Your gift is 100% tax deductible.
Surgery for Laryngeal and Hypopharyngeal Cancers
- Quit smoking before laryngeal and hypopharyngeal cancer surgery
- What kind of surgery is done to treat laryngeal or hypopharyngeal cancer?
- Endoscopic surgery
- Laryngectomy
- Total or partial pharyngectomy
- Lymph node removal
- Thyroidectomy
- Reconstructive surgery
- Tracheostomy
- Gastrostomy tube
- Possible risks and side effects of surgery
- More information about surgery
Studies have shown that people with head and neck cancer who are treated at centers that perform a lot of head and neck cancer surgeries, tend to live longer. And because of the complicated type of surgeries, along with the need for coordination between cancer specialists to make a complete treatment plan, it’s very important to have a surgeon and cancer center who has experience treating these cancers.
Quit smoking before laryngeal and hypopharyngeal cancer surgery
If you smoke, you should quit. Smoking during cancer treatment is linked to poor wound healing, more side effects, and less benefit from treatment which can raise your risk of the cancer coming back (recurrence).Smoking after treatment can also increase the chance of getting another new cancer. Quitting smoking for good (before treatment starts, if possible) is the best way to improve your chances of survival. It is never too late to quit. For help, see How To Quit Using Tobacco.
What kind of surgery is done to treat laryngeal or hypopharyngeal cancer?
Surgery is commonly used to treat laryngeal and hypopharyngeal cancers. Depending on the type, stage, location of the cancer, and other tissues involved, different operations might be used to remove the cancer and sometimes other tissues near the larynx or hypopharynx. In almost all surgeries, the plan is to take out all of the cancer along with a rim (margin) of healthy tissue around it.
Surgery might be the only treatment needed for some early-stage cancers. It also might be used along with other treatments, like chemotherapy or radiation, for later stage cancers.
After the cancer is removed, reconstructive surgery might be done to help make the changed areas look and work better.
Endoscopic surgery
For this surgery, an endoscope is passed down your throat to find the tumor. The endoscope is a long thin tube with a light and camera on the end of it. Using the camera, the doctor can see the tumor and pass long surgical instruments through the endoscope to find, biopsy, and treat some early-stage cancers of the larynx. For early-stage laryngeal cancer, studies have shown that endoscopic surgery can be as effective as radiation therapy.
Vocal cord stripping
If the cancer or pre-cancer is confined to the surface of the vocal cords, this type of surgery can strip away the cancer and the superficial layers of tissue on the vocal cords. Most people can speak normally again after this operation.
Laser surgery
Lasers can also be used through the endoscope. They can be used to excise (cut out) the tumor. This is sometimes called transoral laser microsurgery (TLM).
Laryngectomy
Laryngectomy is the removal of part or all of the larynx (voice box). It involves making an incision (cut) on the outside of the neck over the area of the Adam’s apple.
Partial laryngectomy: Smaller cancers of the larynx often can be treated by removing only part of the voice box. There are different types of partial laryngectomies, but they all have the same goal: to take out all of the cancer while leaving behind as much of the larynx as possible.
In a supraglottic laryngectomy, only the part of your larynx above the vocal cords is removed. This procedure can be used to treat some supraglottic cancers, and will allow you to speak normally afterward.
For small cancers of the vocal cords, the surgeon might be able to remove the cancer by taking out only one side of the larynx (one vocal cord) and leaving the other behind. This is called a hemilaryngectomy. Some ability to speak remains after this surgery.
Total laryngectomy: This procedure removes your entire larynx. The trachea (windpipe) is then brought up through the skin of the front of your neck as a stoma (or hole) that you breathe through (see the picture below). This is called a tracheostomy. If your entire larynx is removed, you will no longer be able to speak as you did, but you can learn other ways of speaking. (See Living as a Laryngeal or Hypopharyngeal Cancer Survivor) The connection between the throat and the esophagus (swallowing tube) is usually not affected, so you can swallow food and liquids just as you did before the operation.
