Mammogram Basics
A mammogram is a low-dose x-ray that allows a special type of doctor (called a radiologist) to look for changes in breast tissue. Mammograms are used to look for breast cancer.
Why do I need mammograms?
Mammograms are used as a screening test in women without symptoms. They are also used for women who have symptoms that might be from cancer.
A mammogram can often find or detect breast cancer early, when it’s still small. Sometimes a mammogram can find breast cancer even before you feel a lump. When breast cancer is found early, it is usually easier to treat.
What are the main uses of mammograms?
Mammograms are used in two main ways.
Screening mammograms
A screening mammogram is used to look for signs of breast cancer in women who don’t have any breast symptoms or problems. X-ray pictures of each breast are taken, typically from 2 different angles.
Diagnostic mammograms
Mammograms are used to look at a woman’s breast if she has breast symptoms or if something unusual is seen on a screening mammogram. When used in this way, they are called diagnostic mammograms. They may include extra views (images) of the breast that aren’t part of screening mammograms. Sometimes diagnostic mammograms are used to screen women who were treated for breast cancer in the past.
What do mammograms show?
Mammograms can often show abnormal areas in the breast. They can’t tell for sure if an abnormal area is cancer, but they can help health care providers decide if more testing (such as a breast biopsy) is needed. The main types of breast changes found with a mammogram are:
- Calcifications
- Masses
- Asymmetries
- Distortions
Learn more about these and other breast changes in What Does the Doctor Look for on a Mammogram?
How do mammograms work?
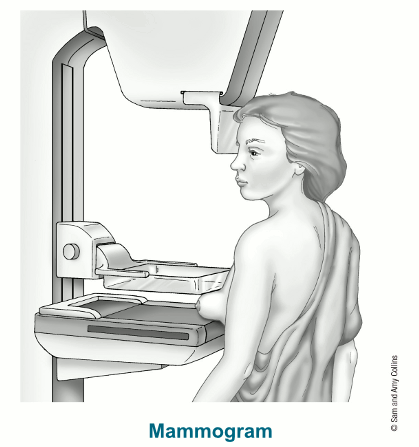
Mammograms are done with a machine designed to look only at breast tissue. The machine takes x-rays at lower doses than the x-rays done to look at other parts of the body, like the lungs or bones. The mammogram machine has 2 plates that compress or flatten the breast to spread the tissue apart. This gives a better quality picture and allows less radiation to be used.
To learn more about how they are done, see Tips for Getting a Mammogram.
In the past, mammograms were typically printed on large sheets of film. Today, digital mammograms are much more common. Digital images are recorded and saved as files in a computer.
What are three-dimensional (3D) mammograms?
Three-dimensional (3D) mammography is also known as breast tomosynthesis or digital breast tomosynthesis (DBT). As with a standard (2D) mammogram, each breast is compressed from two different angles (once from top to bottom and once from side to side) while x-rays are taken. But for a 3D mammogram, the machine takes many low-dose x-rays as it moves in a small arc around the breast. A computer then puts the images together into a series of thin slices. This allows doctors to see the breast tissues more clearly in three dimensions. (A standard two-dimensional [2D] mammogram can be taken at the same time, or it can be reconstructed from the 3D mammogram images.)
Many studies have found that 3D mammography appears to lower the chance of being called back for follow-up testing after screening. It also appears to find more breast cancers, and several studies have shown it can be helpful in women with dense breasts. A large study is now in progress to better compare outcomes between 3D mammograms and standard (2D) mammograms.
For more on 3D mammograms, see American Cancer Society Recommendations for the Early Detection of Breast Cancer.
Are mammograms safe?
Mammograms expose the breasts to small amounts of radiation. But the benefits of mammography outweigh any possible harm from the radiation exposure. Modern machines use low radiation doses to get breast x-rays that are high in image quality. On average the total dose for a typical mammogram with 2 views of each breast is about 0.4 millisieverts, or mSv. (A mSv is a measure of radiation dose.) The radiation dose from 3D mammograms can range from slightly lower to slightly higher than that from standard 2D mammograms.
To put these doses into perspective, people in the US are normally exposed to an average of about 3 mSv of radiation each year just from their natural surroundings. (This is called background radiation.) The dose of radiation used for a screening mammogram of both breasts is about the same amount of radiation a woman would get from her natural surroundings over about 7 weeks.
If there’s any chance you might be pregnant, let your health care provider and x-ray technologist know. Although the risk to the fetus is very small, and mammograms are generally thought to be safe during pregnancy, screening mammograms aren’t routinely done in pregnant women who aren't at increased risk for breast cancer.
Mammograms might also result in some women getting additional tests that don't result in a breast cancer diagnosis, but that might still have their own harms. For more on this, see Limitations of Mammograms.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
Bahl M, Pinnamaneni N, Mercaldo S, et al. Digital 2D versus tomosynthesis screening mammography among women aged 65 and older in the United States. Radiology. 2019; 291:582-590.
Helvie MA, Patterson SK. Chapter 11: Imaging Analysis: Mammography. In: Harris JR, Lippman ME, Morrow M, Osborne CK, eds. Diseases of the Breast. 5th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2014.
Hendrick RE. Radiation doses and cancer risks from breast imaging studies. Radiology. 2010;257(1):246-253.
Lowry KP, Coley RY, Miglioretti DL, et al. Screening performance of digital breast tomosynthesis vs digital mammography in community practice by patient age, screening round, and breast density. JAMA Netw Open. 2020;3(7):e2011792.
Oeffinger KC, Fontham ET, Etzioni R, et al. Breast cancer screening for women at average risk: 2015 guideline update from the American Cancer Society. JAMA. 2015;314(15):1599-614.
Puliti D, Duffey SW, Miccinesi G, et al. Overdiagnosis in mammographic screening for breast cancer in Europe: A literature review. J Med Screen, 2012;19:Suppl 1:42-56.
Radiological Society of North America (RSNA). Breast Tomosynthesis. 2020. Accessed at https://www.radiologyinfo.org/en/info/tomosynthesis on September 28, 2021.
Radiological Society of North America (RSNA). Radiation Dose in X-Ray and CT Exams. 2019. Accessed at https://www.radiologyinfo.org/en/info/safety-xray on September 28, 2021.
Rose SL, Tidwell AL, Bujnoch LJ, et al. Implementation of breast tomosynthesis in a routine screening practice: An observational study. AJR Am J Roentgenol. 2013;200(6):1401-1408.
Skaane P, Bandos AI, Gullien R, et al. Comparison of digital mammography alone and digital mammography plus tomosynthesis in a population-based screening program. Radiology. 2013;267(1):47-56.
Svahn TM, Houssami N, Sechopoulos I, Mattsson S. Review of radiation dose estimates in digital breast tomosynthesis relative to those in two-view full-field digital mammography. Breast. 2015;24(2):93-99.
Last Revised: January 14, 2022
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.


