Your gift is 100% tax deductible.
Intravenous (IV) Lines and Ports Used in Cancer Treatment
IV lines and ports are used a lot during cancer treatment. Knowing what they are, why they’re used, and how to care for them helps you better manage your care.
What is intravenous (IV) therapy?
An IV line is used to deliver medicines, fluids, blood products, or nutrition into a patient’s bloodstream. A flexible tube (called an IV line or catheter) is put through the skin into a vein. This may also be called infusion therapy.
Many types of infusions are given through an IV:
- Chemotherapy (chemo)
- Targeted therapy
- Immunotherapy
- Blood products
- Anti-nausea medicines
- IV fluids
- Electrolytes (such as potassium, magnesium)
- Antibiotics
- Nutrition
IV therapy can be given in the hospital, clinic, doctor’s office, or even at home.
Types of IV lines (catheters) and ports
IV lines (catheters) and ports are both used in cancer treatment to deliver medicines or draw blood, but in different ways.
- IV lines (catheters) are tubes that go directly into the body and are partly on the outside. They usually are temporary.
- Ports are devices placed under the skin and connect to a vein by a catheter inside the body. They are more permanent.
The type of IV catheter you have will depend on what you need it for, how often and for how long you need it, what your doctor recommends, and what your preferences are. Types of IVs that may be used are:
- Peripheral IVs
- Midline catheters
- Central venous catheters
Peripheral IVs (or IVs)
Peripheral IVs are short, hollow tubes that are usually put through the skin into a vein in the hand or arm. A nurse or other health care provider will place the IV and put a clear plastic dressing on top.
Peripheral IVs can only be used for a few days, so they are a better choice for short-term treatments. Medicines that can damage veins should not be given through a peripheral IV.
Midline catheters
Midline catheters are like CVCs, but they are shorter and don’t go all the way to the superior vena cava (SVC). Instead, they end in a vein in the upper arm. For this reason, they are considered peripheral lines. Midlines may be used when a person has fragile veins or needs medicines for days to weeks. Because infection is generally less likely with a midline, it is sometimes preferred over a CVC. But midlines can’t be used to give medicines that can damage veins or those that require a CVC (like TPN).
Central venous catheters (CVCs)
Central venous catheters (CVCs) are also called central venous access devices (CVADs), central catheters, or central lines. Most CVCs have a long, flexible tube that ends in or near the superior vena cava (SVC), a large vein that goes into the heart.
Not everyone getting cancer treatment will need a CVC, but there are times when they can be helpful. You might need a CVC if:
- You have fragile or hard-to-find veins.
- You will need frequent blood draws or infusions.
- Your treatment is expected to last for months or longer.
- Your veins have been damaged from treatment.
- You need a medicine that can be hard on the veins or can cause skin damage if it leaks outside a peripheral IV.
- You need lots of different medicines and treatments at once and each one needs an IV.
- You need total parenteral nutrition (TPN), a liquid nutrition given by IV.
- Your arms can’t be used for IVs.
There are several types of CVCs. You and your doctor will discuss which is best for you. The kinds of CVCs commonly used during cancer treatment are:
- Implanted ports
- PICCs
- Tunneled catheters
Implanted ports (also called a port, Mediport, or port-a-cath)
- Ports are placed under the skin. They are usually put in the upper chest or arm, but can sometimes go in the abdomen (belly) or groin depending on the patient’s anatomy or medical condition.
- The port is placed by a surgeon or radiologist during a short surgical procedure while the patient is under sedation or general anesthesia (you will be asleep).
- To use a port, a nurse or other health care provider will put a special needle through the skin and into the port. You might hear this called “accessing” your port. Sometimes, to reduce pain, a numbing cream is used on the skin covering the port before the needle is inserted.
- The port needle is connected to an IV line with treatments.
- After the infusion is complete, the port will be flushed with fluid, and the needle removed. The port itself lies under the skin, so when it isn’t being used, it looks like a small bump.
- After the port is placed and the incision heals - and while it isn’t being accessed - you can bathe, shower, and swim.
- Your port will be flushed before and after each use. If the port won’t be used for a while, you may need to have it flushed occasionally to keep the line working.
