Your gift is 100% tax deductible.
Managing Sexual Side Effects as a Woman with Cancer
Cancer treatment can cause physical and emotional changes that might affect your desire for sex. These changes might also make it harder to engage in your preferred sexual activity. But there are steps you can take to deal with these changes so that you can have a satisfying sex life.
- Talking with your cancer care team about sexual side effects
- Premature (early) menopause
- Pain during vaginal sex
- Vaginal dryness
- Vaginal narrowing
- Pelvic floor physical therapy to manage vaginal pain and narrowing
- Orgasm after cancer treatment
- Sexual desire (libido) after cancer and cancer treatment
- Specific cancers and treatments that can affect sexual desire
- Feeling good about yourself and feeling good about sex
- Making sex more comfortable
- Getting professional help
- Learn more
Talking with your cancer care team about sexual side effects
If you have concerns about sex or intimacy during or after cancer treatment, you might need to be the one to bring it up with your cancer care team or gynecologist.
Studies show that health professionals don’t always ask or talk about the sexual side effects certain cancer treatments can cause. Don’t assume your doctor or nurse will ask you about sex or intimacy problems. But these issues are still important, even if your health care team doesn’t bring them up.
Remember, if they don't know you have a problem, they can't help you manage it. If you aren’t getting the information you need, you can always ask for a referral to a specialist. The information below can help you start the conversation with your health care team.
The information below describes common sexual problems faced by adult women (or people with female reproductive organs*) after certain types of cancer treatment. You might have problems or needs that aren’t addressed here. Your cancer care team can help you manage your specific situation.
*To learn more about the gender terms used here, and how to start the conversation with your cancer care team about gender identity and sexual orientation, see Gender Identity, Sexual Orientation, and Cancer Treatment.
Premature (early) menopause
Certain types of cancer treatment can cause premature or early menopause.
Menopause happens when your ovaries stop making enough female hormones. This most often takes place when you are in your 50s. But some cancer treatments might make you go through menopause at a younger age.
Causes of premature menopause during cancer treatment
- Surgery: If you have your ovaries removed (oophorectomy) or have a total hysterectomy that includes removal of your ovaries, you will go into menopause that cannot be reversed.
- Radiation therapy, chemotherapy, and hormone therapy: These treatments can cause your ovaries to fail, leading to premature menopause. This menopause can be temporary; some women regain ovarian function after treatment ends. But for other women, this menopause is permanent.
Symptoms of premature menopause
Symptoms of premature menopause are the same as for natural menopause. These can include:
- Hot flashes or flushes: These can happen at any time during the day but can be especially bothersome at night. Hot flashes may be accompanied by chills, flushing (redness and warmth) on the face, anxiety, and feeling like your heart is racing. You can learn more about hot flashes and how to manage them in Hot Flashes.
- Lower sexual desire: This can happen because of lower hormone levels, stress, or poor sleep.
- Vaginal changes: Lower hormone levels can cause vaginal dryness and thinning of vaginal tissues. These changes can make vaginal sex uncomfortable and even painful.
Treatment of premature menopause
Female hormones (estrogen and/or progesterone) are sometimes used to help manage menopause symptoms. This is called menopausal hormone therapy. It comes in the form of a pill, patch, or less often, a vaginal ring.
Some women with cancer might not be able to take these hormones.
If you have breast, endometrial, or ovarian cancer, your doctor may advise against hormone therapy. That is because hormones might promote the growth of these types of cancer. If you can’t take hormone therapy, there may be other treatments to help you manage your symptoms.
If you have questions or concerns about hormone therapy, talk with your cancer care team. If you and your team decide menopausal hormone therapy is the best treatment for you, be sure you understand what to watch for while you take it. It’s important that you have regular checkups so that your dose can be changed if needed.
Pain during vaginal sex
If you have dryness, narrowing, or other changes in your vagina, you might have pain during sex. This is called dyspareunia. You might feel pain in your vagina itself or in the tissues around it, like your bladder and rectum.
