dividing about 1 year after birth. Neurons do not usually form tumors, but they can be damaged by tumors that grow nearby.
Glial cells
Glial cells are the supporting cells of the brain. Most brain and spinal cord tumors develop from glial cells. As a group, these tumors are called gliomas, but there are different types depending on what type of glial cell they start from. (For example, an astrocytoma is a tumor of astrocytes.)
There are a few main types of glial cells:
- Astrocytes help support and nourish neurons. When the brain is injured, astrocytes form scar tissue that helps repair the damage.
- Oligodendrocytes make myelin, a fatty substance that surrounds and insulates the nerve cell axons of the brain and spinal cord. This helps neurons send electrical signals through the axons.
- Ependymal cells line the ventricles (fluid-filled areas) within the central part of the brain and form part of the pathway through which cerebrospinal fluid (CSF) flows.
Microglia are infection-fighting immune cells in the central nervous system. They are not truly glial cells and rarely form tumors.
Neuroectodermal cells
Neuroectodermal cells are very early forms of nervous system cells that are involved in brain cell development, like glial cells. They are found throughout the brain. The most common tumors that come from these cells develop in the cerebellum and are called medulloblastomas.
Endothelial cells
Endothelial cells line the blood-brain barrier. The normal blood-brain barrier protects the brain from toxins and infections, while letting certain nutrients and proteins enter.
When a brain tumor forms, endothelial cells can play an important role in blocking the immune system, which might normally kill tumor cells. Endothelial cells also help build blood vessels. Nutrients and oxygen in the blood are important for tumors to be able to grow.
Meningeal cells
Meningeal cells make up layers of tissue that cover and protect the brain and spinal cord, called the meninges. The meninges help form the spaces CSF travels through. Brain tumors that start in the meninges are called meningiomas.
Where do brain tumors form?
Where a tumor is in the brain can affect what symptoms it causes, as well as which treatments might be best. Brain tumors in younger people are more likely to start in the lower parts of the brain, such as the cerebellum and brain stem, than they are in adults. Sometimes this area of the brain is referred to as the posterior fossa. But they can start in the upper parts of the brain as well.
The main areas of the brain include the cerebrum, cerebellum, and brain stem. Each area has a special function.
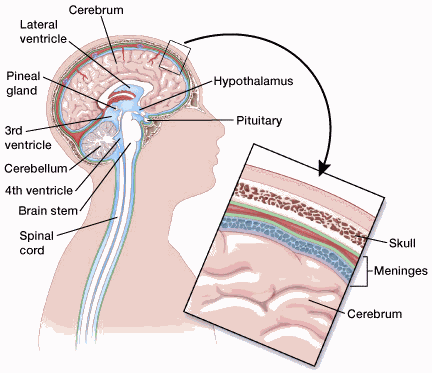
Cerebrum
The cerebrum is the large, outer part of the brain. It is made up of 2 hemispheres (halves) and controls reasoning, thought, emotion, and language. It is also responsible for muscle movements (like those involved in throwing a ball, walking, chewing, etc.) and the senses such as vision, hearing, smell, touch, and pain.
Cerebellum
The cerebellum lies under the cerebrum at the back part of the brain. It helps coordinate movement and balance.
Brain stem
The brain stem is the lower part of the brain that connects to the spinal cord. It has bundles of very long nerve fibers that carry signals controlling muscles and sensation or feeling between the cerebrum and the rest of the body. Special centers in the brain stem also control vital functions like breathing and keeping the heart pumping. In addition, most cranial nerves (described below) start in the brain stem. The cranial nerves affect how the face, eyes, ears, nose, mouth, throat, and tongue move and work, so tumors affecting the brain stem can cause problems in these areas.
The brain stem is divided into 3 main parts:
- Midbrain
- Pons
- Medulla oblongata
Because the brain stem is a small area that is essential for life, it might not be possible to safely remove tumors in this area with surgery.
Pituitary gland and hypothalamus
The pituitary is a small gland at the middle of the base of the brain. It is connected to another part of the brain, called the hypothalamus. Both areas make hormones that help regulate functions like body temperature, metabolism, puberty and sex hormone production, and growth.
The growth of tumors in or near the pituitary or hypothalamus, as well as surgery and/or radiation therapy in this area, can affect these functions. For example, tumors starting in the pituitary gland sometimes make too much of a certain hormone, which can cause problems. On the other hand, a child may have low levels of 1 or more hormones after treatment and may need to take hormones to replace what is missing.
Pineal gland
The pineal gland is a small hormone-producing gland that sits between the 2 major halves of the brain. It makes melatonin, a hormone that controls sleep. A specific tumor, called a pineoblastoma, can grow in this area.
