Lymphedema
Lymphedema is a build-up of lymph fluid in the fatty tissues just under your skin that causes swelling (edema). Lymph fluid travels throughout the body and is part of the lymph or lymphatic system. Certain cancers and cancer treatments can increase your risk for developing lymphedema.
- The lymphatic system and lymphedema
- What causes lymphedema?
- Cancer treatment as a cause of lymphedema
- What areas of the body does lymphedema affect?
- What are symptoms of lymphedema?
- Stages of lymphedema
- Treatment for lymphedema
- Tips for preventing and managing lymphedema
- Talk to your doctor or cancer care team
The lymphatic system and lymphedema
The lymph (or lymphatic) system is part of your body's immune system. It helps maintain the right balance of fluids in your body, transports immune cells and nutrients, and filters out germs and waste.
- Lymph fluid is the clear fluid inside lymph vessels that travels throughout the body. It contains proteins, salts, water, and white blood cells (infection-fighting cells).
- Lymph vessels carry the lymph fluid throughout the body. One-way valves inside lymph vessels help move the fluid and control the flow.
- Lymph nodes are small, bean-sized glands along the lymph vessels that help filter germs, dead cells, and other waste. Lymph nodes are in many parts of the body, including the neck, armpit, chest, abdomen (belly), and groin.
In some ways, the lymphatic system works like the cardiovascular system. Both systems transport fluid (blood or lymph) through vessels throughout the body.
But the cardiovascular system has a powerful pump (the heart) to move blood through the body. The lymph system doesn’t have a pump. Instead, it relies on lymph nodes and the movement of muscles to keep fluid moving. This is why the lymph system is more likely to have poor drainage in some places, especially if lymph nodes are damaged or removed.
What causes lymphedema?
Lymphedema can occur when the lymph system is damaged, which can prevent the lymph fluid from moving through the body.
Cancer treatment as a cause of lymphedema
Any cancer that affects the lymph system can cause lymphedema. But it’s most common in certain cancers including:
- Breast cancer
- Prostate cancer
- Pelvic area cancers (such as bladder, penile, testicular, endometrial, vulvar, or cervical cancer)
- Lymphoma
- Melanoma
- Head and neck cancers
The risk for lymphedema is higher in these cancers because they often require surgery or radiation that involves lymph nodes.
Lymphedema and surgery for cancer
Some surgeries to treat cancer (for example, most breast cancer surgeries) include removing one or more lymph nodes. Removing lymph nodes is like closing lanes on a highway. Cars can’t get through as easily and traffic slows down. Lymph fluid – like the cars – starts to back up and causes swelling in the body parts that those lymph nodes drain fluid from.
Surgery for breast cancer often involves removing lymph nodes from the armpit area, which is why some people get lymphedema in the hand or arm after breast surgery. The more lymph nodes removed, the higher your risk for lymphedema. A sentinel node biopsy usually removes 2 or 3 lymph nodes. An axillary node dissection usually removes between 5 and 30 lymph nodes from the armpit (axilla).
Surgery for other types of cancer might include the removal of lymph nodes in other parts of the body, such as the pelvic area or groin. The risk of lymphedema will depend on the location and number of lymph nodes that must be removed.
Lymphedema and radiation for cancer
Radiation therapy can also cause lymphedema. Radiation can damage or scar nearby lymph nodes. Damaged lymph nodes don’t work well, allowing fluid to back up and cause swelling.
Lymphedema not caused by cancer treatment
Tumors and enlarged lymph nodes can also cause lymphedema if they are pressing on and blocking the flow of lymph fluid.
There are non-cancer causes of lymphedema as well:
- Infections that damage tissue or cause scarring
- Other health conditions, such as heart or vascular disease, arthritis, and eczema
- Gene changes or mutations that involve the lymph system
- Injury or trauma to a certain part of the body
What areas of the body does lymphedema affect?
Lymphedema is most common in the arms and legs. But since we have lymph nodes all through our body, it can develop anywhere.
- Surgery or radiation near the abdomen (belly) or pelvis can cause swelling or lymphedema in the abdomen, genitals, or legs.
- Surgery or radiation in the head and neck area can cause swelling or lymphedema in the face and neck.
What are symptoms of lymphedema?
It’s important to notice lymphedema early so you can start treatment right away. Lymphedema that isn’t treated can get worse and even become permanent.
Common signs and symptoms of lymphedema can include:
- Swelling, fullness, or heaviness in the breast, chest, shoulder, arm, hand, leg, or foot
- Skin changes such as dryness, discoloration, thickening, or dimpling
- New aching, tingling, numbness, pain, or discomfort
- Less movement or flexibility in your joints
- Trouble putting clothes on, feeling clothes are tighter, or leaving indents on your skin
- Your shirt collar, ring, watch, or bracelet feels tight, even though you haven’t gained weight
Stages of lymphedema
If you have lymphedema, your cancer care team might describe it as being stage 0, 1, 2, or 3.
- Stage 0: No visible swelling, but slight symptoms such as feeling the area is heavy, full, or tight. Reversible.