Causes of pain during vaginal sex
The most common cause of pain during sex is vaginal dryness or narrowing from cancer treatment. The walls of your vagina might also get thinner and less stretchy.
If your cancer treatment includes hormone therapy or radiation to the pelvis, or if you’ve gone through premature menopause, your body might not create enough natural lubricant or moisture to make your vagina slippery. This can cause irritation or pain during sex. You might also be more likely to get bladder infections.
If you have pelvic surgery or radiation to your pelvis, your vagina might become shorter and narrower. This can also make sex painful or awkward.
Managing pain during sex
Having sex might take some planning. These tips may help lessen your pain and make sex more enjoyable.
If you have pain in or around your genitals during sex
- Tell your health care team. Tell your cancer care team or gynecologist about the pain. Don’t let embarrassment keep you from getting medical care.
- Spend extra time on foreplay. The pain might not be as bad if you feel very aroused before you start vaginal sex. Your vagina expands to its fullest length and width only when you are highly excited. This is also when the walls of the vagina produce lubricating fluid. It may take a longer time and more touching to get fully aroused.
- Use water-based lubricating gel. This can be used in and around your vagina before vaginal penetration. You can also use lubrication suppositories (soft gel pellets) that melt during foreplay.
- Let your partner know if any types of touching cause pain. Show your partner ways to caress you or positions that don’t hurt. Usually, light touching around the clitoris and the entrance to the vagina won’t hurt, especially if the area is well-lubricated.
- Try different sexual positions. For vaginal sex, try a position that lets you control the movement. Then, if deep penetration hurts, you can make the thrusts less deep. You can also control the speed.
If you have pain in other parts of your body
- Plan ahead. Talk with your partner about when you want to have sex. This will give you some time to prepare mentally and physically.
- Take any pain medicines ahead of time. If you use medicine to manage your pain, take it an hour or so before having sex so it will be working when you’re ready.
- Try different sexual positions. Find a position that puts as little pressure as possible on the sore areas of your body. If it helps, support the sore area and limit its movement with pillows. If a certain motion is painful, choose a position that doesn’t require it or ask your partner to take over the movements during sex.
- Talk with your partner. Tell your partner what you would like and what makes you most comfortable.
- Focus on your feelings of pleasure and excitement. This might help your pain to fade into the background.
Vaginal dryness
Vaginal dryness can be caused by premature (or regular) menopause or by treatments that affect your pelvic organs. There are hormonal and non-hormonal treatments that might help you manage this dryness.
Managing vaginal dryness with lubricants
If you have dryness, vaginal lubricants can help make sex more comfortable. There are several different options, including water-based, silicone, and oil-based lubricants. Place them in and around your vagina before vaginal penetration. You can also use lubrication suppositories (soft gel pellets) that melt during foreplay.
You can find lubricants near the birth control or feminine hygiene products in pharmacies or grocery stores. Be sure to read the labels, and talk with a nurse, doctor, or pharmacist if you have questions.
- Choose a water-based or silicone gel that has no perfumes, coloring, spermicide, herbal remedies, or flavors. These additions can irritate your genital tissues.
- Petroleum jelly, skin lotions, and other oil-based lubricants are not good choices for vaginal lubrication. These products can cause yeast infections or other vaginal problems.
- If you and your partner use latex condoms, stay away from oil-based lubricants as they can damage the latex. Stick with water- or silicone-based products.
- You might want to avoid using condoms or gels that contain nonoxynol-9 (N-9). N-9 is a birth control agent that kills sperm, but it can irritate the vagina and worsen pain.
Managing dryness with vaginal moisturizers
Many women with cancer who have vaginal dryness use vaginal moisturizers several times per week. Vaginal moisturizers help keep your vagina and vulva moist and more comfortable. For the best absorption, apply these at bedtime.
Vaginal moisturizers do not replace lubricants for sexual activity because they do not make your vagina slippery enough to ease penetration.
