Your gift is 100% tax deductible.
Genes and Cancer
Genes are instructions in our DNA that control how cells grow, divide, and function. Learn about how changes can disrupt normal cell behavior and increase the risk of cancer.
What are genes?
Genes are small parts of DNA that tell a cell how to make the products it needs to work. Most genes contain the code (instructions) to make a certain protein, and each protein has its own job. For example, some proteins help cells grow and make new cells. Others help control how fast cells grow.
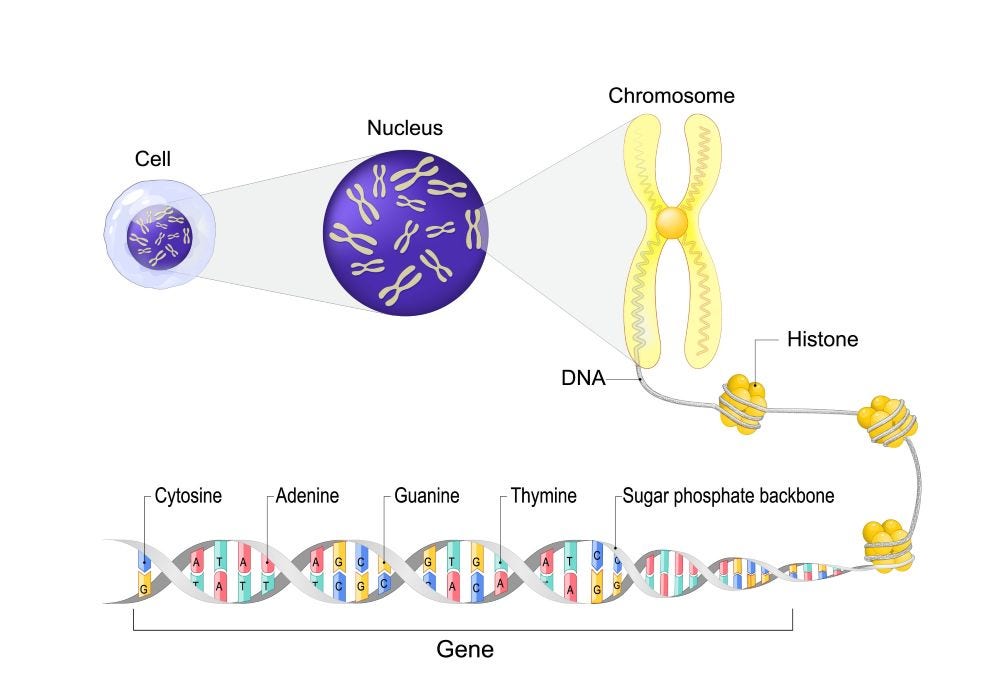
Genes are grouped together on chromosomes, which are long strands of DNA found inside the nucleus (control center) of each cell. Each chromosome carries many genes.
Most human cells have 23 pairs of chromosomes. In each pair, you get one chromosome from your mother and one from your father. This is why children often look like their parents and why some diseases can run in families.
Gene expression
All the cells in the body have the same genes, but each cell only uses the genes it needs. It turns on (activates) the right genes at the right time and turns off (deactivates) the ones it doesn't need. This is called gene expression.
Turning genes on and off helps cells become specialized. For example, it’s how a cell becomes a muscle cell or bone cell.
Some genes stay on all the time because they are needed for basic cell functions. Other genes turn off and on as needed.
Differences in genes
While we all have basically the same set of genes, we also have differences in our genes that make each of us unique.
The ‘code’ or ‘blueprint’ for each gene is contained in chemicals called nucleotides.
DNA is made up of 4 building blocks called nucleotides: adenine (A), thymine (T), guanine (G), and cytosine (C). Each gene is made up of a long chain of nucleotides, the order of which tells the cell how to make a specific protein, just like letters of the alphabet can be grouped to make different words.
Gene changes
Sometimes, there are changes in a gene. These are called gene changes or mutations. For example, one nucleotide ‘letter’ might be changed, missing, or added compared to most other people’s genes.
Gene changes can affect proteins in different ways:
- Some don’t cause any noticeable change.
- Some cause small changes, like making a protein not work well.
- Others cause bigger changes, such as making a protein not work at all.
If a gene change alters how a protein works, it can affect all the cells that carry that gene change, and sometimes the whole body.
Not all gene changes are harmful. Some simply explain normal differences, such as hair or eye color. But others can cause disease or increase the risk of a disease, such as cancer. These are called pathogenic mutations.
Do all gene changes cause cancer?
Gene changes happen often. Your body usually fixes most gene changes, so they do not affect you.
Having just 1 gene change probably will not cause cancer. Cancer is more likely when gene changes build up over many years. That is why older people have cancer more often than young people do.
