Your gift is 100% tax deductible.
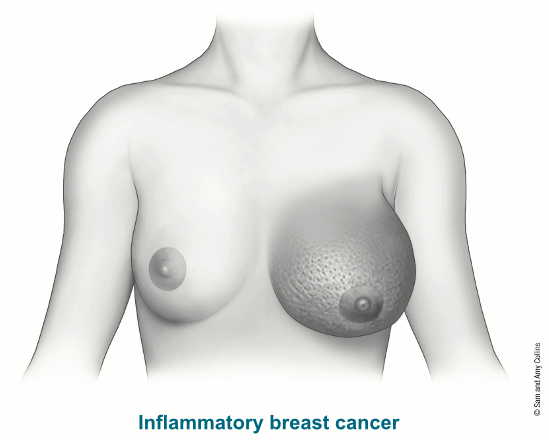
Inflammatory Breast Cancer
Inflammatory breast cancer (IBC) is a rare and aggressive type of invasive breast cancer in which cancer cells block lymph vessels in the skin. This causes the breast to look “inflamed.”
What is inflammatory breast cancer?
Inflammatory breast cancer (IBC) is rare. It accounts for only 1% to 5% of all breast cancers. Although it is a type of invasive ductal carcinoma, its symptoms, outlook, and treatment are different. IBC causes symptoms of breast inflammation like swelling and redness, which is caused by cancer cells blocking lymph vessels in the skin causing the breast to look "inflamed."
Inflammatory breast cancer (IBC) differs from other types of breast cancer in many ways:
- IBC doesn't look like a typical breast cancer. It often does not cause a breast lump, and it might not show up on a mammogram. This makes it harder to diagnose.
- IBC tends to occur in younger women (younger than 40 years of age).
- Black women appear to develop IBC more often than White women.
- IBC is more common among women who have excess body weight (overweight or obesity).
- IBC tends to be more aggressive—it grows and spreads much more quickly—than more common types of breast cancer.
- IBC is always at least at a locally advanced stage when it’s first diagnosed because the breast cancer cells have grown into the skin. (This means it is at least stage III.)
- In about 1 of 3 cases, IBC has already spread (metastasized) to distant parts of the body when it is diagnosed. This makes it harder to treat successfully.
- Women with IBC tend to have a worse prognosis (outcome) than women with other common types of breast cancer.
Signs and symptoms of inflammatory breast cancer
Inflammatory breast cancer (IBC) can cause a number of signs and symptoms, most of which develop quickly (within 3 to 6 months), including:
- Swelling (edema) of the skin of the breast
- Redness involving more than one-third of the breast
- Pitting or thickening of the skin of the breast so that it may look and feel like an orange peel
- A retracted or inverted nipple
- One breast looking larger than the other because of swelling
- One breast feeling warmer and heavier than the other
- A breast that may be tender, painful, or itchy
- Swelling of the lymph nodes under the arms or near the collarbone
If you have any of these symptoms, it does not mean that you have IBC, but you should see a doctor right away. Tenderness, redness, warmth, and itching are also common symptoms of a breast infection or inflammation, such as mastitis if you’re pregnant or breastfeeding. Because these problems are much more common than IBC, your doctor might suspect infection at first as a cause and treat you with antibiotics.
Treatment with antibiotics may be a good first step, but if your symptoms don’t get better in 7 to 10 days, more tests need to be done to look for cancer. Let your doctor know if it doesn't help, especially if the symptoms get worse or the affected area gets larger. The possibility of IBC should be considered more strongly if you have these symptoms and are not pregnant or breastfeeding, or have been through menopause. Ask to see a specialist (like a breast surgeon) if you’re concerned.
IBC grows and spreads quickly, so the cancer may have already spread to nearby lymph nodes by the time symptoms are noticed. This spread can cause swollen lymph nodes under your arm or above your collar bone. If the diagnosis is delayed, the cancer can spread to distant sites.
How is inflammatory breast cancer diagnosed?
