Your gift is 100% tax deductible.
Core Needle Biopsy of the Breast
If exams or imaging tests show you might have breast cancer, your doctor might refer you for a core needle biopsy (CNB) to help find out for sure. This is often the preferred type of biopsy if breast cancer is suspected, because it removes more breast tissue than a fine needle aspiration (FNA), but it doesn't require surgery.
During this procedure, the doctor uses a hollow needle to take out pieces of breast tissue from the area of concern. This can be done with the doctor either feeling the area or while using an imaging test to guide the needle.
What is a core needle biopsy?
For a CNB, the doctor uses a hollow needle to take out pieces of breast tissue from a suspicious area the doctor has felt on exam or has seen on an imaging test. The needle may be attached to a spring-loaded tool that moves the needle in and out of the tissue quickly, or it may be attached to a suction device that helps pull breast tissue into the needle (known as a vacuum-assisted core biopsy).
A small cylinder (core) of tissue is taken out in the needle. Several cores are often removed.
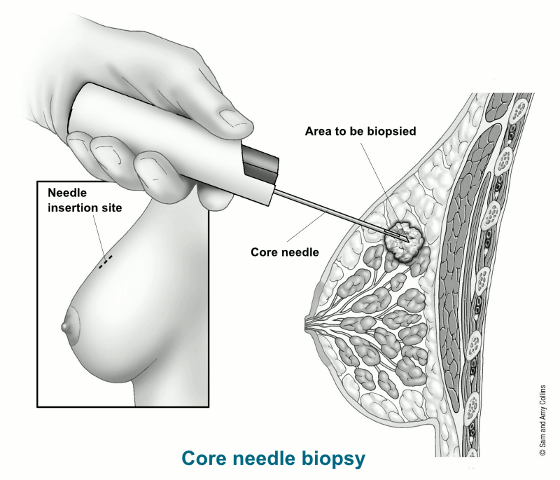
The doctor might put the needle into the abnormal area by feeling the lump. But usually some type of imaging test is used to guide the needle into the right place. Some of the imaging tests a doctor may use include:
- Mammogram (or breast tomosynthesis) (known as a stereotactic biopsy)
- Ultrasound
- MRI
The type of imaging test used to guide the biopsy depends on which test can best see the abnormal area, as well as which is most comfortable for the patient.
What should you expect if you have a CNB?
During the CNB
A CNB is most often done as an outpatient procedure, such as in a doctor’s office. The procedure itself is usually fairly quick, though it may take more time if imaging tests are needed or if one of the special types of CNB described below is used.
If your biopsy is done using image guidance, you may be sitting up, lying flat or on your side, or lying face down on a special table with openings for your breasts to fit into. This depends on which type of imaging (mammography, ultrasound, or MRI) is done. You will have to be still while the biopsy is done.
For any type of CNB, a thin needle will be used first to put numbing medicine (local anesthesia) into the area to be biopsied. Sometimes a small cut (about ¼ inch) is then made in the breast. The biopsy needle is put into the breast tissue through this cut to remove the tissue sample. You might feel pressure as the needle goes in. Again, an imaging test may be used to guide the needle to the right spot.
Typically, a tiny tissue marker (also called a clip) is put into the area where the biopsy is done. This marker will show up on mammograms or other imaging tests so the exact area can be located for further treatment (if needed) or follow up. You can’t feel or see the marker. It can stay in place and is safe during MRIs, and it will not set off metal detectors.
Once the tissue is removed, the needle is taken out. Stitches aren't usually needed, but pressure may be applied for a short time to help limit bleeding. The area is then covered with a sterile dressing.
For more on what it's like to have each type of CNB, see "Types of image-guided core needle biopsies" below.
After the CNB
You might be told to limit strenuous activity for a day or so, but you should be able to go back to your usual activities after that. Your doctor or nurse will give you instructions on this.
A CNB can cause some bleeding, bruising, or swelling. This can make it seem like the breast lump is larger after the biopsy. Most often, this is nothing to worry about, and any bruising or swelling will go away over time. Your doctor or nurse will tell you how to care for the biopsy site and when you might need to contact them if you’re having any issues. A CNB usually doesn’t leave a scar.