- Stage 1 (mild): Visible swelling. Area might also feel heavy, full, or tight. If arms or legs are involved, the swelling improves when the arm or leg is raised. Usually reversible.
- Stage 2 (moderate): More swelling than stage 1. If arms or legs involved, swelling doesn’t get better when the arm or leg is raised. Worse symptoms than stage 1. May be reversible if treated early.
- Stage 3 (severe): Extreme swelling that often limits self-care or everyday activities. Skin can be very dry, thickened, or discolored. May have fluid leaking or blisters. Usually not reversible.
Treatment for lymphedema
It’s important to identify and treat lymphedema as early as possible when it’s most likely to be reversible. The goals of lymphedema treatment are to reduce swelling, prevent infection (cellulitis), improve ability to move and function, and relieve discomfort.
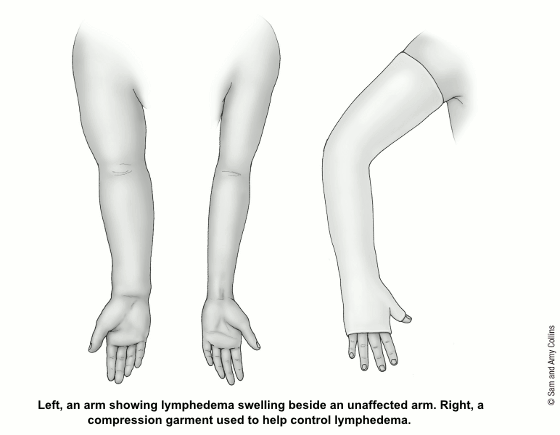
Treating mild lymphedema
Common treatments for early-stage or mild lymphedema include:
- Elevation of affected area to allow gravity to help drain extra fluid.
- Exercises and movements that promote fluid drainage and improve range of motion.
- Skin and nail care to prevent cuts or injuries to the skin around the affected area, which can make lymphedema worse or lead to cellulitis.
- Manual lymphatic drainage (MLD) is a type of gentle massage that helps move lymph fluid out of the swollen area. A trained therapist does this and might teach you how to do self MLD at home.
- Compression garments are special sleeves or stockings to prevent fluid build-up. A prescription from your doctor is needed. They are fitted to you by a professional and apply different amounts of pressure in different areas. Never wear a compression garment that hasn’t been fitted for you. This can trigger lymphedema or make it worse.
Treating moderate lymphedema
Complete decongestive therapy (CDT) is the combination of manual lymphatic drainage, compression therapy, skin care, exercises, and elevation. CDT is often used to manage mild to moderate lymphedema.
Treating severe lymphedema
For severe lymphedema, intermittent pneumatic compression (IPC) might be added to the treatment plan. IPC is a type of compression therapy where a sleeve or stocking is applied to the affected areas and inflated (like a blood pressure cuff). It applies specific amounts of pressure to move fluid out of the area. IPC might also be used for less severe cases of lymphedema if a person can’t wear compression garments or can’t do manual self-lymphatic drainage.
Surgery might be an option if lymphedema is severe and hasn’t improved with other treatments.
- Liposuction removes extra fat that can develop in areas of lymphedema.
- Lympho-venous or lymphatic bypass takes lymph vessels and attaches them to small veins to improve drainage.
- Vascularized lymph node transfer (VLNT) takes healthy lymph nodes from another part of the body and places them in the area with lymphedema.
Tips for preventing and managing lymphedema
Lymphedema can develop many years after cancer treatment, even if you’ve never had it before. If you have had a type of treatment that puts you at high risk of lymphedema, it’s important to continue to watch for signs and take steps to prevent lymphedema from starting, returning, or getting worse. Here are some tips for preventing and managing lymphedema.
Take care of your skin
Skin care is one of the most important things you can do if you are at risk for lymphedema. Cuts and injuries to the skin can trigger lymphedema or make it worse. The skin around the area where there are damaged or missing lymph nodes is always at risk of infection because lymph nodes are part of the immune system that protects us.
- Protect your skin from injuries, cuts, and bites.
- Avoid having blood draws from veins in the affected arm, when possible.
- Wear gloves when doing yardwork or gardening.
- Wear shoes or protective socks.
- Keep skin moisturized to prevent cracking.
- Wear sunscreen with an SPF of at least 30 to prevent sunburns.
- Be careful with sharp objects and tools.
- Be careful when cutting your cuticles.
- Avoid extreme heat on the area (such as hot compresses, saunas, and hot tubs).
- Wash any cuts, bites, or breaks in the skin with soap and water. Call your doctor if it isn’t healing or has any signs of infection (warm, red, tender, pus leaking).
Promote fluid circulation
Body areas that have damaged or missing lymph nodes can’t move and drain lymph fluid through the area as well. But there are things you can do to promote drainage of lymph fluid:
- Don’t wear tight clothing, jewelry, or other items that constrict or squeeze the affected area.
- If you wear a compression garment, wear it as directed. These garments apply measured and specific amounts of pressure to different areas and are not the same as tight clothing.
- Don’t wear a compression garment that doesn’t fit or that you’ve grown out of. Get re-fitted for a garment every few months.