Imaging tests
If inflammatory breast cancer (IBC) is suspected, one or more of the following imaging tests may be done:
Often a photo of the breast is taken to help record the amount of redness and swelling before starting treatment.
Biopsy
Inflammatory breast cancer is diagnosed by a biopsy, taking out a small piece of the breast tissue and looking at it in the lab. This might mean a punch biopsy of the breast skin that is abnormal. Your physical exam and other tests may show findings that are "suspicious for" IBC, but only a biopsy can tell for sure that it is cancer.
Tests on biopsy samples
The cancer cells in the biopsy will be examined in the lab to determine their grade.
They will also be tested for certain proteins that help decide which treatments will be helpful. Women whose breast cancer cells have hormone receptors are likely to benefit from treatment with hormone therapy drugs.
Cancer cells that make too much of a protein called HER2 or too many copies of the gene for that protein may be treated by certain drugs that target HER2.
In certain cases, other gene mutations (changes) or proteins might be tested for to see if specific drugs might be helpful.
Stages of inflammatory breast cancer
All inflammatory breast cancers start as stage III (T4dNXM0) since they involve the skin. If the cancer has spread outside the breast to distant parts of the body, it is stage IV.
For more information, read about breast cancer staging.
Survival rates for inflammatory breast cancer
Inflammatory breast cancer (IBC) tends to grow quickly, is more likely to have spread at the time it’s found, and is more likely to come back after treatment than most other types of breast cancer. Because of this, the survival rates are generally not as high as they are for other types of breast cancer.
Survival rates can give you an idea of what percentage of people with the same type and stage of cancer are still alive a certain amount of time (usually 5 years) after they were diagnosed. They can’t tell you how long you will live, but they may help give you a better understanding of how likely it is that your treatment will be successful.
Keep in mind that survival rates are estimates and are often based on previous outcomes of large numbers of people who had a specific cancer, but they can’t predict what will happen in any particular person’s case. These statistics can be confusing and may lead you to have more questions. Ask your doctor how these numbers may apply to you, as they are familiar with your situation.
What is a 5-year relative survival rate?
A relative survival rate compares women with the same type and stage of breast cancer to women in the overall population. For example, if the 5-year relative survival rate for a specific stage of breast cancer is 70%, it means that women who have that cancer are, on average, about 70% as likely as women who don’t have that cancer to live for at least 5 years after being diagnosed.
Where do these numbers come from?
The American Cancer Society relies on information from the Surveillance, Epidemiology, and End Results (SEER) database, maintained by the National Cancer Institute (NCI), to provide survival statistics for different types of cancer.
The SEER database tracks 5-year relative survival rates for breast cancer in the United States, based on how far the cancer has spread. The SEER database, however, does not group cancers by AJCC TNM stages (stage 1, stage 2, stage 3, etc.). Instead, it groups cancers into localized, regional, and distant stages:
- Localized: There is no sign that the cancer has spread outside of the breast.
- Regional: The cancer has spread outside the breast to nearby structures or lymph nodes.
- Distant: The cancer has spread to distant parts of the body such as the lungs, liver, or bones.
5-year relative survival rates for inflammatory breast cancer
These numbers are based on women diagnosed with IBC between 2015 and 2021.
(There is no localized SEER stage for IBC since it has already reached the skin when first diagnosed.)
| SEER Stage | 5-year Relative Survival Rate |
| Regional | 53% |
| Distant | 22% |
| All SEER Stages | 40% |
Understanding the numbers
- Women now being diagnosed with inflammatory breast cancer may have a better outlook than these numbers show. Treatments improve over time, and these numbers are based on women who were diagnosed and treated at least 5 years earlier.
- These numbers apply only to the stage of the cancer when it is first diagnosed. They do not apply later on if the cancer grows, spreads, or comes back after treatment.
- These numbers don’t take everything into account. Survival rates are grouped based on how far the cancer has spread, but your age and overall health, how well the cancer responds to treatment, tumor grade, and other factors can also affect your outlook.
