Your gift is 100% tax deductible.
Your Lung Pathology Report
When samples are collected from your lung during a biopsy (or cytology procedure), they are studied by a doctor with special training, called a pathologist. After testing the samples, the pathologist creates a report that details what was found, which can then be used to help manage your care.
The information here is meant to help you understand medical terms you might find in your pathology report after a lung biopsy. (If you are found to have lung cancer and have surgery to treat it, a separate pathology report would be created after testing the part of the lung that was removed. That report might contain some of the same information below, as well as other information.)
Lung pre-cancers and related conditions
These findings are not lung cancer, but some of them could become cancer if left untreated.
In-situ carcinoma (carcinoma in situ)
Carcinoma is the general medical term for a cancer that starts in the cells that line organs. Neary all lung cancers are carcinomas. In the lung, carcinomas most often start in the cells that line the inside of the bronchi, bronchioles, or alveoli, which are the passageways inside the lung (from biggest to smallest).
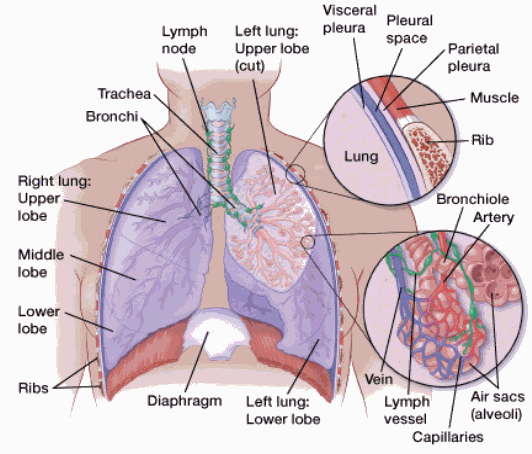
If the carcinoma cells are only in the top layer of cells of the bronchi, bronchioles, or alveoli, without growing into the deeper layers below, it is called in-situ carcinoma or carcinoma in situ (CIS). This is considered a pre-cancer, not a true lung cancer. (Lung cancers, which are also known as invasive or infiltrating carcinomas, are described in more detail below.)
If the report mentions squamous cell carcinoma in situ, adenocarcinoma in situ, or atypical adenomatous hyperplasia…
There are different types of lung pre-cancers, which in turn might become different types of lung cancer if not treated.
- Squamous cell carcinoma in situ (SCIS) is a pre-cancer that can become invasive squamous cell carcinoma (a type of non-small cell lung cancer).
- Adenocarcinoma in situ (AIS) is a pre-cancer that can become adenocarcinoma (another type of non-small cell lung cancer).
- Atypical adenomatous hyperplasia (AAH) is a very small tumor made up of abnormal (atypical) gland cells that can progress to AIS, and might eventually become adenocarcinoma if not treated.
If either SCIS or AIS is seen in a small biopsy sample (such as from a bronchoscopy or CT-guided needle biopsy), invasive carcinoma (cancer) might still be present in another part of the lung tumor that wasn’t sampled with the biopsy, so more tests might be needed.
If SCIS or AIS is found when a tumor is removed (resected) completely, and no invasive cancer is found, a person’s prognosis (likely outcome) is usually very good. However, there’s still a chance there could be other areas of pre-cancer in the lung that are not near the one that was removed (sometimes called multifocal disease). This is something that will be looked for very carefully on any follow-up (surveillance) imaging tests, such as chest CT scans.
SCIS or AIS isn’t likely to be important if it’s mentioned in a report in which invasive carcinoma (cancer) was also found.
If the report mentions squamous metaplasia…
When an air passage in the lung is irritated (such as from smoking or infection), the cells lining the passage can change in shape. Instead of looking like rectangles standing up next to each other, the cells begin to flatten and stack on top of each other. This change is called squamous metaplasia because the cells now look like squamous (flat) cells.
Squamous metaplasia is not considered a pre-cancer, but if the irritation persists it can progress to squamous dysplasia.
If the report mentions squamous dysplasia…
Squamous dysplasia is an early form of pre-cancer in which the squamous cells lining an air passage look abnormal, but not quite like cancer cells. It is often separated into different categories based on how abnormal the cells and tissue appear under the microscope:
- When it is the least abnormal, it is called mild dysplasia.
- When it is most abnormal, it is called severe dysplasia.
- Moderate dysplasia is in between the other two.
The more severe the squamous dysplasia is, the more similar it is to squamous cell carcinoma in situ (see above). If squamous dysplasia is seen on a biopsy, it might mean that there is something more serious, like in-situ or invasive carcinoma, somewhere else in the lung that wasn’t sampled on this biopsy.
