2023 Cancer Facts & Figures

Cancer Facts & Figures 2023 is an educational companion for Cancer Statistics 2023, a scientific paper published in the American Cancer Society journal, CA: A Cancer Journal for Clinicians. These annual reports provide:
- Estimated numbers of new cancer cases and deaths in 2023 by cancer site and US state
- Current cancer incidence, mortality, and survival statistics
- Information on cancer symptoms, risk factors, early detection, and treatment
Also see this news story: Incidence Rate Drops for Cervical Cancer But Rises for Prostate Cancer
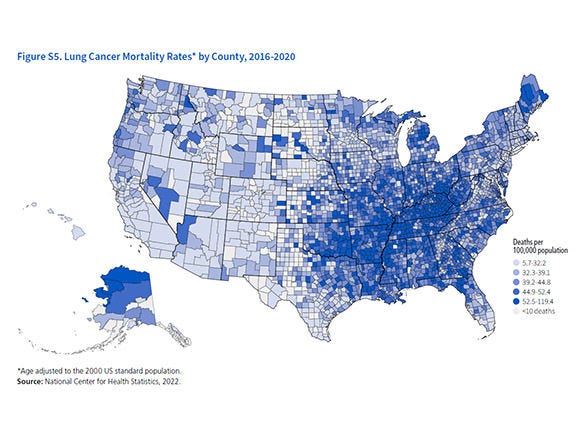
This special section provides an overview of lung cancer occurrence in the United States, including information about risk factors, prevention, and early detection, as well as what the American Cancer Society is doing to reduce the burden.
Most requested Tables & Figures
Trends in Age-adjusted Cancer Death Rates by Site, US, 1930-2020
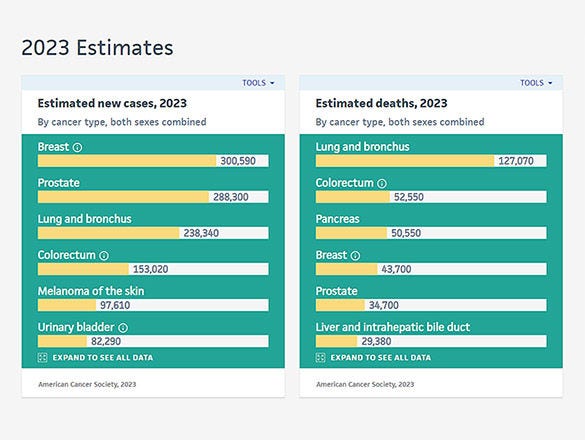
Estimated Number of New Cancer Cases and Deaths, US, 2023
- By Sex (PDF)
Estimated Number for Selected Cancers by State, US, 2023 (PDF)
Leading Sites of New Cancer Cases and Deaths - 2023 Estimates (PDF)
Probability of Developing Invasive Cancer During Selected Age Intervals by Sex, US, 2017-2019 (PDF)
Incidence and Mortality Rates for Selected Cancers by Race and Ethnicity, US, 2015-2020 (PDF)
2023 Supplemental Data
Estimated Number for the 4 Major Cancers by Sex & Age Group, 2023
Estimated Number of New Cases & Deaths by State for 21 Cancer Sites, 2023 (PDF)
Lifetime Probability of Developing & Dying from Cancer for 23 Sites, 2017-2019 (PDF)
Glossary for Nonscientists
Featured Term:
Cancer incidence
(also called cancer occurrence)
The number of new diagnoses of cancer, or new cases, in a group. Incidence counts can give information about a specific group but can’t be used to compare groups because the numbers alone don’t account for the size of the group or age ranges of the people in it. Comparing groups requires cancer incidence rates.
Citations, Credits, & Permissions
Suggested citation: Cancer Facts & Figures 2023. Atlanta: American Cancer Society, Inc. 2022.
Please note that any reproduction or re-use of this publication or portions of it should credit the appropriate edition of the American Cancer Society Annual Cancer Facts & Figures publication. See the PDF contents page for more copyright info and permissions for use.