Surgery for Oral Cavity and Oropharyngeal Cancer
Surgery is often the first treatment used for oral cavity (mouth) or oropharyngeal (throat) cancers. Several types of operations can be done, depending on the location and stage of the cancer. Surgery is most often used for small, early-stage mouth and throat cancers that haven't spread.
After the cancer is removed, reconstructive surgery might be done to help restore the appearance and function of the areas affected by the cancer or treatment.
Surgery for oral cavity and oropharyngeal cancers is often complex. People tend to have better outcomes if they’re treated at centers that have a lot of experience with head and neck cancers.
Surgery to remove the tumor (tumor resection)
In a tumor resection surgery, the entire tumor and a margin (edge) of normal-looking tissue around it are removed (resected). This margin of normal tissue around the tumor is taken out to reduce the chance of any cancer cells being left behind.
The type of surgery you need will depend on the location and size of your tumor.
Mohs surgery, also known as micrographic surgery, might be used to remove some cancers of the lip, such as those at the very edge of the lip.
The tumor is removed in very thin slices. Each slice is looked at right away under the microscope to see if it has cancer cells. Slices are removed and examined until no cancer cells are seen. This method reduces the amount of normal tissue removed with the tumor. The change in appearance caused by the surgery is limited.
Mohs surgery requires a surgeon trained in the technique and may take more time than a standard tumor resection.
Glossectomy may be needed to treat cancer of the tongue.
- Partial glossectomy: For smaller cancers, only part of the tongue (less than 1/3) may need to be removed.
- Total glossectomy: For larger cancers, the entire tongue may need to be removed.
A mandibulectomy, also called a mandibular resection, might be needed if the tumor has grown into the jawbone. For this operation, a surgeon removes all or part of the jawbone (mandible).
Partial-thickness mandibular resection (marginal mandibulectomy)
If the jawbone looks normal on imaging tests and there is no evidence the cancer has spread there, the bone may not need to be cut all the way through. In this operation, the surgeon removes only part or a piece of jawbone.
Segmental mandibulectomy
If the x-ray shows the tumor has grown into the jawbone, a large part of the jaw will need to be removed in an operation called a segmental mandibulectomy.
The removed piece of the mandible can then be replaced with a piece of bone from another part of the body, such as the lower leg, hip bone, or the shoulder blade. A metal plate or a piece of bone from a deceased donor may also be used to repair the bone.
If cancer has grown into the hard palate (front part of the roof of the mouth), all or part of the involved bone (maxilla) will need to be removed. This operation is called a maxillectomy or partial maxillectomy.
The surgery leaves a hole in the roof of the mouth which can be filled with a special prosthetic denture. This is created by a dentist with special training, called a prosthodontist. Other options to close this gap include a skin graft or a piece of muscle from the forearm or thigh.
Very rarely, surgery to remove large tumors at the base of the tongue or oropharynx may require removing tissue needed to swallow normally. As a result, food may enter the windpipe (trachea) and reach the lungs, where it can cause pneumonia.
When there is a high risk of this happening, the voice box (larynx) may also be removed during the same operation as the one to remove the cancer. Removal of the larynx is called a laryngectomy.
When your voice box is removed, your windpipe is attached to a hole (stoma) made in the skin in the front of your neck. You breathe and cough through this stoma, instead of through your mouth and nose. This is called a tracheostomy or trach.
If your voice box is removed, you will no longer be able to speak as you did before surgery. But you can learn other ways of speaking. See After Treatment for Oral Cavity or Oropharyngeal Cancer to learn more about voice restoration.
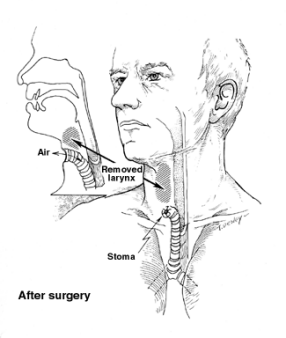
Laryngectomy
Trans-oral robotic surgery (TORS) can be used to remove certain cancers of the back of the throat and mouth. The surgeon sits at a control panel in the operating room and with the help of an attached camera moves robotic arms with small tools on them to cut out the tumor.
These newer robotic techniques may allow surgeons to completely remove throat cancers with less extensive operations and fewer side effects, compared to the more standard open surgeries.
If you plan to have this type of surgery, it's important that your surgeon and treatment center are experienced in this approach.
Surgery to remove lymph nodes
Cancers of the oral cavity and oropharynx often spread to the lymph nodes in the neck. Removing these lymph nodes and other nearby tissues is called a neck dissection or lymph node dissection. It is done at the same time as the surgery to remove the main tumor.
The goal of this surgery is to remove any lymph nodes known to contain cancer. Doctors sometimes recommend an elective lymph node dissection when there is no proof that the cancer has spread to the lymph nodes. This may be done if there is a high chance that the cancer has spread to the lymph nodes based on tumor size.
Sentinel lymph node biopsy
In some early-stage mouth and lip cancers, a sentinel lymph node biopsy might be done to test the lymph nodes for cancer before removing them. This should only be done at treatment centers by doctors with a lot of experience in the technique.