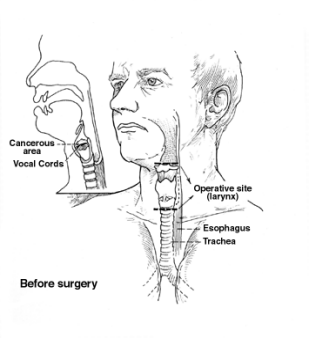
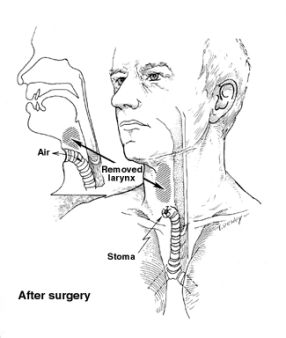
Total or partial pharyngectomy
Surgery to remove all or part of the pharynx (throat) is called a pharyngectomy. This operation might be used to treat cancers of the hypopharynx. Often, the larynx is removed along with the hypopharynx. After surgery, you may need reconstructive surgery to rebuild this part of the throat and improve your ability to swallow.
Lymph node removal
Cancers of the larynx and hypopharynx can spread to the lymph nodes in the neck. If your doctor thinks that lymph node spread is likely, lymph nodes (and other nearby tissues) may be removed from your neck. This operation, called a neck dissection, is often done at the same time as the surgery to remove the main tumor. This might be needed to be sure that all of the lymph nodes likely to contain cancer are removed. Doctors determine the likelihood the cancer has spread to the lymph nodes based on the size and location of the tumor and whether or not the lymph nodes look enlarged or abnormal on an imaging test.
The two most common forms of neck dissection are the comprehensive neck dissection and the less extensive selective neck dissection. They differ in the amount of tissue removed from the neck.
- Comprehensive neck dissection: Some nerves, veins, and muscles might be removed, while still removing all of the lymph nodes in the neck.
- Selective neck dissection: No nerves, veins, or muscles are affected during this type of neck dissection and only lymph nodes in selected parts of the neck are removed. This type of surgery removes fewer normal structures to try to keep your shoulder and neck working normally.
Thyroidectomy
Sometimes the cancer spreads into the thyroid gland and all or part of it must be removed. The thyroid sits in the front of your neck and wraps around to the sides of the trachea (windpipe). It makes hormones that control your metabolism and how your body uses calcium.
If all of the thyroid gland is removed, your body can no longer make the thyroid hormone it needs. In this case, you must take thyroid hormone (levothyroxine) pills to replace the loss of the natural hormone.
Reconstructive surgery
These operations might be done to help restore the structure or function in areas affected by surgery to remove the cancer.
Myocutaneous flaps: Sometimes a muscle and attached piece of skin, from an area close to your throat, such as the chest (pectoralis major flap), may be partly removed and turned upward to reconstruct or rebuild part of your throat.
Free flaps: With the advances in microvascular surgery (sewing together small blood vessels under a microscope), surgeons now have many more reconstruction options. Tissues from other parts of your body such as a piece of intestine or a piece of arm muscle can be used to replace parts of your throat.
Tracheostomy
A tracheostomy is made when the trachea (windpipe) is connected to a hole (stoma) in the front of the neck to help a person breathe by letting air in and out of the lungs through that hole. It may be used in certain cases.
For instance, after a partial laryngectomy or pharyngectomy, a temporary (short-term) tracheostomy may be needed to help protect your airway while you recover from surgery. To do this, a small plastic tube (a trach tube ;short for tracheostomy tube) is put into your trachea through a hole in the front of your neck. The tube stays in place for a short time, and is removed when it's no longer needed. You then breathe through your mouth and nose like you did before.
As described above, a permanent tracheostomy is needed after a total laryngectomy. In this case, the opening in the trachea is attached to a hole in the skin in the front of your neck. A trach tube or stoma cover may be needed to help keep the tracheostomy hole open. You will breathe through this opening instead of through your mouth and nose.
If a laryngeal or hypopharyngeal cancer is blocking the windpipe and is too big to remove completely, an opening may be made to connect the lower part of your windpipe to a stoma (hole) in the front of your neck to bypass the tumor and allow you to breathe more comfortably.
Gastrostomy tube
Cancers in the larynx and hypopharynx might make it hard for you to swallow enough food to maintain good nutrition and a healthy weight. This can make you weak and make it harder to finish treatment.