- Single and double ports are available. Single ports allow one infusion at a time. Double ports allow two infusions at the same time. Each port must be accessed with its own needle.
- Ports can stay in for months or years.
- When you don’t need the port anymore, you will have a short procedure to remove it.
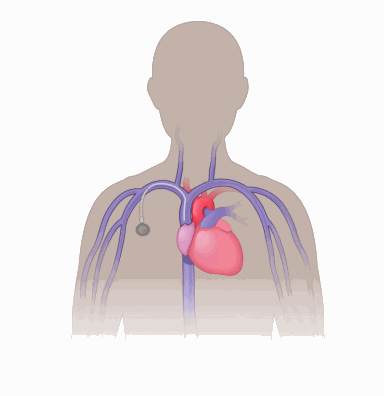
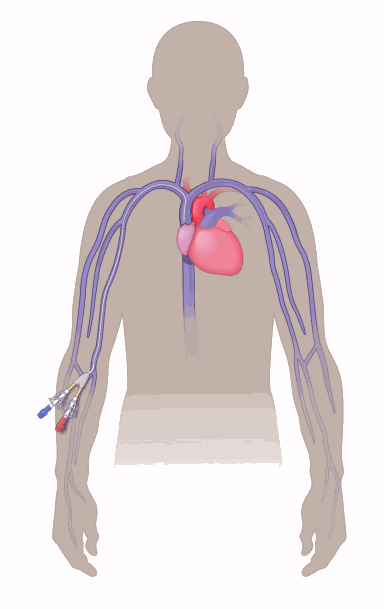
Peripherally inserted central catheters (PICCs)
- PICC lines (see image) are placed through the skin into a vein in the arm and passed along a vein that leads to the superior vena cava (SVC) near the heart.
- A PICC line is placed at the bedside by a specially trained nurse or health care provider. It does not require surgery.
- The end of the catheter sticks out of your arm through the skin and a clear dressing is placed over it. The IV tubing is attached to the end of the catheter.
- Since PICCs stick out of the skin, they cannot get wet. You will need to cover the PICC and dressing while bathing or showering.
- PICCs are flushed before and after each use. If it won’t be used for a while, you may need to have it flushed occasionally to keep it working.
- PICCs may have one to three lines, so that more than one infusion can be given at the same time, if needed.
- PICCs can be left in for days to months.
- When you don’t need the PICC anymore, it can be removed by a nurse or other health care provider.
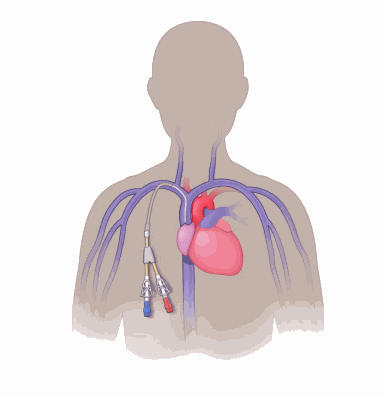
Tunneled CVCs (also called Hickman, Groshong, or Broviac catheters)
- Tunneled CVCs (see image) are placed through the skin into a vein in the chest or neck through a small incision (insertion site). They are tunneled under the skin, brought out through a separate incision (exit site), and stitched in place.
- The catheter is placed this way to lower the risk of infection. Having the catheter partly under the skin also lowers the risk it will accidentally be pulled out.
- Placing a tunneled CVC is done by a doctor, radiologist, or specially trained advanced practice provider (nurse practitioner or physician assistant/associate). Most often, they do not require surgery but can be placed in the operating room.
- The end of the catheter sticks out of your skin and a clear dressing is placed over it. This is attached to the IV tubing when used for treatment.
- Since tunneled CVCs stick out of the skin, they cannot get wet. You will need to cover the CVC and dressing while bathing or showering.
- Tunneled CVCs are flushed before and after each use. If it won’t be used for a while, you may need to have it flushed occasionally to keep it working.
- There are usually one to three lines, which allow for multiple infusions at once.
- Tunneled CVCs can be left in place for weeks to months.