Types of neck dissection surgery
There are several types of neck dissection procedures. They differ in how much tissue is removed from the neck. The amount of tissue removed depends on the size of the primary cancer and how much it has spread to the lymph nodes.
- Partial or selective neck dissection: Only a few lymph nodes are removed.
- Modified radical neck dissection: Most lymph nodes on one side of the neck between the jawbone and collarbone are removed, as well as some muscle and nerve tissue.
- Radical neck dissection: Nearly all nodes on one side are removed, along with even more muscles, nerves, and veins.
Possible side effects
Side effects of a neck dissection can include numbness of the ear, weakness when raising the arm above the head, and weakness of the lower lip due to nerve damage from surgery.
Nerves heal slowly, so sometimes these side effects can improve over time. If more extensive surgery is needed, the side effects might be permanent. After any neck dissection procedure, physical therapy can help improve neck and shoulder movement.
Reconstructive surgery
If you have extensive surgery to remove your cancer, you may need further operations to help restore the structure of the affected areas.
For small tumors, the narrow edge of normal tissue removed along with the tumor is usually small enough that reconstructive surgery isn't needed. Removing larger tumors may cause defects in the mouth, throat, or neck that will need to be repaired.
Skin graft: Sometimes a thin slice of skin, taken from a thigh or another area, can be used to repair a small defect.
Flap surgery: More tissue may be needed to repair a larger defect. A piece of muscle with or without skin may be rotated from an area close by, such as the chest (pectoralis major pedicle flap) or upper part of the back (trapezius pedicle flap).
Other surgical options: Due to advances in microvascular surgery (sewing together small blood vessels under a microscope), there are many more options for reconstructing the oral cavity and oropharynx. Tissue from other areas of the body, such as the intestine, arm muscle, abdominal (belly) muscle, or lower leg bone may be used to replace parts of the mouth, throat, or jawbone.
Before you have extensive head and neck surgery, talk to your surgeon about your options for reconstruction.
Surgery to save or restore body function
A tracheostomy is a stoma (hole) made through the skin in the front of the neck and attached to the trachea (windpipe). It is done to help a person breathe.
Short-term tracheostomy
If your doctor expects a lot of swelling in your airway after your cancer is removed, they may create a short-term tracheostomy by using a small plastic tube to help you breathe more easily until the swelling goes down. This stays in place for a short time and is then removed (or reversed) when it's no longer needed.
Permanent tracheostomy
If the cancer is blocking your throat and is too big to remove completely, you may need a permanent tracheostomy, which is a permanent opening to connect a lower part of your windpipe to a stoma (hole) in the front of your neck. This is done to bypass the tumor and allow you to breathe more comfortably.
A permanent tracheostomy is also needed after a total laryngectomy.
Cancer in the oral cavity and oropharynx may keep you from swallowing enough food to stay well nourished. This can make you weak and make it harder to complete treatment. Sometimes the treatment itself can make it hard to eat enough. There are a few different types of feeding tubes that might be used in these situations.
Gastrostomy tube (G-tube)
A gastrostomy tube, or G-tube, is a feeding tube put through the skin and muscle of your abdomen (belly) and right into your stomach. Sometimes this tube is placed during an operation, but often it's put in place through endoscopy.
When the feeding tube is put in place through endoscopy, it's called a percutaneous endoscopic gastrostomy, or PEG tube. The tube is placed while you are sedated, using medicine to make you fall asleep. The doctor inserts a long, thin and flexible tube, called an endoscope, down your throat. The endoscope has a camera on the end, allowing the doctor to see inside your stomach. The feeding tube is then guided through the endoscope and to the outside of your body.
Once in place, the feeding tube can be used to put liquid nutrition right into your stomach. As long as you can still swallow normally, you can also eat regular food while you have this type of tube.
PEGs can be used for as long as needed. Sometimes these tubes are used for a short time to help keep you healthy and fed during treatment. They can be removed when you are able to eat normally.
Nasogastric feeding tube (NG tube)
If the swallowing problem is likely to be only short-term, another option is a nasogastric feeding tube (NG tube). This tube goes in through your nose, down your esophagus, and into your stomach. Special liquid nutrients are put in through the tube. Some people dislike having a tube coming out of their nose and prefer a PEG tube.
No matter which type of feeding tube you have, you and your caregivers will be taught how to use it. After you leave the hospital, home health nurses might visit to make sure you are comfortable with tube feedings.
If radiation is part of your treatment plan, you must have a dental evaluation before you begin. Depending on the radiation plan and condition of your teeth, some or even all of your teeth might need to be removed before radiation can start.
The teeth may be removed either by the head and neck surgeon or by an oral surgeon. If broken or infected (abscessed) teeth are left in and exposed to radiation, these teeth are very likely to cause problems such as infections and areas of necrosis (bone death) in the jaw.
If part of your jawbone (mandible) is removed and reconstructed with bone from another part of your body, the surgeon might place dental implants in the bone. Dental implants are hardware that prosthetic teeth can be attached to. The implants can be placed when your mandible is reconstructed or they can be placed later.
