Your gift is 100% tax deductible.
Your Breast Pathology Report: Ductal Carcinoma In Situ (DCIS)
Learn about some of the medical terms in a pathology report that shows ductal carcinoma in situ (DCIS).
Types of breast biopsies
A biopsy is a procedure that removes small pieces of tissue so they can be examined under a microscope or tested. A breast biopsy can be done by:
- Needle biopsy, where a hollow needle is used to remove samples from an abnormal area in your breast.
- Incisional biopsy, a type of surgical biopsy in which only part of an abnormal area is removed.
- Excisional biopsy, a type of surgical biopsy that removes the entire abnormal area, often with some of the surrounding normal tissue. It is much like a lumpectomy, a type of breast-conserving surgery.
After biopsy samples are collected from your breast, they are studied by a pathologist, a doctor who specializes in diagnosing and classifying disease. After testing the samples, the pathologist creates a pathology report on what was found. Your doctors can use this report to help manage your care.
What is in-situ carcinoma of the breast?
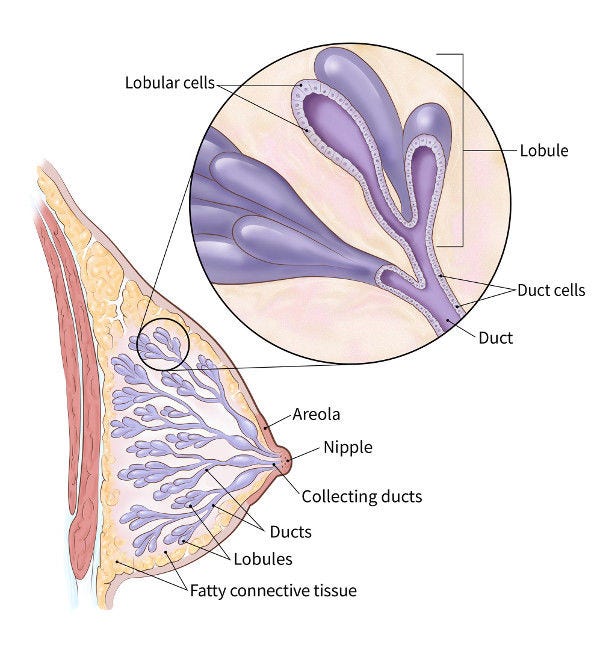
The normal breast contains milk ducts (tiny tubes) that end in groups of sacs called lobules (where milk is made). Ducts, lobules, and many other organs in the body are lined by a layer of tissue called epithelium.
A carcinoma is a cancer that begins in the epithelium. Nearly all breast cancers are carcinomas.
In-situ carcinoma, also known as carcinoma in situ or CIS, means that abnormal cells are growing in the epithelium but they aren’t invading into deeper tissue layers.
If the carcinoma cells have grown (invaded) deeper than the lining layer of the ducts or lobules, it is called invasive or infiltrating carcinoma. This is a true breast cancer, in which the tumor cells can spread (metastasize) to other parts of the body.
Types of CIS
The 2 main types of CIS of the breast are:
- Ductal carcinoma in situ (DCIS)
- Lobular carcinoma in situ (LCIS)
DCIS and LCIS are diagnosed based on how the cells and tissue look under the microscope, sometimes along with other lab tests. Sometimes both are found in the same biopsy.
In-situ carcinoma with duct and lobular features means that under the microscope, the CIS looks like DCIS in some ways and LCIS in some ways.
Ductal carcinoma in situ (DCIS)
DCIS is often described as a precancer, because if it’s left untreated, it can sometimes become an invasive cancer.
While it’s not clear that all DCIS would become invasive cancer, doctors can’t tell which ones would be safe to leave untreated. Therefore, DCIS is usually treated with surgery. In some cases, radiation or hormone therapy, like tamoxifen, is given after surgery to lower the chance that it will come back (recur) or become cancer.
For more information about DCIS, see:
Terms that might describe DCIS
These terms are used to describe certain ways that the DCIS might look under the microscope:
- Cribriform
- Micropapillary
- Comedo (or “with comedo necrosis”)
- Papillary
- Solid
Some of these are linked to a higher chance of the DCIS coming back after treatment, so finding them might change your treatment. Your doctor will discuss these findings with you.
DCIS grades
Under a microscope, certain cell features can help predict how quickly DCIS is likely to grow and how likely it is to come back after surgery. This is known as the DCIS grade.
There are different ways to describe the 3 grades of DCIS.
Low-grade DCIS or nuclear grade 1: The cells have a low mitotic rate, meaning few of them are dividing, and their nuclei (where the DNA is stored) look more like those of normal breast cells. Low grade DCIS tends to grow slowly and is less likely to come back after surgery.
Intermediate-grade DCIS or nuclear grade 2: The cells have an intermediate mitotic rate, meaning the DCIS is more likely to grow quickly and to come back after surgery.
High-grade DCIS or nuclear grade 3: The cells have a high mitotic rate, and their nuclei look more abnormal. High grade DCIS tends to grow the fastest and is most likely to come back after surgery. It is also more likely to turn into invasive breast cancer.
Higher grade DCIS might require additional treatment.
DCIS size
If the entire tumor or area of DCIS is removed with an excisional biopsy or breast-conserving surgery, the pathologist will measure it. This might be done by:
- Looking at it under a microscope.
- Gross examination (looking at it with the naked eye).
- Noting the number of microscopic slides that contain DCIS. For example, the report might say that DCIS was found on 3 slides.
The larger the area of DCIS, the more likely it is to come back after surgery. Doctors use information about the size of the DCIS when deciding whether to recommend further treatments.
Measurements of the area of DCIS are not often reported after a needle biopsy because this type of biopsy only samples a part of the tumor.
