Your gift is 100% tax deductible.
What Is Thymus Cancer?
Cancer that starts in the thymus gland is called thymus cancer. It starts when cells in the thymus gland grow out of control and crowd out normal cells. Thymus cancers are rare.
The thymus
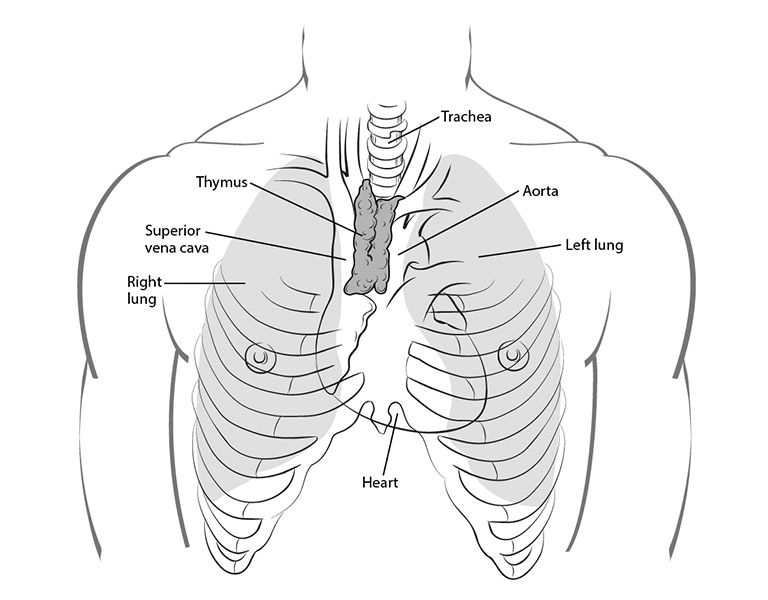
The thymus is a small organ just behind the breast bone (sternum) in the front part of the chest. The thymus is in a part of the chest called the mediastinum, the space between the lungs that also contains the heart, part of the aorta, the esophagus (the tube that connects the mouth to the stomach), part of the trachea (windpipe), and many lymph nodes. The thymus sits just in front of and above the heart.
The thymus has 2 halves, called lobes. It has an irregular shape. There are a lot of small bumps called lobules on its surface. The thymus has 3 main layers:
- The medulla is the inner part of the thymus.
- The cortex is the outer layer that surrounds the medulla.
- The capsule is the thin covering over the outside of the thymus.
The thymus reaches its biggest size during puberty. Then it shrinks during adulthood, and most of it is replaced by fat tissue.
The thymus is an important part of the body’s immune system. Starting very early in life, the thymus makes immune cells called T lymphocytes (also known as T cells) and helps them to mature. T lymphocytes then travel to lymph nodes (small, bean-shaped organs that filter lymph fluid) throughout the body, where they help fight infections.
The thymus is made of different types of cells. Each kind can develop into a different type of cancer:
- Epithelial cells give the thymus its structure and shape. Thymomas and thymic carcinomas develop from these cells.
- Lymphocytes make up most of the rest of the thymus. Whether in the thymus or in other parts of the body, these immune system cells can develop into cancers called Hodgkin lymphoma and non-Hodgkin lymphoma.
- Kulchitsky cells, or neuroendocrine cells, are much less common cells that normally release certain hormones. These cells can give rise to thymic neuroendocrine tumors (TNETs), which are described below.
Thymomas and thymic carcinomas
Thymomas and thymic carcinomas are tumors that start from thymic epithelial cells. They are known as thymic epithelial tumors (TETs). Doctors have faced challenges in trying to figure out the best way to describe and classify these rare tumors.
In the past, thymomas were sometimes divided into benign (non-cancer) thymomas and malignant (cancer) thymomas, while thymic carcinomas were thymic tumors that had already spread to other parts of the body when they were found.
Now, most doctors think all thymomas can become cancer over time, and the best way to predict how they will behave is based on if they have grown into tissues beyond the thymus (and if so, how far). The system used to describe the stage (extent) of thymomas is covered in How Is Thymus Cancer Staged?
WHO classification system for thymomas
Thymomas are classified by how they look under a microscope and by tests done on the tissue samples. This is called the histologic type. The system used for this classification, which is from the World Health Organization (WHO), assigns letters to the different types of thymomas.
