Your gift is 100% tax deductible.
Surgery for Cervical Cancer
Many women with cervical cancer will have some type of surgery. Surgery can be used to:
- Help diagnose cervical cancer
- Help determine how far the cancer has spread
- Help treat the cancer (especially for early-stage cancers)
Surgery for cervical precancers
These procedures are used to treat precancers of the cervix:
- Ablation destroys cervical tissue with cold temperatures (cryosurgery) or with a laser (laser ablation) rather than removing it.
- Excisional surgery (conization) cuts out and removes the precancer.
Cryosurgery is a type of ablation where a very cold metal probe is placed directly on the cervix. This kills the abnormal cells by freezing them. It is used to treat cervical intraepithelial neoplasia (CIN). This can be done in a doctor’s office or clinic. After cryosurgery, you may have a watery brown discharge for a few weeks.
Laser ablation directs a focused laser beam through the vagina to vaporize (burn off) abnormal cells. This might be done in a doctor’s office under local anesthesia (numbing medicine) or in the operating room with general anesthesia, since it can cause more discomfort than cryotherapy. It is also used to treat cervical intraepithelial neoplasia (CIN).
Another way to treat cervical intraepithelial neoplasia (CIN) is with excisional surgery called conization. The doctor removes a cone-shaped piece of tissue from the cervix. The tissue removed in the cone includes the transformation zone where cervical precancers and cancers are most likely to start. A cone biopsy is not only used to diagnose precancers and cancers. It can also be used as a treatment since it can sometimes completely remove precancers and some very early cancers.
The procedure can be done in different ways:
- Using a surgical blade (cold knife cone biopsy)
- Using a laser beam (laser conization)
- Using a thin wire heated by electricity (the loop electrosurgical excision procedure, LEEP or LEETZ procedure).
Surgery for invasive cervical cancer
Procedures to treat invasive cervical cancer are:
- Hysterectomy (simple or radical)
- Trachelectomy
- Pelvic exenteration
A simple hysterectomy removes the uterus (both the body of the uterus and the cervix) but not the structures next to the uterus (parametria and uterosacral ligaments). The vagina and pelvic lymph nodes are not removed. The ovaries are usually left in place unless there is another reason to remove them.
Simple hysterectomy can be used to treat certain types of severe CIN or certain types of very early cervical cancer.
There are different ways to do a hysterectomy:
- Abdominal hysterectomy: The uterus is removed through a surgical incision in the front of the abdomen.
- Vaginal hysterectomy: The uterus is removed through the vagina.
- Laparoscopic hysterectomy: The uterus is removed using laparoscopy. First, a thin tube with a tiny video camera at the end (the laparoscope) is inserted into one or more very small surgical incisions made on the abdominal wall to see inside the abdomen and pelvis. Small instruments can be controlled through the tube(s), so the surgeon can cut around the uterus without making a large cut in the abdomen. The uterus is then removed through a cut in the vagina.
- Robotic-assisted surgery: In this approach, the laparoscopy is done with special tools attached to robotic arms that are controlled by the doctor to help perform precise surgery.
Patients get general anesthesia for these operations.
For a laparoscopic or vaginal hysterectomy, the hospital stay is usually 1 to 2 days, followed by a 2- to 3-week recovery period. A hospital stay of 3 to 5 days is common for an abdominal hysterectomy, and complete recovery takes about 4 to 6 weeks.
Possible side effects: Any type of hysterectomy results in infertility (inability to have children). Complications could include bleeding, infection, or damage to the urinary or intestinal systems, such as the bladder or colon.
Hysterectomy does not change the ability to feel sexual pleasure. The uterus and cervix are not needed for someone to reach an orgasm. The area around the clitoris and the lining of the vagina remain as sensitive as before a hysterectomy. More information about managing the sexual side effects of cervical cancer treatment can be found in How Cancer Surgery Can Affect Sex for Women.
For this operation, the surgeon removes the uterus along with the tissues next to the uterus (the parametria and the uterosacral ligaments), the cervix, and the upper part (about 1 inch [2to 3 cm]) of the vagina next to the cervix. The ovaries are not removed unless there is some other medical reason to do so. More tissue is removed in a radical hysterectomy than in a simple hysterectomy, so the hospital stay may be longer. Often, some pelvic lymph nodes are removed as well. (This procedure, known as lymph node dissection, is covered below on this page.)
This surgery is usually done through a large abdominal incision (also known as open surgery).