Lung cancer types and descriptions
Carcinoma
Carcinoma is the general medical term for a cancer that starts in the cells that line organs. In the lung, carcinomas can start in the cells that line the inside of the bronchi, bronchioles, and alveoli, which are the passageways inside the lung (from biggest to smallest). Carcinoma is by far the most common kind of lung cancer.
Once carcinoma cells have grown deeper than the top layers of cells in the lung passageway, the cancer is called an invasive or infiltrating carcinoma. At this point the cancer cells can spread (metastasize) outside of the lung to lymph nodes and other parts of the body. Invasive carcinomas are considered true lung cancers and not pre-cancers.
There are different types of lung carcinomas. They are named based on how the cells look under the microscope.
Squamous carcinoma or squamous cell carcinoma
Squamous carcinoma or squamous cell carcinoma is a type of non-small cell lung cancer (NSCLC) where the cells look like the flat cells (called squamous cells) that line the airways. It is a common type of lung cancer in the United States.
Adenocarcinoma
Adenocarcinoma is a type of non-small cell lung cancer (NSCLC) where the cells look like gland cells, such as the glands that secrete mucus in the lungs. This is the most common type of lung cancer in the United States.
If the report mentions lepidic, papillary, micropapillary, acinar, mucinous, or solid adenocarcinoma…
These terms describe different types of lung adenocarcinoma, which are based on how the cells look and are arranged under the microscope (called growth patterns). Some tumors look basically the same throughout the tumor, and some look different in different areas of the tumor. Some growth patterns have a better prognosis (outlook) than others.
Since some tumors can have a mixture of patterns, the pathologist can’t always tell all the types contained in a tumor just based on a biopsy that samples only a small part of the tumor. To know what types a tumor contains, the entire tumor must be removed.
Small cell carcinoma
Small cell carcinoma (also known as small cell lung cancer, or SCLC) is a type of lung cancer that starts in neuroendocrine cells, which are like nerve cells in some ways, and like hormone-making endocrine cells in other ways. As the name implies, these cancer cells look smaller than other types of lung cancer cells when seen under a microscope.
Small cell lung cancer tends to grow and spread quickly. Because of this, it is often treated differently from most types of non-small cell lung cancer.
Non-small cell carcinoma
If the cancer clearly doesn’t look like small cell carcinoma under the microscope, but it can’t be identified as either a squamous cell carcinoma or adenocarcinoma (the two main types of NSCLC), the term non-small cell carcinoma might be used.
Telling squamous cell carcinoma from adenocarcinoma can be especially hard if the biopsy sample was small. These tumors may be more precisely classified later with special lab tests (such as immunohistochemistry), or when the entire tumor is removed during surgery and then examined.
Carcinoid tumor
Carcinoid tumors start from cells of the diffuse neuroendocrine system. This system is made up of cells that are like nerve cells in some ways and like hormone-making endocrine cells in other ways. These cells are scattered throughout the body in organs like the lungs, stomach, and intestines.
Like other cells in your body, the lung neuroendocrine cells can sometimes go through changes that cause them to grow too much and form tumors. These are known as neuroendocrine tumors or neuroendocrine cancers. (Neuroendocrine cells in other parts of the body can also form tumors and cancers.)
Typical carcinoid tumors tend to be slow growing, and only rarely spread outside the lungs.
Atypical carcinoid tumors are much less common than typical carcinoids. They tend to grow a little faster and are somewhat more likely to spread to other organs. Seen under a microscope, atypical carcinoids have more cells in the process of dividing and look more like a fast-growing tumor. Some of the features of an atypical carcinoid that may be mentioned in your report include: mitotic figures or mitoses (an indication of how fast the tumor is growing) and necrosis (areas of the tumor that are dead).
Some carcinoid tumors can release hormone-like substances into the bloodstream, which might cause symptoms. Lung carcinoids do this far less often than carcinoid tumors that start in the intestines.
To learn more about these tumors, see Lung Carcinoid Tumor.
Some other types of lung cancer can start in neuroendocrine cells, including small cell carcinoma (SCLC – see above) and large cell neuroendocrine cancer (LCNEC). Unlike carcinoids, these cancers tend to grow and spread quickly. To learn more, see What Is Lung Cancer?
Other types of cancer found in or near the lungs
Mesothelioma
Mesotheliomas are not lung cancers, because they don’t develop from cells in the lung. Instead, these cancers start in the lining on the outside of the lung, called the pleura (and the cancers are called pleural mesotheliomas).
Mesotheliomas are often described based on how they look under the microscope with terms like epithelioid, sarcomatoid, or mixed (epithelioid and sarcomatoid). Mesotheliomas are sometimes linked to exposure to asbestos.
