Your gift is 100% tax deductible.
Types of Ileostomies
The type of ileostomy you need will depend on why you are getting it.
You might need your ileostomy for weeks or months, or you might need it for the rest of your life.
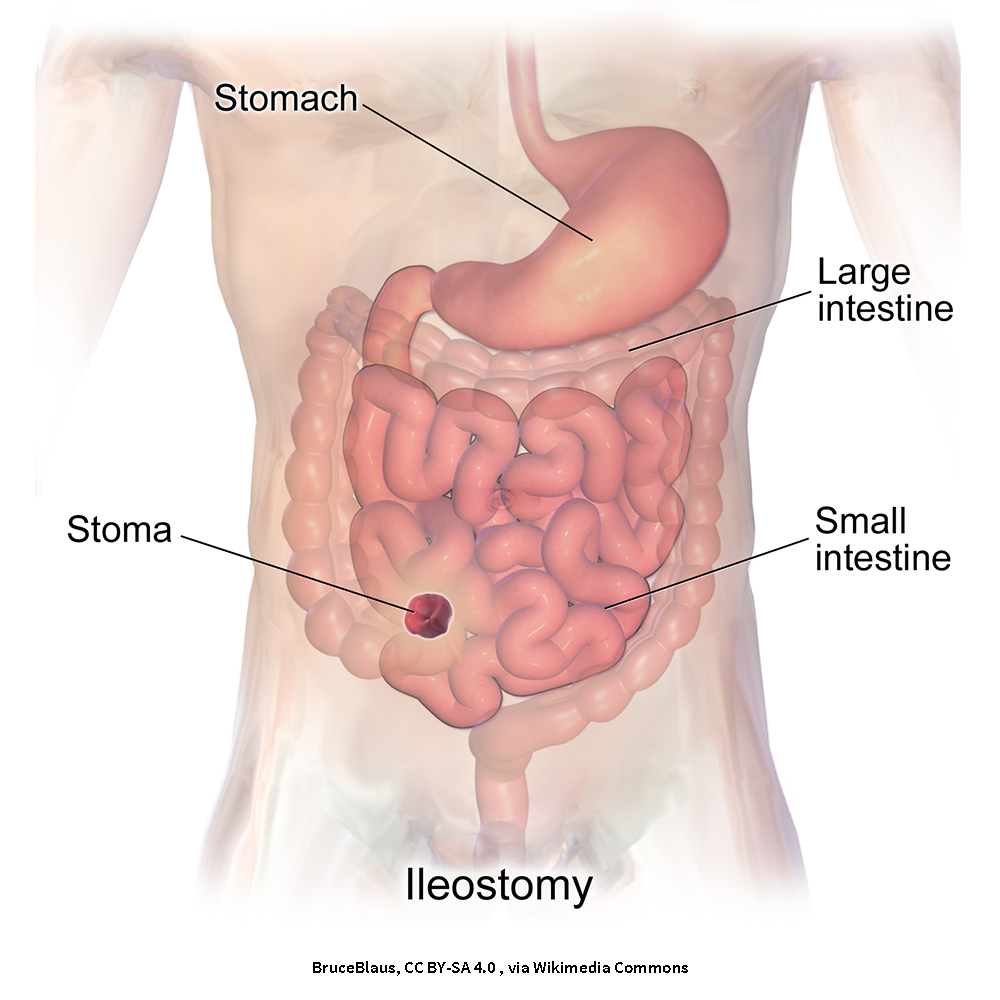
Temporary ileostomies
You might need a temporary ileostomy if your colon (large intestine) needs time to rest and heal after surgery. Since your bowel must be kept empty during this time, a temporary ileostomy is created.
Healing usually takes a few weeks or months but may take years. In time, the ileostomy will be surgically reversed (removed) and the bowel will work much like it did before.
A temporary ileostomy might also be done as the first stage in forming an ileo-anal reservoir (or J-pouch).
Permanent ileostomies
You might need a permanent Ileostomy if you have a disease like cancer and most or all of your colon needs to be removed. You will have this type of Ileostomy for the rest of your life.
How ileostomies are created
There are several types of ileostomies. You and your surgeon will talk about your options and together decide on the best surgery for you. Your options will depend on what part of your bowel has been affected by your disease, how long you will need the ostomy, your age, and your general health and preferences.
Ileostomies are most often placed on the right side of your abdomen.
Diverting loop ileostomy
A diverting loop ileostomy is most often temporary. For this type of ileostomy, a loop of small intestine is pulled through your abdomen to create a stoma . The loop is usually supported by a tube or rod until it heals.
A loop ileostomy may look like one large stoma, but it has 2 openings. One opening puts out stool, the other only puts out mucus. You won’t be able to control the output, so you’ll always need to wear a collection pouch and empty it regularly.