Managing dryness with vaginal estrogens
Vaginal estrogen therapy is sometimes used to treat vaginal dryness, narrowing, and atrophy (when the vaginal walls get thinner and less stretchy).
Vaginal hormones are applied to the genital area. They come in gel, cream, suppository, ring, and tablet forms. Most are put into the vagina, although some creams can be applied to your vulva (the outer part of your vagina).
Vaginal hormones provide small amounts of hormones to your vagina and nearby tissues. Studies show that very little of these hormones get into the bloodstream, so they should have little effect on other parts of your body.
However, if you have concerns about taking vaginal hormones, be sure to talk to your cancer care team. Ask them why they think vaginal hormones are a safe option for you. You can also ask about other treatment options that don’t include hormones.
Vaginal narrowing
Radiation to your pelvis can damage the walls of the vagina, leaving them scarred and less flexible. This can cause your vagina to get narrower and shorter. Some types of surgery can also cause changes in the length and width of your vagina.
Changes like these to your vagina can make sex and internal exams painful or even impossible. Using dilators and having pelvic physical therapy might help deal with these problems.
Managing narrowing with vaginal dilators
Vaginal dilators help keep your vagina open and more flexible after cancer treatment. If you have had radiation or surgery to your pelvis, your doctor or cancer care team may encourage you to use dilators to prevent problems. Even if you aren’t interested in being sexually active, keeping your vagina normal in size allows more comfortable gynecologic exams.
Vaginal dilators come in various widths. You can increase the dilator size as your vagina is able to stretch more. Vibrators can also be used as vaginal dilators and may improve blood flow.
Dilators can also help you learn to relax your vaginal muscles if they are used with Kegel exercises. These exercises help teach you how to control your pelvic floor and vaginal muscles.
Your doctor or nurse will tell you where to buy a dilator. Check with your insurance company to find out if you need a prescription.
You will also be taught when to start using it, and how and when to use it. The dilator feels much like putting in a large tampon for a few minutes. It can be used several times a week to keep your vagina from getting tight from scar tissue that may develop.
Pelvic floor physical therapy to manage vaginal pain and narrowing
Pelvic floor physical therapy teaches you how to relax your vaginal muscles so that you have less pain during sex. It is also sometimes used as part of treatment for vaginal narrowing.
If you’ve had pain during sex, you may tense the muscles inside your vagina without knowing it. This makes vaginal penetration even more painful. You might even clench your muscles so tightly that your partner cannot enter your vagina.
You can become aware of your vaginal muscles and learn to relax them during vaginal penetration. Exercises that teach control of the pelvic floor and vaginal muscles are called Kegels.
Ask your cancer care team or gynecologist to refer you to a therapist for pelvic physical therapy or pelvic rehabilitation.
Orgasm after cancer treatment
Some women report trouble having an orgasm during or after cancer treatment. There are some things you can try that might help.
- Focus on a sexual fantasy before or during sex. A fantasy can be a memory of a past experience or a daydream about something you’ve never tried. A strong sexual thought can help get you aroused and distract you from negative thoughts and fears.
- Use a hand-held vibrator for extra stimulation. Hold it yourself or ask your partner to caress your genitals with it. You can steer your partner to the areas that respond best and away from those that are tender or uncomfortable.
- If you have vaginal dryness, using a lubricant on your vulva and vagina can make touching more comfortable. If you are also using a silicone vibrator, stay away from silicone lubricants as they can damage the covering of the vibrator.
- Change the position of your legs during sexual activity. Some women reach orgasm more easily with their legs open and thigh muscles tense. Others prefer to press their thighs together.
- If you have intercourse, try different sexual positions. Positions where your clitoris gets more direct stimulation can help you reach orgasm.
- Tighten and relax your vaginal muscles in rhythm during intercourse or while your clitoris is being stroked. Or tighten and relax the muscles in time with your breathing. This helps you focus on what you’re feeling. Contract your vaginal muscles and pull them inward as you inhale and let them relax as you exhale.