- When you don’t need the CVC anymore, it can be removed by a nurse or other health care provider.
What are the benefits and risks of having a CVC?
If your cancer care team has suggested a CVC, ask them about the risks and benefits.
Benefits of having a CVC:
- You'll have fewer needle sticks. A peripheral IV must be taken out and a new one placed every few days, or sooner if the IV becomes displaced or irritated. CVCs can stay in place for weeks, months, or years depending on the type and how well it is taken care of.
- You can have several treatments at once. Some CVCs have multiple lines so that more than one infusion can be done at the same time. For example, you might have chemo going into one line, while IV fluids, antibiotics, or blood products go into another line at the same time.
- You have less risk of tissue damage. Since CVCs are longer in length, they are less likely to become displaced. Displaced IVs can leak fluids into the tissue and cause irritation or damage. CVCs also infuse into the large vein of the heart (SVC) that causes less irritation as compared to smaller veins.
- You can get treatment at home. Some people who have a CVC may be able to get fluids, medicines, or chemo at home instead of at the hospital or cancer center.
Risks of having a CVC:
- Pain. There may be some mild pain or discomfort during or after a CVC is placed. This usually goes away in a day or two.
- Bleeding. There may be some bleeding or bruising around the area where the CVC was placed. This is usually mild and goes away in few days.
- Infection. Having a CVC increases the risk of infection and requires special care (see below Caring for a central venous catheter).
- Blockage. Any type of IV catheter can become blocked by clotted blood. Your cancer care team will take steps to help prevent this from happening. If it does, medicines can be used to unblock it.
- Blood clots. Sometimes, a blood clot can form in the vein where the CVC is. It can cause redness or swelling in your hand, arm, shoulder, or neck.
- Migration or kinking. Sometimes, a CVC catheter can move, twist, or become kinked inside the vein and need to be repositioned.
- Accidental removal. Some CVCs can be accidentally pulled out. Your cancer care team will use tape or bandages to secure the CVC when it’s used for treatment. You will need to take special care to avoid tugging or pulling, when it is not in use.
- Collapsed lung. Very rarely, a lung can be punctured and collapse (pneumothorax) when a CVC is placed. Your doctor will take special steps to reduce the risk of this happening.
Caring for a central venous catheter
Your cancer care team will teach you or a caregiver how to take care of your CVC. Here are some things you can do:
- Clean your hands. Always wash your hands or use hand sanitizer before touching your CVC. Make sure anyone else touching your CVC cleans their hands first.
- Watch for signs of infection. Tell your cancer care team if you have fever, chills, or new redness, swelling, or oozing around the site of your CVC.
- Keep it dry. When you shower, cover and tape over your CVC with a waterproof material (like plastic wrap). If your dressing gets wet or loose, put a new dressing on. Moisture attracts bacteria, which can lead to infection.
- Keep it secure. Don’t pull on or bend your CVC tubing. If you use tape to secure it, don’t bend the tubing. Be careful around children and pets, or in situations where your CVC could be caught on something and pulled.
- Promote comfort. To reduce the discomfort of using a seatbelt while in a car, place a special cushion or pad over the CVCs site on your chest. This helps prevent pressure or rubbing from the seat belt, which can be painful. Ask your cancer care team where you can get one.
- Be prepared. Know what you need and keep enough supplies to care for your catheter. Have extra supplies on hand in case the dressing gets wet or comes off.
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
American Society of Clinical Oncology (ASCO). Catheters and ports in cancer treatment. Accessed at cancer.net. Content is no longer available.
Backler C, Kirmse JM. (Eds). Access device guidelines: Recommendations for nursing practice and education. 4th ed. Oncology Nursing Society; 2023.
Kehagias E, Galanakis N, Tsetis D. Central venous catheters: Which, when, and how. British Journal of Radiology. 2023; 96(1151), 20220894.
Kolikof J, Peterson K, Williams C, Baker AM. Central venous catheter insertion. Updated February 4, 2025. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. Accessed from https://www.ncbi.nlm.nih.gov/sites/books/NBK557798/on July 22, 2025.
Last Revised: July 22, 2025
Last Revised: July 22, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



