Your gift is 100% tax deductible.
Mastectomy
Mastectomy is breast cancer surgery that removes the entire breast.
A mastectomy might be done:
- When a woman cannot be treated with breast-conserving surgery (lumpectomy), which saves most of the breast.
- If a woman chooses mastectomy over breast-conserving surgery for personal reasons.
- For women at very high risk of getting a second breast cancer who sometimes choose to have a double mastectomy (the removal of both breasts).
Types of mastectomies
There are several different types of mastectomies, based on how the surgery is done and how much tissue is removed.
Simple (or total) mastectomy
In this procedure, the surgeon removes the entire breast, including the nipple, areola, fascia (covering) of the pectoralis major muscle (main chest muscle), and skin. A few underarm lymph nodes might be removed as part of a sentinel lymph node biopsy depending on the situation. Most women, if they are hospitalized, can go home the next day.
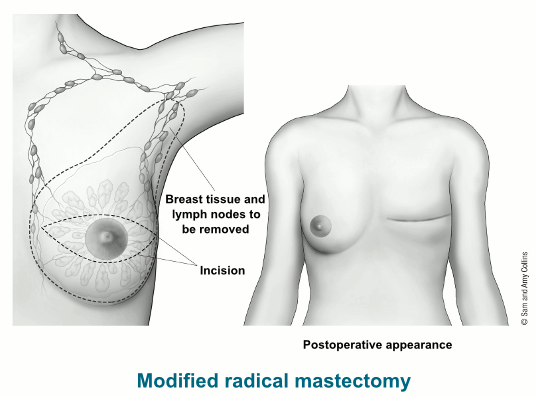
Modified radical mastectomy
A modified radical mastectomy combines a simple mastectomy with the removal of the lymph nodes under the arm (called an axillary lymph node dissection).
Radical mastectomy
This extensive surgery is rarely done now. The surgeon removes the entire breast, axillary (underarm) lymph nodes, and the pectoral (chest wall) muscles under the breast. This surgery was once very common, but less extensive surgery (such as the modified radical mastectomy) has been found to be just as effective and with fewer side effects. This operation might be done if the tumor is growing into the pectoral muscles.
Skin-sparing mastectomy
In this procedure, most of the skin over the breast is left place. Only the breast tissue, nipple, and areola are removed. The amount of breast tissue removed is the same as with a simple mastectomy. Implants or tissue from other parts of the body can be used during the surgery to reconstruct the breast.
Many women prefer a skin-sparing mastectomy because it offers the advantage of less scar tissue and a reconstructed breast that seems more natural. But it may not be suitable for larger tumors or those that are close to the surface of the skin.
The risk of local cancer recurrence with this type of mastectomy is the same as with other types of mastectomies.
Experts recommend that skin-sparing mastectomies be done by a team of breast surgeons with a lot of experience in this procedure.
Nipple-sparing mastectomy
A nipple-sparing mastectomy is similar to a skin-sparing mastectomy in that the breast tissue is removed and the breast skin is saved. But in this procedure, the nipple and areola are left in place. This can be followed by breast reconstruction. The surgeon often removes the breast tissue under the nipple and areola during the procedure to check for cancer cells. If cancer is found in this tissue, the nipple and areola must be removed.
This type of mastectomy is more often an option for women who have a small, early-stage cancer, away (more than 2cm) from the nipple and areola, with no signs of cancer in the skin or the nipple.
As with any surgery, there are risks. After the surgery, the nipple may not have a good blood supply, causing the tissue to shrink or become deformed. Because the nerves are also cut, there often may be little or no feeling left in the nipple. If a woman has larger breasts, the nipple may look out of place after the breast is reconstructed. As a result, many doctors feel that this surgery is best done in women with small to medium sized breasts. This procedure leaves fewer scars you can see, but it also has a risk of leaving behind more breast tissue than other forms of mastectomy. This could result in a higher risk of cancer developing than for a skin-sparing or simple mastectomy. However, improvements in technique have helped lower this risk and the risk of cancer coming back in the same area is about the same as with other types of mastectomies. Most experts consider nipple-sparing mastectomy to be an acceptable treatment for breast cancer in certain cases.