- Ask your partner to gently touch your breasts and genital area at the same time or separately. Experiment with your partner to find the type of touch that most excites you.
If you continue to have trouble with orgasms, you might find sex therapy or counseling helpful. There are different techniques they can teach you. Ask your cancer care team or gynecologist for a referral.
Sexual desire (libido) after cancer and cancer treatment
Sexual desire can be affected by cancer and cancer treatment. If you are worried, depressed, nauseous (sick to your stomach), having pain, or experiencing fatigue, you may not feel like having sex. Cancer treatments that disturb the normal hormone balance in your body can also lessen your desire for sex.
Anyone going through cancer treatment might lose interest in sexual activity, at least for a time. You might not feel like it’s a priority while you are getting treated. But for most people, this is temporary.
Once you finish treatment and have recovered, your desire for sex and intimacy will most likely return. If you continue to have problems, think about seeing a therapist who has experience working with people with cancer.
Side effects that can lower your sexual desire
Some side effects of cancer and cancer treatment can lower your desire for sex while you have them.
Pain can make you feel worried, depressed, or easily discouraged. If you have these feelings, you may find it hard to get excited about sexual activity.
Other side effects from cancer and cancer treatment can also lower your desire for sex, including:
- Fatigue
- Nausea and vomiting
- Changes in how you look, such as rashes, hair loss, or an ostomy
Hormone therapy can affect desire
Cancer treatments that lower your hormone levels can reduce your desire for sex.
For example, treatment for some breast and endometrial cancers often includes hormone therapy to lower estrogen levels because estrogen can fuel the growth of these cancers.
The goal of hormone therapy is to starve the cancer cells of female hormones. This slows the growth of the cancer.
A decreased desire for sex (libido) is the most common sexual side effect of hormone treatment.
Hormone therapy may also cause physical changes, such as:
- Vaginal dryness
- Hot flashes
- Premature menopause
Ask your cancer care team about possible side effects and how to manage them.
Emotions can affect desire and intimacy
Your emotions about cancer and treatment can also affect your interest in sex and your ability to be intimate with your partner.
You might feel:
- Afraid the cancer will come back
- Sad, frustrated, or powerless
- Bad about changes in your body
- Stressed, depressed, or anxious
Your partner might also have many of the same emotions. Talk with each other about your feelings and concerns, including how they might affect your sexual desire and response. Keeping these feelings to yourself can get in the way of being intimate, both physically and emotionally.
If your emotions about cancer and cancer treatment are making it hard for you to be intimate, talk to your cancer care team or gynecologist. They will have resources to help you, or they can refer you to a counselor or sex therapist.
Specific cancers and treatments that can affect sexual desire
Any type of cancer or cancer treatment can affect your desire for sex, at least temporarily. But some cancers and treatments are more likely to cause significant or long-term changes to the way you experience sex and intimacy.
An ostomy is a surgical opening made to help with a body function. The opening itself is called a stoma.
- A urostomy takes urine through a new passage and sends it out through a stoma on your abdomen (belly).
- A colostomy or ileostomy gets rid of stool (poop) through an opening in your abdomen. In an ileostomy, the opening is made with the part of the small intestine called the ileum. A colostomy is made with a part of the large intestine called the colon.
Adjusting to sex and intimacy with an ostomy
There are ways to reduce the effect of an ostomy on your sex life.
- Make sure the appliance (pouch system) fits well.
- Check the seal and empty your pouch before sex. This will reduce the chance of a leak.
- To reduce rubbing against the appliance, choose sexual positions that keep your partner’s weight off the ostomy.
- Consider wearing a cotton cover made for ostomy pouches to decrease rubbing on you or your partner’s skin. Some people also like to wear intimate clothing that covers their pouch.
Learn more in Ostomies.
Surgery or radiation therapy for head and neck cancers can lead to changes in how you look and breathe. These changes may affect how you feel about being intimate with another person.
Appearance changes
Some cancers of the head and neck are treated by removing part of the bone structure of the face. This can change your appearance. Surgery on the jaw, mouth, or tongue can also change the way you look and talk. Facial reconstruction can help you regain a more normal look and clearer speech.