Having a loop ileostomy lets your bowel heal after surgery, or from a disease or injury. The two ends are often reconnected after several months and the ileostomy reversed so that you can move your bowels the same way you did before surgery.
Standard or end ileostomy
A standard ileostomy is the most common type and is usually permanent. The end of your small intestine is pulled through the right lower part of your abdomen and a stoma created on the skin of your belly.
You may need a standard ileostomy if most or all of your colon and rectum are removed because you have colorectal cancer or are at high risk because of familial adenomatous polyposis (FAP).
You always will need to wear a pouch to collect the stool that comes through the opening. Your stool will be liquid or paste-like and have digestive enzymes that can irritate the skin around your stoma.
Continent ileostomy
A continent ileostomy is a permanent ileostomy. It’s made by looping part of your ileum back on itself. This creates a reservoir or pocket inside your belly (abdomen) to hold your stool until you empty it. This pocket is connected to a stoma.
You will need to drain the stool from your ileostomy a few times a day by putting a thin, soft tube called a catheter into the stoma. Your stool will be liquid or paste-like and have digestive enzymes that can irritate the skin around your stoma.
You don’t need to wear an external pouch with this kind of ileostomy.
Ileo-anal reservoir (J-pouch or pelvic pouch)
If your entire colon is removed, you might need an ileo-anal reservoir. This is an internal pouch made from part of your small intestine which is connected to your anus to store stool. You may also hear this type of ileostomy called a J-pouch, W-pouch, or S-pouch, depending on the surgical procedure you get.
In most cases, at least 2 surgeries are needed to make the ileo-anal reservoir. After the first surgery, you would have a temporary ileostomy and attachment of a loop of small intestine to the rectum to create the pouch. Once the pouch is healed (about 3 months), the ileostomy is reversed, and you will begin having bowel movements as before surgery.
When you feel the need to move your bowels, your stool will pass through your anus and out of your body. The sphincter muscle around your anus will need to work to keep the pouch from leaking. The consistency of the stool that comes out of the pouch depends on what you eat and drink and can be managed with medicines.
This type of ileostomy is permanent. It is done most often to treat people at high risk of colorectal cancer because of familial adenomatous polyposis (FAP). It might also be done for people with ulcerative colitis.
What should I expect when my ileostomy is placed?
An ileostomy is created with surgery done when you are under general anesthesia. Your ileostomy may be done as an open surgery or laparoscopic surgery. Your surgeon can tell you which they think is best and why.
To help make sure that your stoma is put where you can see and care for it, your surgeon or a Wound Ostomy Continence nurse will figure out the best placement for your stoma. A WOC or ostomy nurse is a specially trained nurse who takes care of and teaches people to take care of their ostomies.
Like any surgery, having an ileostomy placed can cause side effects. You will be at risk of bleeding in your colon or stoma, infection, and damage to nearby organs.
You will likely need to stay in the hospital for 2 to 7 days after your ileostomy is placed. How long you stay will depend on why you need the ileostomy and any side effects you’re having. You can usually go home once your ileostomy is working and you are ready to care for it.
Complete recovery from an ileostomy can take up to 3 months. During this time, you might need to be careful about what you eat and drink. Your surgical team or ostomy nurse should let you know what you can eat and drink, and what you need to avoid
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
American Society of Clinical Oncology. Ileostomy. Cancer.net. Content is no longer available.
Babakhanlou R, Larkin K, Hita AG, Stroh J, Yeung SC. Stoma-related complications and emergencies. Int J Emerg Med. 2022;15(1):17. Published 2022 May 9. doi:10.1186/s12245-022-00421-9
Carmel J, Colwell JC, Goldberg M. Wound, Ostomy, and Continence Nurses Society Core Curriculum: Ostomy Management. 2nd ed. Wolters Kluwer Health; 2022.
Cross HH. CE: Nursing Care for Patients After Ostomy Surgery. Am J Nurs. 2023;123(8):34-41. doi:10.1097/01.NAJ.0000947460.38199.fe
Francone TD. Overview of surgical ostomy for fecal diversion. UpToDate. 2023. Accessed at https://www.uptodate.com/contents/overview-of-surgical-ostomy-for-fecal-diversion on April 18, 2025.
Peery AF, Shaheen NJ, Cools KS, et al. Morbidity and mortality after surgery for nonmalignant colorectal polyps. Gastrointest Endosc. 2018;87(1):243-250.e2. doi:10.1016/j.gie.2017.03.1550
Rivet EB. Ostomy Management: A Model of Interdisciplinary Care. Surg Clin North Am. 2019;99(5):885-898. doi:10.1016/j.suc.2019.06.007
United Ostomy Association of America (UOAA). Living with an ileostomy. Accessed at https://www.ostomy.org/wp-content/uploads/2022/10/UOAA_Living_with_an_Ileostomy_Guide-2022-10.pdf on May 5, 2025.
Last Revised: July 1, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



