Your gift is 100% tax deductible.
Hodgkin Lymphoma
If you or your child has Hodgkin lymphoma (Hodgkin disease), knowing what to expect can help you cope. Here you can learn all about Hodgkin lymphoma, including risk factors, symptoms, how it’s found, and how it’s treated.
About Hodgkin lymphoma
Hodgkin lymphoma is a type of cancer that begins in white blood cells called lymphocytes.
There are 2 main types of lymphocytes:
- B lymphocytes (B cells): B cells make proteins called antibodies to help protect your body from germs (bacteria and viruses).
- T lymphocytes (T cells): There are many types of T cells. Some T cells destroy germs or abnormal cells in your body. Other T cells help boost or slow the activity of other immune system cells.
Hodgkin lymphoma usually starts in B lymphocytes.
Lymphocytes make up most of your lymph system, also known as your lymphatic system. Your lymph system is part of your immune system, which helps fight infections and other diseases. Your lymph system also helps control the flow of fluids in your body.
Where in the body does Hodgkin lymphoma start?
Lymph tissue is in many parts of your body, so Hodgkin lymphoma can start almost anywhere, but:
- It most often starts in lymph nodes in the upper part of the body.
- The most common sites are in the chest, neck, or under the arms.
The main sites of lymph tissue are your spleen, bone marrow, thymus, adenoids and tonsils, and digestive tract.
Where does it spread?
Hodgkin lymphoma most often spreads through the lymph vessels from lymph node to lymph node. Rarely, late in the disease, it can invade the bloodstream and spread to other parts of the body, such as the liver, lungs, and/or bone marrow.
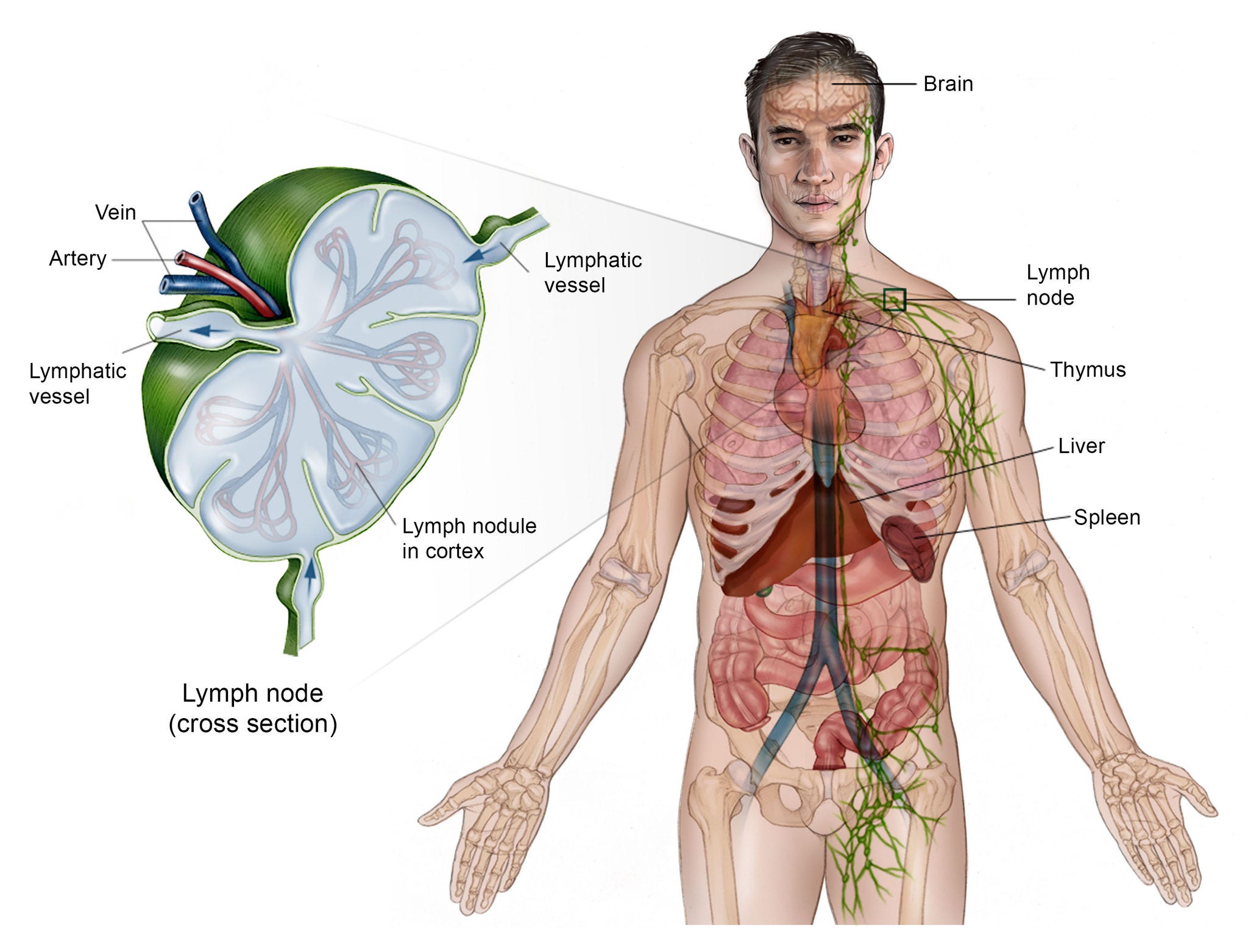
© American Society for Clinical Oncology. Used with permission.