Paget disease
Paget disease, also called Paget’s disease, Paget disease of the nipple, or Paget disease of the breast, is a condition in which cells resembling those of DCIS are found in the skin of the nipple and the nearby skin (the areola).
If Paget disease is found, most often it means that there is DCIS or invasive carcinoma (cancer) in the underlying breast tissue.
When Paget disease is found on a needle or punch biopsy, the doctor will usually want to remove the area of Paget disease completely and to look for DCIS or cancer nearby. Further treatment depends on if DCIS or cancer is found. Talk to your doctor about the best treatment for you.
Estrogen receptor (ER) and progesterone receptor (PR) status
If DCIS is found on the biopsy, the cells will most likely be tested for hormone receptors.
Receptors are proteins on cells that can attach to certain substances, such as hormones in the blood. Normal breast cells and some breast cancer cells have receptors that attach to the hormones estrogen and progesterone. These hormones often fuel the growth of the cancer cells.

On your pathology report
Testing for ER is done for most cases of DCIS, although testing for PR might not be needed.
- ER-positive or ER+ means it has estrogen receptors (ER).
- PR-positive or PR+ means it has progesterone receptors (PR).
Results for ER and PR are reported separately, and they might be reported in different ways:
- Negative, weakly positive, or positive
- Percent positive
- Percent positive and whether the staining is weak, moderate, or strong
Knowing the hormone receptor status of your DCIS can help predict whether hormone therapy, such as tamoxifen, can help lower the risk of it coming back after treatment.
Ask your doctor how these results might affect your treatment.
Other terms that might be on a pathology report
In addition to DCIS, you might see other medical terms on your pathology report. Many of these are benign changes. Usually, they are not important when seen on a biopsy where there is DCIS.
ADH and ALH are types of atypical (abnormal) changes in breast cells that can sometimes be seen on a breast biopsy. They aren’t as serious as DCIS. If ADH or ALH is mentioned on your pathology report, talk with your doctor about what these findings might mean for your care.
Other benign changes that might be noted on a pathology report include:
- Usual ductal hyperplasia (UDH)
- Adenosis or sclerosing adenosis
- Radial scar or complex sclerosing lesion
- Papilloma or papillomatosis
- Apocrine metaplasia
- Columnar cell change
- Collagenous spherulosis
- Duct ectasia
- Fibrocystic changes or cysts
- Flat epithelial atypia (FEA)
- Columnar alteration with prominent apical snouts and secretions (CAPSS)
These aren’t likely to be important if they’re seen on a biopsy sample that also contains DCIS.
Microcalcifications or calcifications are small calcium deposits that can be found in both noncancerous and cancerous breast lesions. They can be seen both on mammograms and under a microscope.
Because certain calcifications can be found in areas containing cancer, their presence on a mammogram might lead to a biopsy of the area. Once the biopsy is done, the pathologist looks at the tissue removed to be sure that it contains calcifications. If the calcifications are there, the doctor knows that the biopsy sampled the correct area (the abnormal area on the mammogram).
When the entire area of DCIS and some surrounding normal breast tissue is removed, the margins (edges) of the specimen are coated with ink. This helps the pathologist tell whether the abnormal area was removed completely when looking at it under a microscope. If DCIS is touching the ink, called positive margins, it can mean that some DCIS cells were left behind and more surgery or other treatments might be needed. Sometimes, though, the surgeon has already removed more tissue during surgery to help make sure that this isn’t needed.
If your pathology report shows DCIS with positive margins, your doctor will talk to you about what treatment is best.
E-cadherin is a test that might be done to help determine if carcinoma in situ is ductal (DCIS) or lobular (LCIS). The cells in DCIS are usually positive for E-cadherin. If your report doesn’t mention E-cadherin, it means that this test wasn’t needed.
Other tests that might be done to help diagnose DCIS include:
- High molecular weight cytokeratin (HMWCK)
- CK903, also known as 34betaE12
- CK5/6
- p63
- Muscle specific actin
- Smooth muscle myosin heavy chain
- Calponin
- Keratin
Not all biopsy samples need these tests. If these tests appear on your pathology report, ask your health care provider what the results mean for you.
Gene expression profiling or genomic tests
Gene expression profiling, also called genomic testing, can look at the activity of many different genes at once to learn more about a person’s DCIS and which treatment options might be best.
For example, a test known as Oncotype DX can be done on DCIS cells to help predict how likely it is to come back (recur), and therefore if further treatment might be needed. But not everyone with DCIS needs this type of test.
If your doctor orders this test, ask your doctor to explain what the results mean. The results don’t affect your diagnosis, although they might affect your treatment options.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Bleiweiss IJ. Pathology of breast cancer. UpToDate. 2026. Accessed at https://www.uptodate.com/contents/pathology-of-breast-cancer on March 18, 2026.
Collins LC, Laronga C, Wong JS. Breast ductal carcinoma in situ: Epidemiology, clinical manifestations, and diagnosis. UpToDate. Accessed at https://www.uptodate.com/contents/breast-ductal-carcinoma-in-situ-epidemiology-clinical-manifestations-and-diagnosis on March 19, 2026.
Collins LC, Laronga C, Wong JS. Ductal carcinoma in situ: Treatment and prognosis. UpToDate. Accessed at https://www.uptodate.com/contents/ductal-carcinoma-in-situ-treatment-and-prognosis on March 19, 2026.
National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology: Breast Cancer Risk Reduction. Version 1.2026. Accessed at https://www.nccn.org on March 19, 2026.
Sabel MS. Overview of benign breast diseases. UpToDate. 2026. Accessed at https://www.uptodate.com/contents/overview-of-benign-breast-diseases on March 18, 2026.
Last Revised: May 21, 2026
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



