Cancer-related Fatigue
Many people with cancer have fatigue (a feeling of being very tired, low-energy, and worn out). This can happen before, during, and after treatment. Some people report that their fatigue lasts for weeks, months, or even years after they finish cancer treatment.
There are steps you can take to help manage your cancer-related fatigue.
What is cancer-related fatigue?
Cancer-related fatigue (CRF) is a physical, emotional, and mental feeling of tiredness or exhaustion in someone with cancer. This feeling doesn’t get better with rest and sleep.
CRF is often worse and harder to manage than the fatigue people who don’t have cancer get. It can happen whether or not you are in cancer treatment.
What causes cancer-related fatigue?
Cancer-related fatigue can be a symptom of cancer itself. This is especially true if your cancer is more advanced. But there are also many other things that can cause CRF.
This includes:
Certain cancer treatments
Certain cancer treatments can cause fatigue. For example:
- Chemotherapy. Fatigue starts in the days after a chemotherapy treatment and usually gets better before your next treatment.
- Radiation therapy. Fatigue often starts a few weeks after beginning radiation therapy and is at its worst near the end of treatment. It then gets better over the next weeks and months.
- Immunotherapy. Fatigue most often starts in the first few weeks to months of immunotherapy. But it can happen at any time during your treatment, depending on the type of immunotherapy you get.
- Surgery. Fatigue starts right after surgery and gets better as you heal.
Anemia
Certain treatments, like chemotherapy, radiation therapy, and surgery can cause the number of red blood cells in your body to go down. When this happens, it’s called anemia. Anemia can cause fatigue.
Pain
Living with pain can wear you out and make you feel tired. Many pain medicines can also cause drowsiness and fatigue.
Distress, anxiety, and depression
Strong emotions, moods or mental health issues can cause or make fatigue worse. Fatigue may also make these emotions stronger.
Sleep problems
Many people with cancer have insomnia (trouble falling asleep or staying asleep). Not getting enough sleep, or good quality sleep, can make you feel more tired during the day.
Other problems such as sleep apnea and restless leg syndrome can also prevent you from sleeping well.
Sleep apnea is rarely caused by cancer or cancer treatment. It is usually something a person has before they are diagnosed with cancer. Like sleep apnea, restless leg syndrome can happen to people who don’t have cancer. But some people get it during chemotherapy.
Problems eating and drinking
A well-balanced diet and plenty of liquids can help reduce fatigue. But people with cancer often have problems getting enough to eat and drink because of:
- Loss of appetite
- Nausea and vomiting
- Mouth sores and pain
- Mouth dryness or thick saliva
- Trouble swallowing
- Taste and smell changes
Not getting enough physical activity
Too much time spent resting or sitting can lead to fatigue, loss of body function, and muscle weakness.
Medicines
Some medicines can make you feel sleeper and more tired. Pain medicines, antihistamines, and medicines to help you relax or sleep are the ones most likely to worsen fatigue.
Other health conditions
You might have other health conditions that make your cancer-related fatigue worse. This is especially true if you are older. Other health conditions that can worsen fatigue include: arthritis, heart or breathing problems, and hormone problems.
Symptoms of fatigue
People with cancer-related fatigue often describe feeling very tired, weak, exhausted, weary, or worn-out. Fatigue can make it hard for you to keep up with your work, social life, or daily routine. For some people with cancer, fatigue can cause even more distress than side effects like pain, nausea, or vomiting.
Cancer-related fatigue might make you feel:
- Tired in a way that doesn’t get better with rest or sleep
- More tired than usual during or after an activity
- Too tired to do the things you normally do
- Like your arms and legs are heavy and hard to move
- Like you have no energy
- Sad, cranky, or frustrated
- Very weak
- Like you can’t concentrate or focus your thoughts
- Like you need more sleep (or you might have trouble sleeping)
Your fatigue can be different from one day to the next. Some days it might be worse or bother you more. Cancer-related fatigue may take weeks or months to totally resolve, but it gets better over time.
Is it fatigue or weakness?
Fatigue and weakness are often used to describe the same thing, but they are not the same. Fatigue means having a lack of energy. Weakness means feeling like you have less muscle strength. Both fatigue and weakness make it harder to do your usual activities, but for different reasons.
Is it fatigue or depression?
Some symptoms of fatigue might seem a lot like symptoms of depression. You can have fatigue and not be depressed, but some people have both.