To learn more about these cancers, see Mesothelioma.
Metastatic carcinoma to the lung
Cancers that start in other organs often spread (metastasize) to the lungs. This is common because all blood flows through the lungs. Cancer cells that have broken away from the main tumor can travel through the blood and lodge in the lungs, where they can start new tumors.
Cancers that have spread to the lung from another organ are still named after where they started — they are not considered lung cancers. For example, if an adenocarcinoma of the colon (colon cancer) spreads to the lung it is still a colon cancer, and not a lung cancer. This is important because treatment for an adenocarcinoma of the lung is different from treatment for adenocarcinoma of the colon.
Other terms that might be on the pathology report
Margins and ink
When an entire tumor or abnormal area is removed, the pathologist coats the outer edges, or margins, of the tissue with ink, sometimes with different colored ink on different sides. This is done so that the margin can be seen easily under the microscope.
If something abnormal (such as a cancer or pre-cancer) is found, the pathologist can tell if it is at the edges of the removed tissue. This is known as a positive margin. If it is, it may mean that some cancer (or pre-cancer) has been left behind. Sometimes this is not a concern because the surgeon removed other tissue in that area. Still, if some cancer (or pre-cancer) has been left behind, you might need more treatment. Talk with your doctor about the best approach for you if cancer (or pre-cancer) is found at the margins.
Scarring, emphysema, emphysematous changes, or inflammation
All of these are terms for non-cancerous changes that the pathologist might see under the microscope. They are usually not important when seen on a biopsy sample that also has pre-cancer or cancer. Pathologists mention them for completeness, as they may help answer other questions about your health that come up later.
Granulomas, (Grocott) methenamine silver stain (GMS), acid fast bacilli (AFB), or Periodic Acid Schiff (PAS)
Granulomas are common structures seen under the microscope that can be caused by certain types of infections or other diseases such as sarcoidosis, allergic reactions, or dust-induced lung disease (pneumoconiosis).
Granulomas can also be a reaction in the lung tissue to a lung tumor. If this is the case, they have no significance for the treatment of your lung tumor.
Germs causing a lung infection (and, therefore, granulomas) typically can only be seen if the pathologist applies special stains (such as GMS, AFB or PAS stains) to the biopsy samples on the microscope slides. In most situations, these stains won’t show any germs, but they are often done just to be sure a granuloma isn’t caused by an infection.
Lab tests that might be done on biopsy samples
If the pathologist sees cancer cells in the biopsy (or surgery) samples, different types of lab tests might be done to help tell what type of cancer cells they are.
These tests are often immunohistochemical (IHC) stains done on very thin slices of the biopsy samples, which are placed on glass slides and viewed under a microscope. Sometimes other types of lab tests are done as well.
p63, p40, cytokeratin 5/6 (CK5/6), TTF-1, and/or napsin A
Stains for p63, p40, cytokeratin 5/6, TTF-1, and napsin A are special tests that the pathologist might use to help tell between an adenocarcinoma and a squamous cell carcinoma.
CK7 (cytokeratin 7), CK20, CDX2, gross cystic disease fluid protein (GCDFP), mammaglobin, estrogen receptor (ER), or progesterone receptor (PR), and/or TTF-1
These tests are sometimes used to help tell if a cancer in the lung started there (that is, if it’s a primary lung cancer) or if it spread there from some other organ (that is, if it metastasized from somewhere else). These tests aren’t always needed, so if your report doesn’t mention them, it doesn’t mean there is a problem or a question about your diagnosis.
CD56, chromogranin, or synaptophysin
These tests are sometimes used to help tell if a lung cancer is a tumor of the neuroendocrine system – that is, if it’s a typical carcinoid, atypical carcinoid, small cell carcinoma, or large cell neuroendocrine carcinoma (see above).
D2-40 (podoplanin), calretinin, WT-1, BAP-1, CEA, cytokeratin (CK) 5/6, HBME-1, Ber-EP4, TTF-1, and/or CD15 (LeuM1)
These tests are sometimes used to help tell if a tumor that includes the lining of the lung (pleura) is a mesothelioma (see above) or an adenocarcinoma of the lung.
EGFR, K-RAS, ALK, BRAF, ROS1, RET, MET, HER2, and/or NTRK
If a type of non-small cell lung cancer is found (such as a squamous cell carcinoma or adenocarcinoma), tests might be done on the cancer cells to look for changes in these gene or proteins (which are sometimes called biomarkers).
