Your gift is 100% tax deductible.
Blood Type Testing and Matching Before a Transfusion
Before a transfusion, your blood will be tested to make sure it matches the blood you get.
The main blood tests done before a transfusion are:
- Type
- Antibody screen
- Crossmatch
These tests are important because if you get a transfusion of a blood type that doesn’t work with yours, your immune system might attack the donated blood. This can cause a serious or even life-threatening transfusion reaction.
Blood type testing
Donated blood is always tested to find out the type. This is done when it’s taken from the donor and again in the hospital lab. If you need a blood transfusion, a sample of your blood is tested the same way.
Determining your blood type
The type of blood you have depends on the presence or absence of certain antigens in your blood. (Antigens are substances that trigger your body’s immune response.)
The antigens that affect your blood type are:
- ABO antigen: Everyone has either type A, B, AB, or O blood. This means that their blood cells have either antigen A (type A), antigen B (type B), both antigens (type AB), or neither antigen (type O).
- Rh factor: Everyone is either Rh-positive or Rh-negative (you either have Rh or you don’t).
Your ABO antigen + Rh factor = your blood type.
There are 8 different blood types:
- A positive and A negative
- B positive and B negative
- AB positive and AB negative
- O positive and O negative
In the United States, the most common blood type is O, followed by type A.
ABO blood type matching
When you get a transfusion, your blood is matched based on your ABO blood type (see above for more on this).
ABO blood type: the type of antigens you have on your blood cells (A, B, A+B, or neither).
These antigens are linked with the antibodies in your plasma. Antibodies are proteins in your immune system that watch for and attack foreign substances.
This is why it’s so important to match ABO blood types.
For example: If you have type A blood, your blood cells have A antigens, and your body makes anti-B antibodies. These antibodies attack any donor blood with B antigens, so you can’t get type B or AB blood.
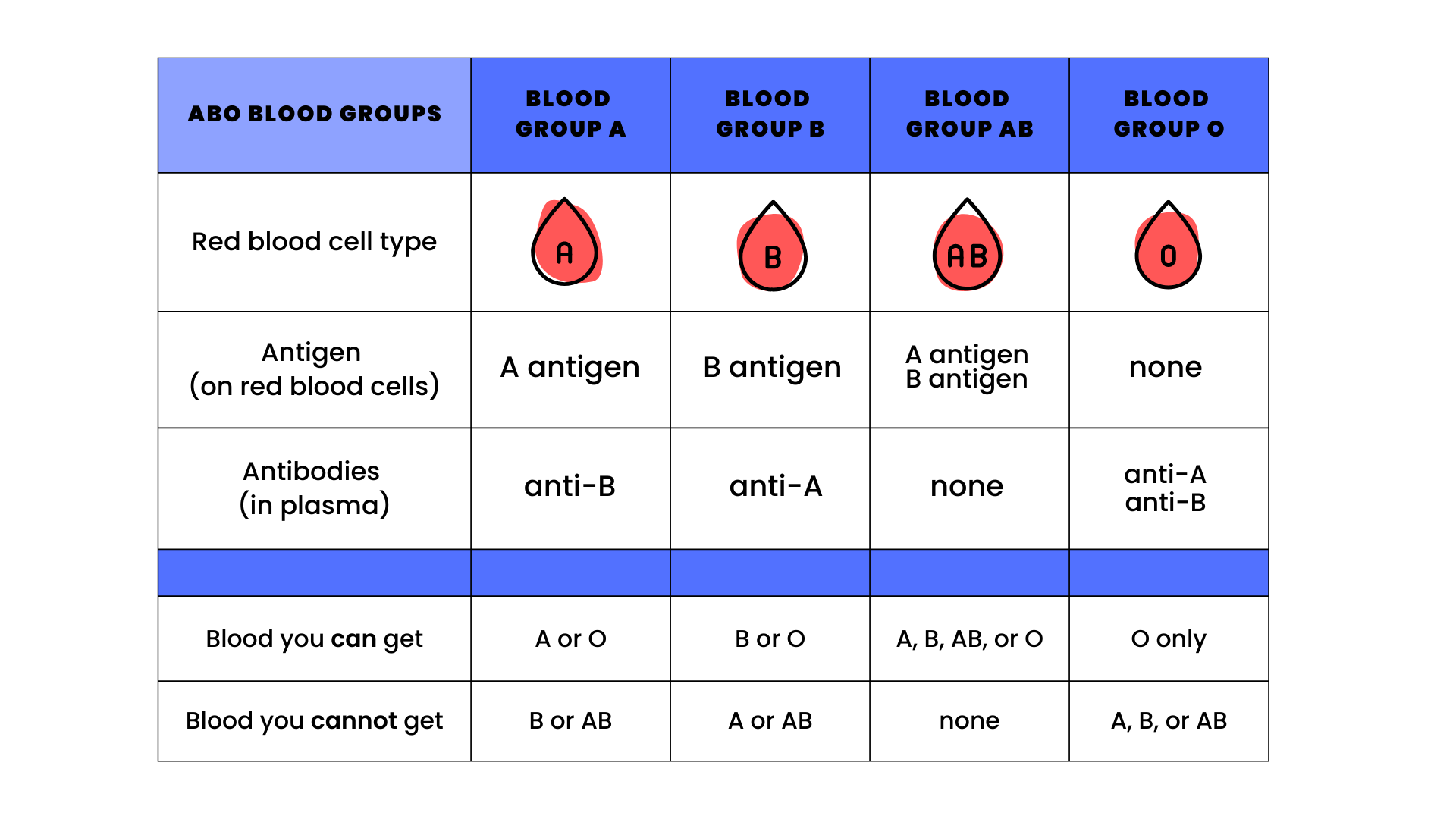
If you have type A blood with A antigens, you also make anti-B antibodies. You can’t get type B or AB blood, because your anti-B antibodies would attack any donor blood with B antigens.