Possible risks and side effects of surgery
The risks and side effects of any surgery depend on the extent of the operation and your general health before the surgery. If you are considering surgery, your health care team will discuss the likely side effects with you beforehand. Be sure you understand how surgery may affect the way you look and how your body works.
General risks and side effects
All surgery carries some risk, including the possibility of blood clots, bleeding, infections, complications from anesthesia, and pneumonia. These risks are generally low but are higher with more complicated surgeries.
Most people will have some pain for a while after surgery, although this can usually be controlled with medicines. Rarely, some people do not survive surgery.
Impacts of specific surgeries
Most people can still speak if only part of their tongue is removed, but they often notice that their speech isn’t as clear as it once was. The tongue is important in swallowing, so this may also be affected. Speech therapy can often help with these problems.
When the entire tongue is removed, you lose the ability to speak and swallow. With reconstructive surgery and a good rehabilitation program, including speech therapy, some people may regain the ability to swallow and speak well enough to be understood.
After a laryngectomy to remove your voice box, leaves you without the usual means of speech. There are several ways to restore the voice. See After Treatment for Oral Cavity and Oropharyngeal Cancer to learn more about voice restoration.
After a laryngectomy, you breathe through a tracheostomy, which is a hole (stoma) placed in the front of your neck that connects to your trachea (windpipe).
The air you breathe in and out no longer passes through your nose or mouth, which normally helps moisten, warm, and filter the air, removing dust and other particles. The air reaching your lungs will be dryer and cooler. This can irritate the lining of the tracheostomy and can cause thick or crusty mucus to build up.
It's important to learn how to take care of your stoma.
You will need to use a humidifier over the stoma as much as possible, especially right after the surgery, until your airway lining has a chance to adjust to the drier air now reaching it.
You will also need to learn how to suction out and clean your stoma to help keep your airway open. Your health care team can teach you how to care for and protect your stoma, which includes precautions to keep water from entering your windpipe while showering or bathing, as well as keeping small particles out of your windpipe.
Some cancers of the head and neck are treated with operations that remove part of the facial bone structure. Because the changes that result are so visible, they can have a major effect on how people view themselves.
It’s important to talk with your health care team about these changes before you have surgery. This can help you prepare. You can also get an idea about the options available to you afterward.
Recent advances in reconstructive surgery and facial prostheses (human-made replacements) now give many people a more typical look, which can be a great help to self-esteem after this type of surgery.
More information about surgery
For more general information about surgery as a treatment for cancer, see Cancer Surgery.
To learn about some of the side effects listed here and how to manage them, see Managing Cancer-related Side Effects.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Baghel SS, Singhal P, Verma N, et al. Is thyroid excision mandatory with laryngectomy in carcinoma larynx? BMC Cancer 2020;20:700.
Cigna E, Rizzo MI, Greco A, et al. Retromolar trigone reconstructive surgery: prospective comparative analysis between free flaps. Ann Surg Oncol. 2015;22(1):272-278. doi:10.1245/s10434-014-3963-4.
Civantos FJ, Zitsch RP, Schuller DE, et al. Sentinel lymph node biopsy accurately stages the regional lymph nodes for T1-T2 oral squamous cell carcinomas: results of a prospective multi-institutional trial. J Clin Oncol 2010;28:1395-1400.
D’Cruz AK, Vaish R, Kapre N, et al; Head and Neck Disease Management Group. Elective versus therapeutic neck dissection in node-negative oral cancer. N Engl J Med 2015;373:521-529.
Gou L, Yang W, Qiao X, et al. Marginal or segmental mandibulectomy: treatment modality selection for oral cancer: a systematic review and meta-analysis. Int J Oral Maxillofac Surg. 2018;47(1):1-10.
Haughey BH, Sinha P. Prognostic factors and survival unique to surgically treated p16+ oropharyngeal cancer. Laryngoscope 2012;122 Suppl 2:S13-S33.
Mendenhall WM, Dziegielewski PT, Pfister DG. Chapter 45- Cancer of the Head and Neck. In: DeVita VT, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 12th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2023.
National Cancer Institute. Physician Data Query (PDQ). Lip and Oral Cavity Cancer Treatment. May 14, 2025. Accessed at https://www.cancer.gov/types/head-and-neck/hp/adult/lip-mouth-treatment-pdq on January 29, 2026.
National Comprehensive Cancer Network. Clinical Practice Guidelines in Oncology (NCCN Guidelines), Head and Neck Cancers, V.1.2026. Accessed at www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdf on February 3, 2026.
National Comprehensive Cancer Network (NCCN). NCCN Clinical Practice Guidelines in Oncology: Smoking Cessation. V.2.2025. Accessed at https://www.nccn.org/professionals/physician_gls/pdf/smoking.pdf on February 3, 2026.
Solomon J, Hinther A, Matthews TW, et al. The impact of close surgical margins on recurrence in oral squamous cell carcinoma. J Otolaryngol Head Neck Surg 2021;50:9.
Last Revised: March 23, 2026
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.