How gene changes can affect cancer risk
Some genes help control cell growth, repair DNA mistakes, or trigger cell death when needed. When these genes don’t work the way they are supposed to, cancer risk can increase:
- Oncogenes are overactive versions of genes that normally help cells grow, divide, or stay alive. They can cause cells to grow out of control.
- Tumor suppressor genes normally slow down cell division or trigger cell death. When they are turned off, cells can grow out of control.
- DNA repair genes fix mistakes in a cell’s DNA. If they stop working, DNA errors can build up, which might lead to them growing out of control.
Usually, it takes several gene changes before a cell becomes a cancer cell.
Other gene changes don’t directly cause cancer but can increase risk. For example:
- Some changes might make it harder for the body to break down toxins in tobacco smoke, raising the risk of lung and other smoking-related cancers.
- Some gene changes can affect body weight. Excess body weight is linked to higher risk for certain cancers, so these changes might also indirectly affect cancer risk.
When do gene changes occur?
Gene changes can be:
- Inherited from a parent, meaning a person was born with the gene change
- Acquired, meaning the gene change occurred during a person's life
Inherited gene changes and cancer
An inherited gene change is one passed down from a parent. It is present in the very first cell formed when an egg and sperm join. Since all the cells in the body come from this first cell, the gene change is in every cell in the body. It can also be passed on to future children. This type of gene change is called a germline or hereditary mutation.
Most cancers happen after several gene changes build up over time. Being born with an inherited gene change can make it easier and faster for more changes to happen, which can lead to cancer. This is why cancers linked to inherited gene changes often happen at a younger age.
Even so, inherited gene changes are not the main cause of most cancers. Only about 5% to 10% of cancers are caused by inherited changes.
Learn about some of the more common inherited gene changes that can lead to Family Cancer Syndromes.
Acquired gene changes and cancer
An acquired gene change is not passed down from a parent. It develops at some point during a person's life. It starts in 1 cell and is passed on to new cells that come from that cell. This type of gene change cannot be passed to children because it doesn’t affect sperm or egg cells. It is also called a somatic mutation.
Most cancers are caused by acquired gene changes, not inherited ones.
Acquired gene changes can happen for different reasons. Sometimes they are caused by damage to a cell’s DNA, such as from exposure to radiation or certain chemicals. Other times, they happen by chance. For example, when a cell divides, it must copy all its DNA, and mistakes (gene changes) can occur during this process.
Each time a cell divides is another chance for a mutation to occur. Over time, these changes can build up. This is one reason why the risk of cancer increases with age.
Other ways gene activity can be changed
Some changes inside cells that can lead to cancer don’t involve gene changes. Instead, cells can turn genes on or off in other ways, which can affect how cells grow and divide. These changes are called epigenetic changes because they change gene activity without changing the DNA sequence.
Epigenetic changes control which genes are active or inactive, and targeting these changes is an important area of cancer research and treatment.
There are several types of these epigenetic changes:
A small chemical called a methyl group can attach to DNA and turn a gene off, stopping it from making its protein. Removing the methyl group (demethylation) can turn the gene back on.
DNA is wrapped around proteins called histones to form chromosomes. Histones can be chemically changed by adding or removing a small chemical group called an acetyl group. Adding acetyl groups (acetylation) can turn genes on, while removing them (deacetylation) can turn genes off.
Medicines called histone deacetylase (HDAC) inhibitors can treat some cancers by turning on genes that help control cell growth and division.
To make proteins, cells copy a gene into messenger RNA (mRNA), which carries the instructions to the protein-making machinery. Cells can also make other RNA molecules that stick to the mRNA and either destroy it or stop it from working. This keeps the gene from working. Medicines are being developed to target RNAs from specific cancer-causing genes to turn them off.
Related Topics
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
American Society of Clinical Oncology (ASCO). Genes and cancer. Accessed at www.cancer.net. Content is no longer available.
Mahon S. Cancer genetics/genomics. In: Malone-Newton S, Hickey M, Brant JM (eds.). Mosby’s Oncology Nursing Advisor: A Comprehensive Guide to Clinical Practice. 3rd ed. Elsevier; 2024: 35-51.
National Cancer Institute (NCI). Cancer genetics overview (PDQ) – health professional version. Updated May 9, 2025. Accessed at https://www.cancer.gov/about-cancer/causes-prevention/genetics/overview-pdq on March 19, 2026.
National Cancer Institute (NCI). The genetics of cancer. Updated August 8, 2024. Accessed at https://www.cancer.gov/about-cancer/causes-prevention/genetics on March 19, 2026.
National Library of Medicine. Gene mutation. MedlinePlus Genetics. Accessed at https://medlineplus.gov/genetics/understanding/mutationsanddisorders/genemutation/ on March 19, 2026.
Last Revised: May 12, 2026
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