Type A: The cells in these tumors are spindle-shaped or oval epithelial cells that are fairly normal looking. This is the rarest type of thymoma, but it seems to have the best outlook.
Type AB: This type, also known as a mixed thymoma, looks mostly like type A, but there are also areas of lymphocytes mixed in the tumor.
Type B1: This type looks a lot like the normal structure of the thymus. It has a lot of lymphocytes along with normal-looking thymus cells.
Type B2: This type also has a lot of lymphocytes, but the thymus epithelial cells are larger with abnormal nuclei (the DNA-containing part of the cell).
Type B3: This type has few lymphocytes and is mostly made of thymus epithelial cells that look close to normal.
Types AB and B2 are the most common types of thymoma. Type A is the least common.
Type A tends to have the best outlook, and the outlook for type B3 tends to be worse than the others. Still, for most types of thymoma, the stage (extent of growth and spread) is a better predictor of a person’s outcome than the histologic type.
Thymic carcinoma cells look very abnormal under a microscope. The cells may no longer even look like thymus cells. Instead, the cells look like cancers that start in other parts of the body. These tumors have often grown into nearby tissues and/or spread (metastasized) to other parts of the body by the time they are found. The outlook for thymic carcinomas tends to be worse than for thymomas.
Thymic neuroendocrine tumors (TNETs)
Thymic neuroendocrine tumors (TNETs) are rare tumors that can form from neuroendocrine cells in the thymus. TNETs may be linked with other conditions that affect the endocrine system, like Cushing syndrome and MEN1 syndrome.
These tumors are rare, so not a lot is known about them. But they are usually treated like similar NETs that start in other parts of the body.
There are several types of TNETs:
- Typical carcinoid tumors (TCs): These are low-grade (slow-growing) tumors that rarely spread.
- Atypical carcinoid tumors (ACs): These tumors tend to grow a little faster than typical carcinoids and are somewhat more likely to spread to other organs.
- Large cell neuroendocrine carcinoma (LCNEC). This is a high-grade cancer that tends to grow quickly and is likely to spread to other parts of the body.
- Small cell carcinoma. This is a high-grade cancer, with cells that look like small cell cancers in other parts of the body (such as small cell lung cancer). These cancers tend to grow quickly and to spread to other parts of the body.
For more on how these tumors are typically treated, see Treating Lung Carcinoid Tumors and Treating Small Cell Lung Cancer.
Other cancers and tumors in the mediastinum
Other types of cancers and tumors can also occur in the mediastinum.
Cancers can start in the esophagus (esophageal cancer), in the heart (and the tissue surrounding it), in the trachea (windpipe), and in the lymph nodes (lymphoma).
Rarely, cancers and tumors known as germ cell tumors can start in the mediastinum. These come from cells like those found in the testicles and ovaries.
Sometimes the thyroid gland, which is normally in the neck, is misplaced into the mediastinum. If this happens, a thyroid tumor or cancer can develop in the mediastinum.
More often, cancer that starts in another part of the body, especially the lungs, spreads to the mediastinum.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Kaidar-Person O, Zagar T, Haithcock BE, Weiss J. Chapter 70: Diseases of the Pleura and Mediastinum. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa. Elsevier: 2019.
Meneshian A, Oliver KR, Molina JR. Clinical presentation and management of thymoma and thymic carcinoma. UpToDate. 2024. Accessed at https://www.uptodate.com/contents/clinical-presentation-and-management-of-thymoma-and-thymic-carcinoma on October 18, 2024.
National Cancer Institute. Thymoma and Thymic Carcinoma Treatment (PDQ®)–Health Professional Version. 2024. Accessed at https://www.cancer.gov/types/thymoma/hp/thymoma-treatment-pdq on October 18, 2024.
National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines): Thymomas and Thymic Carcinomas. Version 1.2024. Accessed at https://www.nccn.org on October 18, 2024.
Strosberg JR, Berry MF, Tazelaar HD, Roden AC. Thymic neuroendocrine neoplasms. UpToDate. 2024. Accessed at https://www.uptodate.com/contents/thymic-neuroendocrine-neoplasms on October 18, 2024.
Tazelaar HD, Roden AC. Pathology of mediastinal tumors. UpToDate. 2024. Accessed at https://www.uptodate.com/contents/pathology-of-mediastinal-tumors on October 18, 2024.
Last Revised: January 15, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