A radical hysterectomy can also be done using laparoscopy or robot-assistance. (See the Simple hysterectomy section for a description of laparoscopy.) These techniques are also referred to as minimally invasive surgery. Laparoscopic (or robotic) surgery can result in less pain, less blood loss during the operation, and a shorter hospital stay compared to open surgery. Studies have shown, however, that patients who have minimally invasive radical hysterectomies for cervical cancer have a higher chance of the cancer recurring and a higher risk of dying from the cancer than those who have surgery through an abdominal incision (open surgery). Having a radical hysterectomy through an abdominal cut is the preferred type of surgery in most cases. Laparoscopic surgery may still be an option for a small specific group of patients with early-stage cancer, but you should discuss your options carefully with your doctor.
A modified radical hysterectomy is similar to a radical hysterectomy but does not remove as much of the vagina and tissues next to the uterus (the parametria and the uterosacral ligaments) and lymph nodes are usually not removed.
Possible side effects: Because the uterus is removed, this surgery results in infertility[BG1] . Because some of the nerves to the bladder are removed, some patients have problems emptying their bladder after this operation and may need a catheter for a time. Complications could include bleeding, infection, or damage to the urinary and intestinal systems such as the bladder or colon.
When some of the lymph nodes are removed to check for cancer, lymphedema (leg swelling) might develop. This is not common but may happen after surgery and is treated with different methods.
Radical hysterectomy does not change the ability to feel sexual pleasure. Although the vagina is shortened, the area around the clitoris and the lining of the vagina is as sensitive as before. A uterus or cervix is not needed to reach orgasm. When cancer has caused pain or bleeding with intercourse, the hysterectomy might actually improve a sex life by stopping these symptoms.
A radical trachelectomy treats you and keeps your ability to have children. The operation is done either through the vagina or the abdomen and is sometimes done using laparoscopy or a robot.
This procedure removes the cervix and the upper part of the vagina but not the body of the uterus. The surgeon then places a permanent "purse-string" stitch inside the uterine cavity to keep the opening of the uterus closed, the way the cervix normally would.
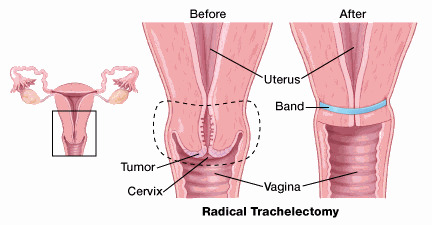
The nearby lymph nodes are also removed using laparoscopy, which may require another incision (cut). The operation is done either through the vagina or the abdomen.
After trachelectomy, some are able to carry a pregnancy to term and deliver a healthy baby by cesarean section, although those who have had this surgery might have a higher risk of miscarriage.
This operation is done for very specific cases of recurrent cervical cancer. All of the same organs and tissues are removed as in a radical hysterectomy with pelvic lymph node dissection. (Lymph node dissection is discussed in the next section.) In addition, the bladder, vagina, rectum, and part of the colon are also removed, depending on where the cancer has spread.
If your bladder is removed, you will need a new way to store and get rid of urine. This usually means using a short piece of intestine to function as a new bladder. The new bladder may be connected to the abdominal wall so that urine is drained periodically when the patient places a catheter into a urostomy (a small opening). Or urine drains continuously into a small plastic bag attached to the front of the abdomen. For more information, see Urostomy Guide.
If the rectum and part of the colon are removed, a new way to get rid of fecal waste must be created. This is done by attaching the remaining intestine to the abdominal wall so that fecal material can pass through a small opening (stoma) into a small plastic bag worn on the front of the abdomen (more information about colostomies can be found in Colostomy Guide). In some cases, it may be possible to remove the cancerous part of the colon (next to the cervix) and reconnect the colon ends so that no bags or external appliances are needed.
If the vagina is removed, a new vagina can be created from skin, intestinal tissue, or muscle and skin (myocutaneous) grafts.
Sexual impact of pelvic exenteration
Recovery from total pelvic exenteration takes a long time. Most people don't begin to feel like themselves again for about 6 months after surgery. Some say it takes a year or two to adjust completely.
Nevertheless, they still can lead happy and productive lives. With practice, they can also have sexual desire, pleasure, and orgasms.
More information about managing the sexual side effects of cervical cancer treatment can be found in How Cancer Surgery Can Affect Sex for Women.