Laryngectomy and tracheostomy
Some people with head and neck cancer will need to have part of their airway removed.
- A laryngectomy is surgery that removes part or all of your voice box (larynx). A total laryngectomy (and some partial laryngectomies) leaves you unable to talk in the usual way. Since your larynx is next to the windpipe that connects your mouth and lungs, you might need a tracheostomy.
- A tracheostomy creates a new airway. Instead of breathing through your mouth and nose, you will breathe through a stoma (opening or hole) in the front of your neck. A tracheostomy might be created during laryngectomy surgery. It can be temporary or permanent.
Adjusting to sex and intimacy with a stoma
During sex, a partner may be startled at first by breath that hits at a strange spot. If you or your partner find this distracting, a scarf, necklace, or turtleneck can help hide the stoma cover.
If you are concerned about food odors coming from your stoma, it might help to avoid garlic or spicy foods and wear perfume.
Sometimes, problems speaking can make it hard to communicate during sex. If you learn to speak using your esophagus, this can make talking during sex less of an issue. A speech aid or electronic voice box built into the stoma might also work well.
Learn more in Ostomies.
Limb amputation
Treatment for some cancers can include surgically removing (amputating) a limb, such as an arm or leg.
If you’ve lost a limb, you may wonder whether to wear your artificial limb (prosthesis) during sex. Sometimes the prosthesis helps with positioning and ease of movement. Talk with your partner about what works best for the two of you.
Learn more in Prostheses.
Feeling good about yourself and feeling good about sex
Sometimes friends and partners withdraw when a person has cancer. This can be out of fear or uncertainty. It can help to talk with your partner about how each of you is feeling.
Sexual touching between you and your partner is always possible. It may just be different than before you got treated for cancer. It may be easy to forget this, especially if you’re both feeling down or have not had sex for a while.
Keep in mind that you might need extra help with the changes caused by cancer. Counseling and sex therapy may be good options.
Changes in the way you look
Cancer surgery and treatment can affect your appearance.
Your surgical scars may be visible. You might lose the hair on your head, or less often, your eyebrows, eyelashes, and pubic hair. If you have breast cancer, you may lose one or both breasts. You might gain or lose weight and muscle. You might have skin rashes or other changes to your skin and nails.
Changes you see or feel in your body might make you doubt that others will find you attractive. This might make you afraid to initiate or agree to sex.
- Talk about these changes with your partner or someone else close to you. This can help you realize how others see you, and in turn help you see yourself in a more positive light.
- Try asking your partner to tell you what they find enjoyable about the way you look or feel to the touch. Tell them that these positive responses will help you feel better about yourself.
- Let your partner know when you’re feeling unsure.
- Talk to your cancer care team about things that can be done to limit the damage cancer has on the way you look, your energy, and your sense of well-being.
You can find more tips on feeling good about yourself in Looking Your Best During Cancer Treatment.
Overcoming anxiety about sex
You might find it hard to be as spontaneous as you used to be. Try setting up time with your partner to relax, enjoy one another’s company, and talk about what you each would like sexually. Just as you learned to enjoy sex when you first started having it, you can learn how to feel pleasure again during and after cancer treatment.
Masturbation is not a required step in resuming your sex life, but it might help. It can help you find out where you are tender or sore and what kind of touch you enjoy. Sharing this information can help you and your partner decide what next steps to take.
Depending on your situation, you may feel a little shy bringing up sex. It might be hard to let your partner know you would like more physical closeness or that you’re anxious about having sex. But these conversations are an important step toward resuming a fulfilling sex life. So be as clear and direct as you can.
Making sex more comfortable
If you still have some pain or feel weak from cancer treatment, you might want to try new positions. Many couples have found one favorite position, particularly for vaginal penetration, and rarely try another. Talk to your partner and learn different ways to enjoy sex that are most comfortable. The drawings below are some ideas for positions that may help as you resume sex.