- Avoid having blood pressure measurements taken on the affected arm, when possible.
- Ask your doctor or therapist what exercises are good for your type and area of lymphedema.
- Raising the affected arm or leg (above the level of your heart if possible) can improve swelling.
- If you have lymphedema in your lower body, avoid crossing your legs.
- Ask how to do manual lymph drainage (self-massage) on yourself.
- Note any changes in size, shape, or color of the affected area. Compare to the non-affected side if possible. Tell your doctor right away if you notice any changes.
Does drinking water help with lymphedema?
Drinking plenty of fluids each day is important for everyone at every age. Drinking enough water helps the body filter and get rid of excess fluid and waste products.
Researchers recently studied how people cope with lymphedema. One part of the study looked at their eating and drinking habits. The researchers found:
- About 1 in 3 study participants reported that increasing their daily water intake was helpful for their symptoms.
- About 1 in 4 study participants rated decreased alcohol intake as very helpful in controlling symptoms.
Water is usually the best choice for daily hydration. In addition to water, choosing unsweetened, low-fat beverages can support fluid intake. Water is also found in many foods, such as vegetables, fruits, broths and soups. Learn more in Nutrition During and After Cancer Treatment.
Skin hydration is important, too, especially in the areas affected by lymphedema. If you have lymphedema, check to see which moisturizers are recommended by your cancer care team to keep skin hydrated.
Talk to your doctor or cancer care team
Call your doctor or lymphedema therapist if you notice any signs of lymphedema or cellulitis, or if:
- You have new or worse pain in the affected area.
- You have lymphedema and get a cut, bite, or other injury to the area.
- Any part of the affected area feels hot, looks red, or swollen.
- You have a fever that's not from being sick.
- You have other signs or symptoms of an infection, like chills, sweats, muscle pain or aches, nausea, or dizziness.
Ask your doctor or cancer care team:
- What symptoms should I call for versus sending a message?
- When should I not call and go right to the emergency room?
- Who should I call first? Primary doctor, nurse, oncologist, or someone else?
- What should I do if I can’t reach someone at the office or clinic?
To learn more
Lymphatic Education & Resource Network: The LE&RN Resource Guide offers videos, newsletters, frequently asked questions, personal stories, and a list of lymphedema specialty centers. They also connect people with lymphedema to others through state and international community chapters.
Find a certified lymphedema therapist (CLT):
- Lymphology Association of North America (LANA)
www.clt-lana.org - National Lymphedema Network (NLN)
1-800-541-3259
www.lymphnet.org
- Written by
- References

Developed by the American Cancer Society medical and editorial content team with medical review and contribution by the American Society of Clinical Oncology (ASCO).
Admoun C, Mayrovitz HN. Coping mechanisms for lymphedema: An analysis of patient experiences. Cureus. 2023;15(7):e41573. Available at https://pmc.ncbi.nlm.nih.gov/articles/PMC10406395/
Executive Committee of the International Society of Lymphology. The diagnosis and treatment of peripheral lymphedema: 2020 Consensus Document of the International Society of Lymphology. Lymphology. 2020;53(1):3-19.
Kilbreath SL, Ward LC, Davis GM, et al. Reduction of breast lymphoedema secondary to breast cancer: a randomized controlled exercise trial. Breast Cancer Res Treat. 2020;184(2):459-467.
Lymphatic Education & Research Network. Lymphedema: what you need to know. Massachusetts General Hospital. 2019. Accessed December 18, 2023.
Mehrara B. Clinical staging and conservative management of peripheral lymphedema. UpToDate. UpToDate Inc; 2023. Updated November 2022. Accessed December 18, 2023. https://www.uptodate.com/contents/clinical-staging-and-conservative-management-of-peripheral-lymphedema
Mehrara B. Surgical treatment of primary and secondary lymphedema. UpToDate. UpToDate Inc; 2023. Updated August 2023. Accessed December 18, 2023. https://www.uptodate.com/contents/surgical-treatment-of-primary-and-secondary-lymphedema
National Cancer Institute (NCI). Lymphedema. Updated March 6, 2024. Accessed from https://www.cancer.gov/about-cancer/treatment/side-effects/lymphedema#can-i-prevent-lymphedema on May 20, 2025.
National Comprehensive Cancer Network (NCCN). Clinical Practice Guidelines in Oncology Survivorship. Version 1.2025. Accessed at www.nccn.org on May 20, 2025.
Ridner SH, Dietrich MS, Deng J, Ettema SL, Murphy B. Advanced pneumatic compression for treatment of lymphedema of the head and neck: a randomized wait-list controlled trial. Support Care Cancer. 2021;29(2):795-803. doi:10.1007/s00520-020-05540-8
Schmitz KH, Troxel AB, Dean LT, et al. Effect of home-based exercise and weight loss programs on breast cancer-related lymphedema outcomes among overweight breast cancer survivors: the WISER survivor randomized clinical trial. JAMA Oncol. 2019;5(11):1605-1613. doi:10.1001/jamaoncol.2019.2109
Last Revised: May 20, 2025
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.