Some people with laryngeal or hypopharyngeal cancer may need to have a feeding tube (usually called a gastrostomy tube or G-tube), put in place before treatment. A G-tube is put through the skin and muscle of your abdomen (belly) right into your stomach. The tube is often put in place with the help of a flexible, lighted instrument (endoscope) passed down your mouth and into the stomach. This is done while you are sedated (asleep). When it's placed through an upper endoscopy, it's called a percutaneous endoscopic gastrostomy, or PEG tube. Another option is to put the tube in during an operation. Once in place, liquid nutrition and medicines can be put right into the stomach through the tube.
Often, the gastrostomy tube is only needed for a short time to help you get enough nutrition during cancer treatment. The tube is often removed once you can swallow again after treatment. It's important to keep swallowing even when you're getting most of your nutrition through a G tube. This helps keep those muscles active and gives you a better chance of going back to swallowing normally after treatment is complete.
Possible risks and side effects of surgery
All surgery carries some risks, including blood clots, infections, complications from anesthesia, and pneumonia. These risks are generally low but are higher with more complicated operations. Rarely, some people do not survive the surgery.
Patients who have a laryngectomy or pharyngectomy typically lose the ability to speak normally. Some people will need a tracheostomy after surgery. Less extensive operations can also affect speech in some cases. (See Living as a Laryngeal or Hypopharyngeal Cancer Survivor for more about speech after surgery.)
Surgeries that involve the throat or voice box can lead to a gradual narrowing (stenosis) of the throat or larynx. Sometimes this can make it hard to breathe. If this happens, you might need a tracheostomy.
Throat or larynx surgeries might also sometimes make it hard to swallow well. This can affect how you eat, and might be severe enough to require a permanent feeding tube.
Laryngectomy and pharyngectomy can also lead to the development of a fistula (an abnormal opening between 2 areas that are not normally connected). Surgery may be needed to fix it.
A very rare but serious complication of neck surgery is rupture of a carotid artery (the large artery on either side of the neck).
More information about surgery
For more general information about surgery as a treatment for cancer, see Cancer Surgery.
To learn about some of the side effects listed here and how to manage them, see Managing Cancer-related Side Effects.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
Britt CJ, Gourin CG. Contemporary Management of Advanced Laryngeal Cancer. Laryngoscope Investig Otolaryngol. 2017;2(5):307-309.
Leeman JE, Katabi N, Wong, RJ, Lee NY, Romesser PB. Chapter 65 - Cancer of the Head and Neck. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa: Elsevier; 2020.
Lorenzo JG, Martinez VM, Quera AR, et al. Modifications in the treatment of advanced laryngeal cancer throughout the last 30 years. Eur Arch Otorhinolaryngol. 2017;274:3449–3455.
Mendenhall WM, Dziegielewski PT, Pfister DG. Chapter 45- Cancer of the Head and Neck. In: DeVita VT, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 11th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2019.
National Cancer Institute. Physician Data Query (PDQ). Hypopharyngeal Cancer Treatment. October 04, 2019. Accessed at https://www.cancer.gov/types/head-and-neck/patient/adult/hypopharyngeal-treatment-pdq on May 15, 2020.
National Cancer Institute. Physician Data Query (PDQ). Laryngeal Cancer Treatment. November 21, 2019. Accessed at https://www.cancer.gov/types/head-and-neck/patient/adult/laryngeal-treatment-pdq on May 16, 2020.
National Comprehensive Cancer Network (NCCN). NCCN Clinical Practice Guidelines in Oncology: Head and Neck Cancers. V.1.2020. Accessed at www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdf on May 15, 2020.
Salvador-Coloma C, Cohen E. Multidisciplinary Care of Laryngeal Cancer. J Oncol Pract. 2016;12(8):717-724.
Shenoy AM, Prashanth V, Shivakumar T, et al. The utility of second look microlaryngoscopy after trans oral laser resection of laryngeal cancer. Indian J Otolaryngol Head Neck Surg. 2012;64(2):137‐141. doi:10.1007/s12070-012-0496-7.
Steuer CE, El-Deiry M, Parks JR, Higgins KA, Saba NF. An update on larynx cancer. CA Cancer J Clin. 2017;67(1):31-50.
Last Revised: January 21, 2021
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