As with a skin-sparing mastectomy, experts also recommended that this type of mastectomy be done by a team of breast surgeons with a lot of experience with this procedure.
Double mastectomy
When both breasts are removed, it is called a double (or bilateral) mastectomy. Double mastectomy is sometimes done as a risk-reducing (or preventive) surgery for women at very high risk for getting breast cancer, such as those with a BRCA gene mutation. Most of these mastectomies are simple mastectomies, but some may be nipple-sparing. There are other situations where a double mastectomy might be done as part of a women's breast cancer treatment plan. This is done after careful consideration and discussion between the patient and their cancer care team.
Who might get a mastectomy?
Many women with early-stage cancers can choose between breast-conserving surgery (BCS) and mastectomy. You may prefer mastectomy as a way to "take out all the cancer as quickly as possible." But the fact is that in most cases, mastectomy does not give you any better chance of long-term survival compared to BCS. Studies of thousands of women over more than 20 years show that when BCS is done along with radiation, the outcome is the same as having a mastectomy.
Mastectomy might be recommended if you:
- Are unable to have radiation therapy
- Would prefer more extensive surgery instead of having radiation therapy
- Have had the breast treated with radiation therapy in the past
- Have already had BCS with re-excision(s) that did not completely remove the cancer
- Have two or more areas of cancer in different quadrants of the same breast (multicentric) that are not close enough to be removed together without changing the look of the breast too much
- Have a tumor larger than 5 cm (2 inches) across, or a tumor that is large relative to your breast size
- Are pregnant and would need radiation therapy while still pregnant (risking harm to the fetus)
- Have a genetic factor such as a BRCA mutation, which might increase your chance of a second cancer
- Have a serious connective tissue disease such as scleroderma or lupus, which may make you especially sensitive to the side effects of radiation therapy
- Have inflammatory breast cancer
For women who are worried about breast cancer coming back, it is important to understand that having a mastectomy instead of breast-conserving surgery plus radiation only lowers your risk of developing a second breast cancer in the same breast. It does not lower the chance of the cancer coming back in other parts of the body, including the opposite breast.
Breast reconstruction surgery after mastectomy
After having a mastectomy a woman might want to consider having the breast mound rebuilt to restore the breast's appearance. This is called breast reconstruction. Although each case is different, most mastectomy patients can have reconstruction. Reconstruction can be done at the same time as the mastectomy or sometime later.
If you are thinking about having reconstructive surgery, it’s a good idea to discuss it with your surgeon and a plastic surgeon before your mastectomy. This allows the surgical teams to plan the treatment that’s best for you, even if you wait and have the reconstructive surgery later. Insurance companies typically cover breast reconstruction, but you should check with your insurance company so you know what is covered.
Going flat
Some women choose not to have reconstructive surgery. Wearing a breast prosthesis (breast form) is an option for women who want to have the shape of a breast under their clothes without having surgery. Some women are also comfortable with just ‘going flat’. Going flat involves a procedure called aesthetic flat closure or flat closure. A flat closure means the extra fat, skin, and other tissue in the breast area are removed and the leftover tissue is tightened and smoothed out to flatten the chest wall.
Recovering from a mastectomy
In general, women having a mastectomy stay in the hospital for 1 or 2 nights and then go home. How long it takes to recover from surgery depends on what procedures were done, and some women may need help at home. Most women should be fairly functional after going home and can often return to their regular activities within about 4 weeks. Recovery time is longer if breast reconstruction was also done, and it can take months to return to full activity after some procedures.