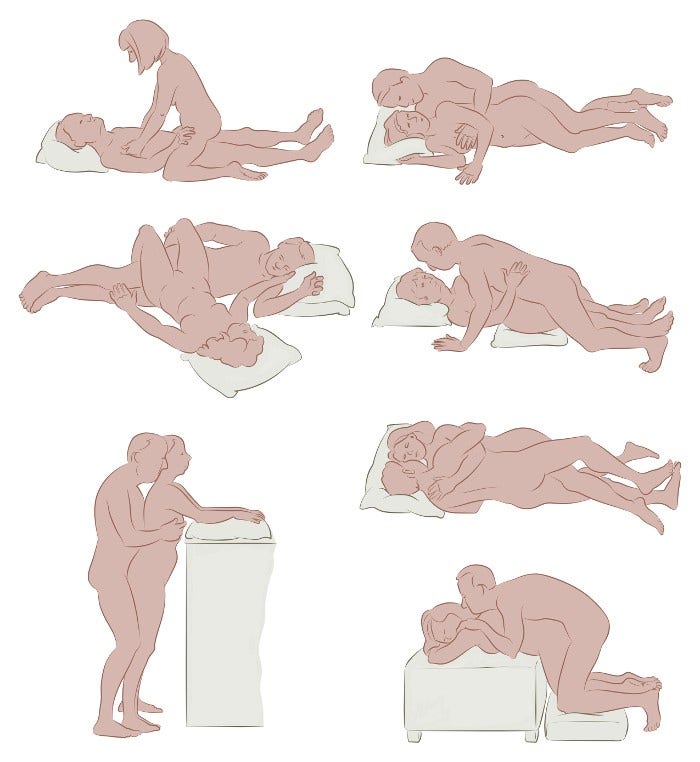
There's no one position that's right for everyone. You and your partner can work together to find what’s best for you. Pillows can help as supports. Keeping a sense of humor can always lighten the mood.
Getting professional help
Many health care professionals, including cancer doctors and nurses, have little training in sexuality issues. Depending on the problems you are having, you might be referred to a different kind of specialist.
A gynecologist is a medical doctor who specializes in female health issues, including sexual and reproductive function and diseases of the reproductive organs. They can see if you have any physical problems that are making sex difficult and suggest ways to deal with any sexual problems.
An endocrinologist is an expert in how hormones work in the body. If the most likely cause of a sexual problem is a hormone imbalance, an endocrinologist may be able to help.
There are many different programs and specialists that can help you find the answers you need. Ask your cancer care team or primary care provider for referrals to specialists who can help you.
Counseling and sex therapy
There are also health care professionals who can help you understand and manage the emotions that affect your sex life. Options include:
- Talking with a counselor or sex therapist.
- Finding help in your community, such as a support group for women who are cancer survivors.
- Seeing a couples counselor who can help you talk about tough issues with your partner, including emotions that interfere with intimacy and sex.
Sexual rehabilitation programs
Some cancer centers have experts on staff who can assess and treat sexual problems. Ask your cancer care team if your center offers any programs or where else you can get help.
Sex therapists and other types of counselors
Sex therapy is psychotherapy or counseling that focuses on solving a sexual problem.
Sex therapists may practice in a clinic or alone. Look for a sex therapist who is a licensed mental health professional (a psychiatrist, psychologist, social worker, or psychiatric clinical nurse specialist or nurse practitioner) with special training in treating sexual problems.
Psychotherapy can help you feel better about the changes in your body, help you and your partner communicate more clearly, and give you skills to better cope with your cancer and treatment. Couples counseling may be helpful, too.
Finding a well-qualified mental health professional is important. These are some of the different types of mental health professionals:
- Psychiatrist: A medical doctor (an MD or DO) with a specialty in psychiatry. They should also be certified by the American Board of Psychiatry and Neurology.