How is Hodgkin lymphoma different from non-Hodgkin lymphoma?
There are 2 main types of lymphoma:
- Hodgkin lymphoma (HL)
- Non-Hodgkin lymphoma (NHL)
Both of these start in white blood cells called lymphocytes, but they come from different types of lymphocyte cells. They behave, spread, and respond to treatment differently, so it’s important to know which one you have.
This information is about Hodgkin lymphoma. To learn about NHL, see Non-Hodgkin Lymphoma.
Types of Hodgkin lymphoma
There are different types of Hodgkin lymphoma. These types can grow and spread differently and may be treated differently.
Classic Hodgkin lymphoma (cHL)
Classic Hodgkin lymphoma (cHL) accounts for more than 9 in 10 cases of Hodgkin lymphoma in developed countries.
The cancer cells in cHL are called Reed-Sternberg cells. These cells are usually an abnormal type of B lymphocyte. Enlarged lymph nodes in people with cHL usually have a small number of Reed-Sternberg cells with a lot of normal immune cells around them. These other immune cells cause most of the swelling in the lymph nodes.
Classic HL subtypes
This is the most common type of Hodgkin disease in developed countries. It accounts for about 7 out of 10 cases. It is most common in teens and young adults, but it can happen in people of any age. It tends to start in lymph nodes in the neck or chest.
This is the second most common type, found in about 4 out of 10 cases. It’s seen mostly in people with HIV infection. It’s also found in children or the elderly. It can start in any lymph node but most often occurs in the upper half of the body.
This subtype isn’t common. It usually occurs in the upper half of the body and is rarely found in more than a few lymph nodes.
This is a rare form of Hodgkin disease. It’s seen mainly in older people and those with HIV infection. It's more aggressive than other types of HL and likely to be advanced when first found. It's most often in lymph nodes in the abdomen (belly) as well as in the spleen, liver, and bone marrow.
Nodular lymphocyte-predominant Hodgkin lymphoma
Nodular lymphocyte-predominant Hodgkin lymphoma (NLPHL) accounts for about 5% of cases.
NLPHL usually starts in lymph nodes in the neck and under the arm. It can occur in people of any age and is more common in men than in women. This type of HL tends to grow more slowly and is treated differently from the classic types.
The cancer cells in NLPHL are called lymphocyte-predominant (LP) cells. You might also hear them called popcorn cells because they look like popcorn under the microscope.
Quick Guides
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Bartlett NL, Foyil KV. Chapter 105: Hodgkin lymphoma. In: Niederhuber JE, Armitage JO, Dorshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa. Elsevier: 2019.National Comprehensive Cancer Network, Clinical Practice Guidelines in Oncology (NCCN Guidelines®), Hodgkin Lymphoma, Version 2.2025 -- Jan 30, 2025. Accessed at www.nccn.org/professionals/physician_gls/pdf/hodgkins.pdf on July 10, 2025.
Younes A, Carbone A, Johnson P, Dabaja B, Ansell S, Kuruvilla J. Chapter 102: Hodgkin’s lymphoma. In: DeVita VT, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 10th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2015.
Last Revised: October 6, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
This information is possible thanks to people like you.
We depend on donations to keep our cancer information available for the people who need it most.