These tests can show if you might be helped by treatment with a targeted drug that affects cancer cells with these changes. This type of testing is sometimes referred to as precision (or personalized) medicine. How the test results might affect your treatment is best discussed with your doctor.
PD-L1
If a type of non-small cell lung cancer is found (such as a squamous cell carcinoma or adenocarcinoma), this test might be done to look for the PD-L1 protein on the cancer cells. In some situations, it can show if you might be helped by treatment with an immunotherapy drug. How the results of your tests might affect your treatment is best discussed with your doctor.
Other information if lung cancer has been found
If any type of lung carcinoma (cancer) is found, the pathologist might provide other information about the cancer in the pathology report.
Cancer grade (differentiated, moderately differentiated, or poorly differentiated)
If carcinoma is found, the pathologist will likely assign it a grade, based on how the cancer cells look under a microscope:
- Well differentiated (low-grade) carcinomas tend to look a lot like the type of cells from which they arose.
- Moderately differentiated (intermediate-grade) carcinomas retain only some of the features of the cells from which they arose.
- Poorly differentiated (high-grade) carcinomas look very different from the cells from which they arose.
The grade of the cancer is often related to how fast it is likely to grow and spread (with poorly differentiated cancers tending to grow the fastest). For many types of cancer, the grade is important in determining a person’s prognosis (outlook), as well as the best treatment options.
The grade typically doesn’t affect treatment options for most lung cancers. However, for the non-mucinous type of lung adenocarcinoma, the presence of more than 20% of what are considered “high-grade” (poorly differentiated) components (solid, micropapillary, cribriform, or complex glandular patterns) is linked with worse outcomes.
Tumor size
If the entire tumor has been removed, the pathologist will measure its size by looking at it (called the gross examination), or, if it is very small, measure it under the microscope.
Often, what is reported is how big across it is in the area where the tumor is the largest. This is called the greatest dimension of the tumor, as in “the tumor measured 2.2 centimeters (cm) in greatest dimension.” In general, smaller tumors have a better prognosis (outlook).
A biopsy typically only samples a part of the tumor, so measurements of its overall size aren’t included in a biopsy pathology report. In this case your doctor will most likely rely on tumor measurements from an imaging test such as a CT scan to help determine the stage of the cancer (see below) and how it might affect your treatment options.
Cancer stage
The stage of the cancer is a measure of the extent of the cancer, including its spread to other parts of the body.
TNM categories
The stage of a lung cancer is based on 3 main pieces of information, each of which is represented by a letter:
- T stands for the main (primary) tumor (its size and if it has grown into nearby structures).
- N stands for spread to nearby lymph nodes.
- M is for metastasis (spread) to distant parts of the body.
Each category is assigned a number (and sometimes a lowercase letter), based on how much cancer there is (for example, T1a, N0, M0, etc.), with higher numbers (and letters) used for more advanced cancers.
Once the T, N, and M categories have been determined, they are combined to create an overall stage, which is given a number from I (1) to IV (4), sometimes followed by an uppercase letter (for example, stage IIIB). Again, higher stage numbers (and letters) mean the cancer is more advanced.
If the report is for a biopsy specimen, staging information is not usually given, because the pathologist would need to have the entire tumor and nearby lymph nodes to determine the T and N categories.
If surgery has been done to remove a lung tumor and nearby lymph nodes, the staging information is indicated by a lower-case letter “p” put before the T and N. So, in your pathology report, pT would be followed by numbers and letters based on the size of the tumor and some other information about it. pN would be followed by numbers and letters based on the extent of spread to nearby lymph nodes that may have been removed at the same time as the lung tumor.
The pathologist typically does not report the M category, as they often cannot determine whether there is spread to distant parts of the body just based on surgery to remove a lung tumor and nearby lymph nodes. The M category is often based on the results of imaging tests such as CT scans, MRIs, and PET scans, sometimes along with a biopsy of an area of suspected cancer spread.
Ask your doctor how the stage of your cancer might affect your treatment.
Vascular, lymphatic, angiolymphatic, or lymphovascular invasion
Tumors sometimes grow into small blood vessels and/or lymphatic vessels. When this is seen under the microscope it is called vascular, lymphatic, angiolymphatic or lymphovascular invasion. If cancer cells are present in these vessels, it means there is a higher chance that the cancer has spread outside the lung, although this does not always occur. Talk to your doctor about how this finding might affect your treatment.
D2-40 (podoplanin) and CD34
D2-40 and CD34 are special tests (immunohistochemical stains done on tissue slides) the pathologist might use to help identify vascular, lymphatic, lymphovascular, or angiolymphatic invasion. These tests are not always needed.
- Written by

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
Last Revised: July 7, 2023
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