Ask your health care team how to care for your surgery site and arm. Usually, you and your caregivers will get written instructions about care after surgery. These instructions typically cover:
- How to care for the surgery site and dressing
- How to care for your drain, if you have one (this is a plastic or rubber tube coming out of the surgery site attached to a soft rubber ball that collects the fluid that occurs during healing)
- How to tell if an infection is starting
- Bathing and showering after surgery
- When to call the doctor or nurse
- When to start using your arm again and how to do arm exercises to prevent stiffness
- When you can start wearing a bra again
- When to begin using a prosthesis and what type to use
- Use of medicines, including pain medicines and possibly antibiotics
- Any restrictions on activity
- What to expect regarding sensations or numbness in the breast and arm
- What to expect regarding feelings about body image
- When to see your doctor for a follow-up appointment
- Referral to an ACS CARES volunteer. Through ACS CARES, a specially trained volunteer who has had breast cancer and can provide information, comfort, and support.
Possible side effects of mastectomy
Bleeding and infection at the surgery site are possible with all operations. The side effects of mastectomy can depend on the type of mastectomy you have (complex surgeries tend to have more side effects). Side effects can include:
- Pain or tenderness at the surgery site
- Swelling at the surgery site
- Buildup of blood in the wound (hematoma)
- Buildup of clear fluid in the wound (seroma)
- Limited arm or shoulder movement
- Numbness in the chest or upper arm
- Neuropathic (nerve) pain (sometimes described as burning or shooting pain) in the chest wall, armpit, and/or arm that doesn’t go away over time. It is also called post-mastectomy pain syndrome or PMPS.
- If axillary lymph nodes are also removed, other side effects such as lymphedema may occur.
Treatment after mastectomy
Some women might get other treatments after a mastectomy, such as hormone therapy to help lower the risk of the cancer coming back. Some women might also need chemotherapy, or targeted therapy after surgery. If so, radiation therapy and/or hormone therapy is usually delayed until the chemotherapy is completed. Talk to your doctor about what to expect.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
Gieni M, Avram R, Dickson L, et al. Local breast cancer recurrence after mastectomy and immediate breast reconstruction for invasive cancer: a meta-analysis. Breast 2012;21(3):230–236.
Henry NL, Shah PD, Haider I, Freer PE, Jagsi R, Sabel MS. Chapter 88: Cancer of the Breast. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa: Elsevier; 2020.
Jagsi R, King TA, Lehman C, Morrow M, Harris JR, Burstein HJ. Chapter 79: Malignant Tumors of the Breast. In: DeVita VT, Lawrence TS, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 11th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2019.
Kwong A and Sabel MS. Mastectomy. In Chen W, ed. UpToDate. Waltham, Mass.: UpToDate, 2021. https://www.uptodate.com. Accessed July 8, 2021.
National Cancer Institute. Aesthetic flat closure. Accessed at https://www.cancer.gov/publications/dictionaries/cancer-terms/def/aesthetic-flat-closure on December 20, 2023.
National Cancer Institute. Physician Data Query (PDQ). Breast Cancer Treatment – Patient Version. 2021. Accessed at https://www.cancer.gov/types/breast/patient/breast-treatment-pdq on July 8, 2021.
National Comprehensive Cancer Network (NCCN). Practice Guidelines in Oncology: Breast Cancer. Version 4.2021. Accessed at https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf on June 25, 2021.
Oh J.L. (2008) Multifocal or Multicentric Breast Cancer: Understanding Its Impact on Management and Treatment Outcomes. In: Hayat M.A. (eds) Methods of Cancer Diagnosis, Therapy and Prognosis. Methods of Cancer Diagnosis, Therapy and Prognosis, vol 1. Springer, Dordrecht. https://doi.org/10.1007/978-1-4020-8369-3_40.
OJ Vilholm, S Cold, L Rasmussen and SH Sindrup. The postmastectomy pain syndrome: an epidemiological study on the prevalence of chronic pain after surgery for breast cancer. British Journal of Cancer (2008) 99, 604 – 610.
Sabel MS. Breast-conserving therapy. In Chen W, ed. UpToDate. Waltham, Mass.: UpToDate, 2021. https://www.uptodate.com. Accessed July 8, 2021.
Last Revised: March 31, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