Surgery to remove nearby lymph nodes
When cancer cells break away from a tumor, they can travel to other areas through either the bloodstream or the lymph system. If they travel through the lymph system, the cancer cells may end up in lymph nodes. Most of the escaped cancer cells die or are killed before they can start growing somewhere else. But one or two might settle in a new area, begin to grow, and form new tumors.
Usually during surgery for a radical hysterectomy, the lymph nodes next to the aorta (the large artery in the abdomen) are removed. This is called para-aortic lymph node sampling. The lymph nodes may be sent to the lab during the operation for quick testing. If the para-aortic lymph nodes have cancer cells, the surgery may be stopped, and systemic therapy, such as chemotherapy with or without immunotherapy, given instead. If the lymph nodes do not have cancer cells, then pelvic lymph nodes (see below) are usually removed and the radical hysterectomy completed. Any tissue removed during surgery will be tested to see if the cancer has spread there. If so, radiation therapy with or without chemotherapy may be recommended.
Cancer that starts in the cervix can spread to lymph nodes in the pelvis. To check for lymph node spread, the surgeon might remove some of these lymph nodes. This procedure is known as a pelvic lymph node dissection or lymph node sampling. It is done at the same time as a hysterectomy or trachelectomy.
Removing lymph nodes can lead to fluid drainage problems in the legs. This can cause severe leg swelling, a condition called lymphedema.
Sentinel lymph node mapping and biopsy is a procedure in which the surgeon finds and removes only the lymph node(s) where cancer is most likely to spread first. A radioactive substance and/or blue dye is injected into the cervix at the start of the surgery. These substances travel through the lymphatic vessels along the path cancer cells would likely follow. The first lymph node(s) the dye or radioactive substance reaches is called sentinel nodes. Removing only one or a few lymph nodes helps reduce the risk of side effects from surgery, such as leg swelling, known as lymphedema.
After the substance has been injected, the sentinel node(s) can be found either by using a special machine to detect radioactivity in the nodes, or by looking for nodes that have turned blue. To double check, both methods are often used. The surgeon then removes the node(s) containing the dye or radioactivity.
Sentinel lymph node mapping may be considered for certain cases of stage I cervical cancer. It is best used for tumors that are less than 2 cm (almost one inch) . If your surgeon is planning sentinel lymph node biopsies, you should ask if this procedure is appropriate for you.
Even if sentinel lymph node mapping does not show any lymph nodes to biopsy, the surgeon will most likely still remove the lymph nodes on that side of the pelvis to make sure cancer is not missed. Also, any enlarged or suspicious lymph nodes need to be removed during surgery, even if they do not take up the dye.
More information about surgery
For more general information about surgery as a treatment for cancer, see Cancer Surgery.
To learn about some of the side effects listed here and how to manage them, see Managing Cancer-related Side Effects.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Basaran D, Leitao MM Jr. The Landmark Series: Minimally Invasive Surgery for Cervical Cancer. Ann Surg Oncol. 2021 Jan;28(1):204-211. doi: 10.1245/s10434-020-09265-0. Epub 2020 Oct 30. PMID: 33128120; PMCID: PMC8369473.
Bogani G, Leone Roberti Maggiore U, Rossetti D, Ditto A, Martinelli F, Chiappa V, Ferla S, Indini A, Sabatucci I, Lorusso D, Raspagliesi F. Advances in laparoscopic surgery for cervical cancer. Crit Rev Oncol Hematol. 2019 Nov;143:76-80. doi: 10.1016/j.critrevonc.2019.07.021. Epub 2019 Aug 2. Erratum in: Crit Rev Oncol Hematol. 2020 Jan;145:102833. doi: 10.1016/j.critrevonc.2019.102833. PMID: 31499276.
Shvygin A, Manning-Geist BL, Sonoda Y. Fertility-sparing and minimally invasive surgery for early-stage cervical cancer. J Surg Oncol. 2024 Jan;129(1):112-116. doi: 10.1002/jso.27540. Epub 2023 Nov 30. PMID: 38032090.
van der Plas RCJ, Bos AME, Jürgenliemk-Schulz IM, Gerestein CG, Zweemer RP. Fertility-sparing surgery and fertility preservation in cervical cancer: The desire for parenthood, reproductive and obstetric outcomes. Gynecol Oncol. 2021 Dec;163(3):538-544. doi: 10.1016/j.ygyno.2021.09.003. Epub 2021 Sep 25. PMID: 34583837.
Last Revised: July 1, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