- Psychologist: Most psychologists who practice alone have a doctorate in psychology (PhD or PsyD) or in education (EdD). Psychologists do not have medical degrees and don’t write prescriptions. A psychologist with a master’s degree is usually supervised by someone with a doctorate. In most states, a psychologist must be licensed. Those who practice usually have degrees in clinical or counseling psychology.
- Social worker: A social worker usually has a master’s degree in social work (MSW). Many social workers have training in mental health counseling. Licensing laws vary from state to state.
- Marriage and family counselors: Some states have a category for licensed psychotherapists called marriage and family counselors. They usually have a master’s degree in psychology or a related field, plus training in counseling.
- Psychiatric clinical nurse specialists or psychiatric nurse practitioners: This is someone with a master’s or doctorate degree in psychiatric nursing. They are licensed professionally, although their ability to prescribe medicines varies from state to state.
Finding a sex therapist or counselor
Professional societies can often give you information about their members in your area who have special training in sex therapy. These are good places to start:
- American Association of Sex Educators, Counselors, and Therapists (AASECT)
www.aasect.org
- National Association of Social Workers (NASW)
www.helpstartshere.org
You can also get a listing of professionals in your area by contacting your state’s psychological association or a state association for licensed marriage and family therapists.
The cost of counseling varies with the professional’s level of training and experience. Insurance coverage for counseling varies depending on the health insurance plan. Check with your insurance company to find out if your plan will pay for counseling and how much of the cost it will cover.
Learn more
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
American Society of Clinical Oncology (ASCO). Interventions to Address Sexual Problems in People with Cancer: American Society of Clinical Oncology Clinical Practice Guideline Adaptation of Cancer Care Ontario Guideline. Published 2018. Accessed September 26th, 2024.
American Society of Clinical Oncology. Sexual Health and Cancer Treatment: Women. Cancer.net. Content is no longer available.
Bober SL & Krapf J. Overview of sexual dysfunction in female cancer survivors. UpToDate. 2024. Accessed September 26th, 2024. https://www.uptodate.com/contents/overview-of-sexual-dysfunction-in-female-cancer-survivors on February 20, 2025.
Carter et al. Interventions to address sexual problems in people with cancer: American Society of Clinical Oncology clinical practice guideline adaptation of Cancer Care Ontario guideline. Journal of Clinical Oncology. 2018;36(5):492-513.
Damast S, Jeffery DD, Son CH, et al. Literature Review of Vaginal Stenosis and Dilator Use in Radiation Oncology. Pract Radiat Oncol. 2019;9(6):479-491. doi:10.1016/j.prro.2019.07.001
Hickey M, Basu P, Sassarini J, et al. Managing menopause after cancer. Lancet. 2024;403(10430):984-996. doi:10.1016/S0140-6736(23)02802-7
Katz A. Breaking the Silence on Cancer and Sexuality: A Handbook for Healthcare Providers. 2nd ed. Pittsburgh, PA: Oncology Nursing Society.; 2018.
Lubián López DM. Management of genitourinary syndrome of menopause in breast cancer survivors: An update. World J Clin Oncol. 2022;13(2):71-100. doi:10.5306/wjco.v13.i2.71
National Comprehensive Cancer Network (NCCN). Clinical practice guidelines in oncology: Survivorship [Version 2.2019]. Accessed at https://www.nccn.org/professionals/physician_gls/pdf/survivorship.pdf on January 31, 2020 Shifren JL. Overview of sexual dysfunction in females: Epidemiology, risk factors, and evaluation. UpToDate. UpToDate, Inc; 2024. Updated May17, 2024. Accessed September 26th, 2024. https://www.uptodate.com/contents/overview-of-sexual-dysfunction-in-females-epidemiology-risk-factors-and-evaluation
Syrjala KL & Yi JC. Overview of psychosocial issues in the adult cancer survivor. UpToDate. UpToDate, Inc; 2024. Updated October 2023. Accessed September 26, 2024. https://www.uptodate.com/contents/overview-of-psychosocial-issues-in-the-adult-cancer-survivor
Last Revised: April 15, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