Treating inflammatory breast cancer
Inflammatory breast cancer (IBC) that has not spread outside the breast is stage III. In most cases, treatment is chemotherapy first to try to shrink the tumor, followed by surgery to remove the cancer. Radiation and often other treatments, like more chemotherapy or targeted drug therapy, are given after surgery. Because IBC is so aggressive, breast conserving surgery (lumpectomy) and sentinel lymph node biopsy are typically not part of the treatment.
IBC that has spread to other parts of the body (stage IV) may be treated with chemotherapy, hormone therapy, and/or targeted drugs.
For details, see Treatment of Inflammatory Breast Cancer.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
American Joint Committee on Cancer. Breast. In: AJCC Cancer Staging Manual. 8th ed. New York, NY: Springer; 2017:589.
Curigliano G. Inflammatory breast cancer and chest wall disease: The oncologist perspective. Eur J Surg Oncol. 2018 Aug;44(8):1142-1147.
Hennessy BT, Gonzalez-Angulo AM, Hortobagyi GN, et al. Disease-free and overall survival after pathologic complete disease remission of cytologically proven inflammatory breast carcinoma axillary lymph node metastases after primary systemic chemotherapy. Cancer. 2006;106:1000−1006.
Henry NL, Shah PD, Haider I, Freer PE, Jagsi R, Sabel MS. Chapter 88: Cancer of the Breast. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa: Elsevier; 2020.
Howlader N, Noone AM, Krapcho M, Miller D, Brest A, Yu M, Ruhl J, Tatalovich Z, Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (eds). SEER Cancer Statistics Review, 1975-2017, National Cancer Institute. Bethesda, MD, https://seer.cancer.gov/csr/1975_2017/, based on November 2019 SEER data submission, posted to the SEER web site, April 2020.
Jagsi R, King TA, Lehman C, Morrow M, Harris JR, Burstein HJ. Chapter 79: Malignant Tumors of the Breast. In: DeVita VT, Lawrence TS, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 11th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2019.
Menta A, Fouad TM, Lucci A, Le-Petross H, Stauder MC, Woodward WA, Ueno NT, Lim B. Inflammatory Breast Cancer: What to Know About This Unique, Aggressive Breast Cancer. Surg Clin North Am. 2018 Aug;98(4):787-800.
National Cancer Institute. Inflammatory Breast Cancer. 2016. Accessed at https://www.cancer.gov/types/breast/ibc-fact-sheet on August 30, 2021.
National Comprehensive Cancer Network (NCCN). Practice Guidelines in Oncology: Breast Cancer. Version 7.2021. Accessed at https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf on August 30, 2021.
Overmeyer B and Pierce LJ. Chapter 59: Inflammatory Breast Cancer. In: Harris JR, Lippman ME, Morrow M, Osborne CK, eds. Diseases of the Breast. 5th ed. Philadelphia, Pa: Lippincott-Williams & Wilkins; 2014.
Schlichting JA, Soliman AS, Schairer C, Schottenfeld D, Merajver SD. Inflammatory and non-inflammatory breast cancer survival by socioeconomic position in the Surveillance, Epidemiology, and End Results database, 1990-2008. Breast Cancer Res Treat. 2012 Aug;134(3):1257-68. Epub 2012 Jun 26.
SEER*Explorer: An interactive website for SEER cancer statistics [Internet]. Surveillance Research Program, National Cancer Institute. Accessed at https://seer.cancer.gov/explorer/ on June 13, 2025.
Taghian A and Merajver SD. Inflammatory breast cancer: Clinical features and treatment. In Vora SR, ed. UpToDate. Waltham, Mass.: UpToDate, 2021. https://www.uptodate.com. Last updated November 25, 2020. Accessed August 24, 2021.
Yang WT, Le-Petross HT, Macapinlac H, Carkaci S, Gonzalez-Angulo AM, Dawood S, Resetkova E, Hortobagyi GN, Cristofanilli M: Inflammatory breast cancer: PET/CT, MRI, mammography and sonography findings. Breast Cancer Res Treat. 2008 Jun;109(3):417-26. Epub 2007 Jul 26. Review.
Last Revised: June 25, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