Types of image-guided core needle biopsies
There are 3 main types of image-guided biopsies:
- Stereotactic (mammogram- or tomosynthesis-guided)
- Ultrasound-guided
- MRI-guided
The type of image-guided biopsy that is best for you will depend on which type of imaging test will show the abnormal area best, as well as your comfort.
Stereotactic (mammogram- or tomosynthesis-guided) core needle biopsy
For this procedure, a doctor uses mammogram pictures taken from different angles to pinpoint the biopsy site. A computer analyzes the breast x-rays and shows where the needle tip needs to go in the abnormal area. This type of biopsy is often used to check suspicious microcalcifications (tiny calcium deposits) or small masses or other abnormal areas that can’t be seen clearly on an ultrasound.
You may be sitting up, lying on your side, or lying on your belly with your breast hanging through a hole in the table for this procedure.
The breast will be positioned in the mammography machine and compressed, and an image will be taken to make sure the area in question can still be seen. The breast is then cleaned, and numbing medicine (local anesthesia) is given. The biopsy device is placed into the breast, and more images are taken to confirm that the device is in the correct spot to take samples. Several biopsy samples are then taken.
Afterwards, the device is removed from the breast, and a biopsy marker (clip) is placed in the area. Another mammogram is then done to confirm the marker is in the right place.
Ultrasound-guided core needle biopsy
For this procedure, a doctor uses breast ultrasound to view the area that needs to be biopsied. Typically this is done while you are lying down or slightly on your side, with your arm above your head.
An ultrasound is done first to view the area. Then the skin is cleaned and numbing medicine (local anesthesia) is injected. Ultrasound is then used to guide the needle into the correct area. You might feel pressure as the needle goes in. Several biopsy samples are usually taken.
A biopsy marker (clip) is placed in the area of the biopsy. Most often, a mammogram is done after the biopsy to confirm the clip is in the right place.
MRI-guided core needle biopsy
For this procedure, a doctor uses breast MRI to locate and biopsy the suspicious area. This is most often done when something is seen on a breast MRI that is unlikely to be seen on mammogram or ultrasound. As with a breast MRI, you will be asked to lie on your belly on the MRI table with your arms above your head. However, the breast will be compressed during the procedure.
The table will slide into the MRI scanner and images will be taken. Then you’ll be given contrast through an IV line (which can help make the abnormal area easier to see), and more images will be taken.
Once the suspicious area has been located, the skin is cleaned and numbing medicine (local anesthesia) is injected into the area. The biopsy device is then gently inserted into the breast. It’s normal to feel pressure while this is being done.
More MRI images will then be taken to confirm to that the device is in the correct spot to take samples. Several biopsy samples are then taken, and the device is removed from the breast.
A biopsy marker (clip) is then placed in the area of the biopsy. Most often, a mammogram is done after the biopsy to confirm the clip is in the right place.
What does a CNB show?
A doctor called a pathologist will look at the biopsy tissue and/or fluid to check if there are cancer cells in it. A CNB is likely to clearly show if cancer is present (and often provides enough of a sample if other lab tests are needed), but it can still miss some cancers.
Ask your doctor when you can expect to get the results of your biopsy. If the results of the CNB do not give a clear diagnosis, or if your doctor still has concerns, you might need to have a second CNB or a more extensive type of biopsy, such as a surgical (open) biopsy.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
Joe BN, Esserman LJ. Breast Biopsy. 2021. UpToDate. Accessed at www.uptodate.com/contents/breast-biopsy on October 14, 2021.
Radiological Society of North America. Stereotactic Breast Biopsy. 2021. Accessed at https://www.radiologyinfo.org/en/info/breastbixr on October 14, 2021.
Radiological Society of North America. Ultrasound-Guided Breast Biopsy. 2021. Accessed at https://www.radiologyinfo.org/en/info/breastbius on October 14, 2021.
Sung JS, Comstock CE. Chapter 15: Image-Guided Biopsy of Nonpalpable Breast Lesions. In: Harris JR, Lippman ME, Morrow M, Osborne CK, eds. Diseases of the Breast. 5th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2014.
Last Revised: January 14, 2022
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