Talk with your doctor or cancer care team if you have symptoms that seem like depression or fatigue. They may want you to see a mental health provider to figure out if depression is part of the problem. If it is, treatment might help.
Describing your fatigue to your health care team
Your health care team can suggest ways to manage your fatigue. But first, they need to understand how it makes you feel. To do this, they might ask you to rate and describe your fatigue. There aren’t any lab tests or x-rays to diagnose fatigue, so the best measure is how you describe it.
You might be asked to rate your fatigue as none, mild, moderate, or severe. Or you might be asked you to rate your fatigue on a scale.
Fatigue is often rated on a scale of 0-10. Using this scale, 0 means no fatigue at all, and 10 means the worst fatigue you can imagine.
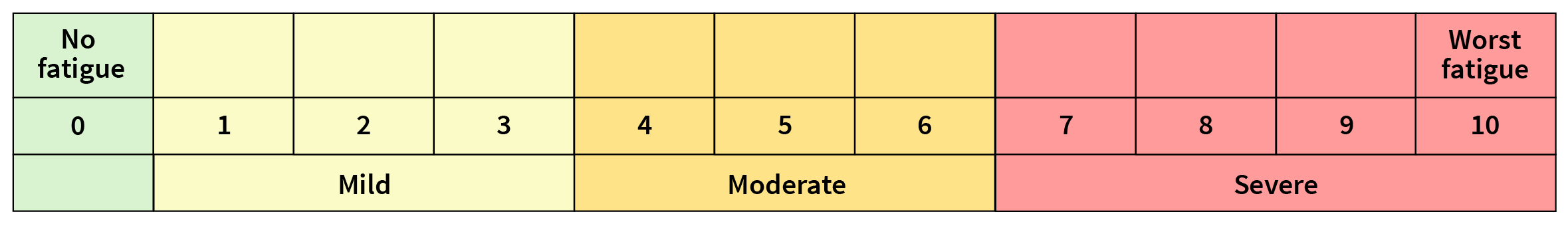
If you have any fatigue, your health care team will probably ask you for more details.
You might be asked:
- When did your fatigue first start?
- How long has it lasted?
- Has it gotten better or worse over time?
- Does anything make it better? Worse?
- Are there times of day you notice it more?
- How has it affected the activities you enjoy or the things you do every day?
Treatment for fatigue
How your health care team treats your fatigue will depend on the cause and symptoms.
Common treatments for fatigue include:
Medicines, supplements, and transfusions
Your cancer care team may prescribe medicines that might make you feel more alert and awake. Check with your cancer care team before taking any medicines or supplements that they didn’t tell you to take. Some medicines and supplements might interact with your cancer treatment.
If you have anemia (low red blood cells), your treatment will depend on how low your red blood cell count. You might be given supplements, medicines to help your body make more red blood cells, or transfusions.
Pain control
If pain is adding to your fatigue, your health care team will work with you to come up with a pain control plan. This might include medicines and non-medical ways of managing your pain.
Counseling and stress management
Your emotions, moods, and mental health could make your fatigue worse. Counseling, stress management, and relaxation exercises might help you cope and learn to deal with the tiredness you feel.
Sleep therapy
If you’re having problems sleeping, or if you’re sleeping too much, your cancer care team might suggest sleep therapy. This therapy can help you sleep better, wake up less, and learn ways you can change your routine to get a more restful night’s sleep.
Physical activity
Lack of physical activity can make fatigue worse. If you would like help finding a safe physical activity plan, ask your health care team to refer you to a physical therapist or other exercise specialist.
Nutrition
Some people with cancer have a hard time eating a diet with enough nutrients. Your cancer care team may want to check and see if you if you have enough vitamins and minerals in your body.
It also might help for you to talk with a registered dietician (RD) if you are having trouble eating. An RD is an expert in nutrition, food and diet and can give you ideas about how to eat more food and drink fluids.
Palliative care
Many people with cancer-related fatigue have other side effects as well. If so, your cancer care team might suggest that you work with a palliative care team.
Palliative care helps patients and caregivers manage the symptoms of cancer and side effects of cancer treatment at any point after diagnosis.
Tips for managing fatigue
There are many things you can do to help manage your fatigue, including:
Physical activity and exercise
Be as active as you can. Start slowly and add more activity as you are able.