You can only get type A or O blood.
If you have type B blood with B antigens, you also make anti-A antibodies. You can’t get type A or AB blood, because your anti-A antibodies would attack any donor blood with A antigens.
You can only get type B or O blood.
If you have type AB blood with A and B antigens, you don’t make anti-A or anti-B antibodies. People with AB blood are sometimes called universal receivers.
You can get transfusions from any blood type.
If you have type O blood with no A or B antigens, you make both anti-A and anti-B antibodies. You can’t get type A, B, or AB blood because your anti-A and anti-B antibodies would attack any donor blood with A or B antigens.
You can only get type O blood.
But since type O has no antigens, anyone of any blood type can receive type O blood. This is why people with type O blood are sometimes called universal donors.
Rh factor matching
In addition to matching ABO types, your blood is also matched by Rh (rhesus) factor. Rh factor is another protein that some people have on their red blood cells.
- If you have Rh-positive blood: You have the Rh antigen on your blood cells, so your body doesn’t make anti-Rh antibodies. You can get Rh-positive or Rh-negative red blood cell transfusions.
- If you have Rh-negative blood: You don’t have the Rh antigen on your red blood cells, so your body can make anti-Rh antibodies. An Rh-positive blood transfusion can cause a person with Rh-negative blood to make antibodies against the Rh antigen. This can lead to a transfusion reaction. You should only get Rh-negative red blood cells, except in emergencies.
Other antigens
Other antigens on red blood cells can also lead to transfusion reactions. This is rare because your body doesn’t make antibodies against these antigens unless you’ve had transfusions before. These antigens may become a problem in matching blood if you’ve had many transfusions in the past.
Blood type matching for plasma, platelet, and cryo transfusions
Plasma transfusions: Blood type is also important for plasma transfusions, but the rules are different from the rules for red blood cell transfusions (discussed above). For example, people with type AB blood are universal plasma donors.
- Anyone can receive AB plasma.
- Someone who is AB can only receive type AB plasma.
Platelet and cryo transfusions: For platelet and cryo transfusions, it isn’t necessary to match the blood type of the donor to the recipient. But many labs still try to match them. If you get frequent platelet or cryo transfusions, matching may lower your risk of future transfusion reactions.
Antibody screen
After your blood is typed, the lab does a test called an antibody screen to see if your plasma has antibodies other than those against A, B, and Rh. If there are extra antibodies, testing may take longer. This is because some units of donor blood may not fully match yours, even though they have the same ABO and Rh types.
Crossmatching
Before you can get a red blood cell transfusion, another test called a crossmatch must be done.
For a crossmatch, a small amount of donor blood is mixed with your blood to see if they react before the blood is transfused. If the two blood samples clump together, they aren’t a good match and that donor’s blood won’t be used for you.
A crossmatch usually isn’t needed for platelet or plasma transfusions unless the platelets look like they could have some red blood cells.
Other testing
Other testing might be done depending on the person. For example, some people with cancer need CMV-negative blood. CMV (cytomegalovirus) is a common infection that most people get at some point, but don’t have symptoms. But if someone with a weakened immune system gets CMV-positive blood, it can cause serious problems.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
American Red Cross. Facts about blood and blood types. Updated 2025. Accessed at www.redcrossblood.org/donate-blood/blood-types.html on July 15, 2025.
American Red Cross. What happens to donated blood. Updated 2025. Accessed at www.redcrossblood.org/learn-about-blood/what-happens-donated-blood/blood-testing on July 15, 2025.
Association for the Advancement of Blood & Biotherapies. Patient blood management. Accessed at www.aabb.org/news-resources/resources/patient-blood-management on July 15, 2025.
Auerbach, M, DeLoughery, TG. Treatment of iron deficiency and iron deficiency anemia in adults. UpToDate. 2025. Accessed at https://www.uptodate.com/contents/treatment-of-iron-deficiency-and-iron-deficiency-anemia-in-adults on July 17, 2025.
Centers for Disease Control and Prevention (CDC). NHSN biovigilance component hemovigilance module surveillance protocol. V2.9. Updated March 2025. Accessed at https://www.cdc.gov/nhsn/pdfs/biovigilance/bv-hv-protocol-current.pdf on July 16, 2025.
Centers for Disease Control and Prevention (CDC). Transfusion complications monitoring. Updated May 15, 2024. Accessed at https://www.cdc.gov/sickle-cell-research/php/transfusion-complications/ on July 15, 2025.
Lenet T, Baker L, Park L, et al. A Systematic Review and Meta-analysis of Randomized Controlled Trials Comparing Intraoperative Red Blood Cell Transfusion Strategies. Ann Surg. 2022;275(3):456-466.
National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Hematopoietic growth factors. Version 1.2025. Accessed at www.nccn.org on July 15, 2025.
Sieff, CA. Introduction to recombinant hematopoietic growth factors. UpToDate. 2023. Accessed at https://www.uptodate.com/contents/introduction-to-recombinant-hematopoietic-growth-factors on July 15, 2025.
Taheri Soodejani M, Haghdoost AA, Okhovati M, et al. Incidence of adverse reaction in blood donation: a systematic review. Am J Blood Res. 2020;10(5):145-150.
Tibi P, McClure RS, Huang J, et al. STS/SCA/AmSECT/SABM Update to the clinical practice guidelines on patient blood management. Ann Thorac Surg. 2021;112(3):981-1004.
Uhl, L. Pretransfusion testing for red cell transfusion. UpToDate. 2025. Accessed at https://www.uptodate.com/contents/pretransfusion-testing-for-red-blood-cell-transfusion on July 15, 2025.
Last Revised: August 22, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