Spinal cord
The spinal cord has bundles of very long nerve fibers that carry signals that control muscles, sensation or feeling, and bladder and bowel control. Tumors in this area may cause an area to feel numb or not move properly and can affect the ability to pass urine or stool normally. Some tumors affecting the spinal cord start from the brain cells, and others may spread to the spinal cord from other parts of the body or press on it from the outside.
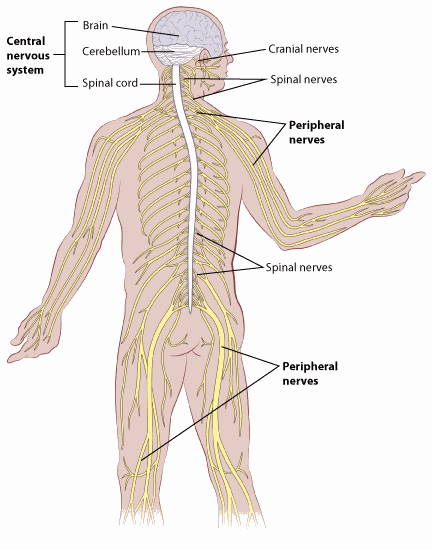
Cranial nerves
The cranial nerves extend directly out of the brainstem. These nerves carry signals directly between the brain and the face, eyes, ears, nose, mouth, throat, and tongue.
The most common cranial nerve tumors in children are optic gliomas, which start in the optic nerve (the large nerve that runs between the brain and each eye). These tumors are seen more often in people with neurofibromatosis type 1.
If a brain tumor grows near a cranial nerve, it can press on the nerve, causing problems like double or blurry vision, balance issues, changes in facial appearance, or difficulty chewing and swallowing.
Cerebrospinal fluid (CSF)
CSF is fluid that surrounds the brain, providing nourishment and support. The CSF is a common place for some malignant brain tumors to spread. People with malignant brain tumors, such as medulloblastoma, may need a lumbar puncture to remove a small amount of CSF to test for cancer cells.
Ventricles
The ventricles are the spaces in the brain where CSF collects. In some cases, tumors can grow into or push on these spaces, blocking the flow of fluid. This can cause increased pressure in the brain and lead to symptoms like severe headaches and vomiting.
Choroid plexus
The choroid plexus is the area of the brain within the ventricles that makes CSF. Tumors that start here include choroid plexus papillomas and choroid plexus carcinomas.
Meninges
The meninges cover and protect the brain and spinal cord. They also help form the spaces through which CSF travels. Brain tumors that start in the meninges are called meningiomas.
Blood-brain barrier
The inner lining of the small blood vessels (capillaries) in the brain and spinal cord creates a very selective barrier between the blood and the tissues of the central nervous system. The blood-brain barrier normally supports and protects the brain, keeping harmful chemicals out. But it also keeps out many chemotherapy drugs, which can limit their usefulness in treating brain tumors.
Quick Guides
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Alencastro Veiga Cruzeiro G, Rota C, Hack OA, Segal R, Filbin MG. Understanding the epigenetic landscape and cellular architecture of childhood brain tumors. Neurochem Int. 2021;144:104940.
Clark V, Gunel JM, Gunel M. Section 10: Neoplasms of the central nervous system. In: DeVita VT, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 10th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2015.
Dorsey JF, Salinas RD, Dang M, Alonso-Basanta M, Judy KD, Maity A, et al. Chapter 63A: Central Nervous System; Cancer of the Central Nervous System. In: Niederhuber JE, Armitage JO, Dorshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa. Elsevier: 2019.
National Cancer Institute. Childhood Astrocytomas, Other Gliomas, and Glioneuronal/Neuronal Tumors. Accessed at https://www.cancer.gov/types/brain/hp/child-astrocytoma-glioma-treatment-pdq on August 28, 2025.
National Cancer Institute. Childhood Brain and Spinal Cord Tumors Summary Index (PDQ). 2023. Accessed at https://www.cancer.gov/types/brain/hp/child-brain-treatment-pdq on August 28, 2025.
National Cancer Institute. Childhood Central Nervous System Atypical Teratoid/Rhabdoid Tumor Treatment (PDQ). 2025. https://www.cancer.gov/types/brain/hp/child-cns-atrt-treatment-pdq on August 28, 2025.
Price M, Ballard CAP, Benedetti JR, Kruchko C, Barnholtz-Sloan JS, Ostrom QT. CBTRUS Statistical Report: Primary Brain and Other Central Nervous System Tumors Diagnosed in the United States in 2018-2022. Neuro Oncol. 2025;27(Supplement_4):iv1-iv66.
Robinson GW, Kaste SC, Chemaitilly W, et al. Irreversible growth plate fusions in children with medulloblastoma treated with a targeted hedgehog pathway inhibitor. Oncotarget. 2017;8(41):69295-69302. Published 2017 Sep 1.
Last Revised: February 9, 2026
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
This information is possible thanks to people like you.
We depend on donations to keep our cancer information available for the people who need it most.