Try to be get some physical activity each day. Even short walks can ease fatigue and help you feel better.
Combine aerobic activity and weight training. Try to get a combination of aerobic activity (walking, riding a bicycle, swimming, etc.) and resistance training (weights).
Try other types of activity. Activities like yoga, tai chi, or stretching can also help ease fatigue.
Follow a daily routine. Keep as normal a level of activity as you can.
Check with your doctor or cancer care team before you become more physically active if you have:
- Cancer that has spread to your bones (bone metastasis)
- Low platelet count
- Fever or active infection
- Anemia (low red blood cell counts)
- Balance problems, weakness, or other problems the make it more likely that you will fall
Energy conservation
Rest, but not too much. Too much rest can lower your energy level and make it harder to sleep at night.
Focus on important things first. Decide which things you most need or want to do and focus on those first. Do them during times when you have the most energy.
Put items in reach. Put things that you use most often within easy reach.
Ask for help. Ask your family or friends to help with the things you find tiring or too hard to do. Their support might help you cope better with your fatigue.
Lowering your stress
Try yoga, Qigong, meditation, or mindfulness and relaxation exercises. These exercises might lower your stress. If you want help getting started, check with your cancer care team for resources.
Consider counseling. Counseling, either on your own or in a group, can help you find ways to cope with your cancer, symptoms, and side effects.
Try massage or touch therapy. These therapies have helped some people with cancer lower their stress levels and sleep better. Talk to your cancer care team before starting massage therapy.
Join a support group. This could help you share your concerns and learn how others have coped. Ask your cancer care team about support groups in person or online.
Trying to get good sleep
Try to sleep 7 to 8 hours each night. Regular bed and wake times along with a sleep routine might help.
Take only short naps or rest breaks. Try to limit your naps and rest breaks to less than 30 minutes during the day. Longer naps can make it harder to go to sleep at night.
Exercise, but not right before bed. Try to exercise at least 30 minutes a day but at least 2 hours before bedtime. Choose a time of day when you have enough energy to be active.
Avoid caffeine before bed. Avoid caffeine at least 4 hours before bedtime.
Eating well
Eat a balanced diet. Try to eat a diet that includes protein, fruits, vegetables, and whole grains.
Stay hydrated. Drink fluids throughout the day to stay hydrated.
Meet with a registered dietician. Ask your cancer care team about meeting with a registered dietician if you are having trouble eating. They can check to see if you are getting the calories and nutrients you need to keep your energy up.
When to call your health care team
Call your health care team or cancer care team if:
- You feel too tired to get out of bed for a 24-hour period.
- You have problems waking up.
- You have problems catching your breath when you are active.
- Your fatigue seems to be getting worse.
These may be signs of other problems that need to be treated.
When to go to the emergency room or call 911
Call 911 or go to the emergency room if:
- You feel confused, dizzy, lose your balance, or fall.
- You feel short of breath even when resting.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Albrecht TA, DeGennaro R. Cancer-related fatigue. In: Eggert JA, Byar KL & Parks LS, ed. Cancer Basics. Oncology Nursing Society; 2022: 301-312.
Alnawwar MA, Alraddadi MI, Algethmi RA, Salem GA, Salem MA, Alharbi AA. The Effect of Physical Activity on Sleep Quality and Sleep Disorder: A Systematic Review. Cureus. 2023;15(8):e43595. Published 2023 Aug 16.
American Society of Clinical Oncology. Fatigue. Cancer.net. Accessed on April 1, 2024.
Azeem Khan M, Florou V, Swami U. Immunotherapy and fatigue: what we know and what we don't know. Oncotarget. 2021;12(8):719-720.
Bower JE, Bak K, Berger A, et al. Screening, assessment, and management of fatigue in adult survivors of cancer: an American Society of Clinical Oncology clinical practice guideline adaptation. J Clin Oncol. 2014;32(17):1840-1850.
National Comprehensive Cancer Network. (NCCN). Cancer-related fatigue. Version 2.2024 Accessed at www.nccn.org on April 1, 2024.
Tschanz JA. Fatigue. In: Camp-Sorrel D, Hawkins RA, Cope DG, eds. Clinical Manual for the Advanced Practice Nurse. Oncology Nursing Society; 2022: 1289-1297.
Last Revised: July 16, 2024
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.


