Your gift is 100% tax deductible.
Lymph Node Surgery for Breast Cancer
If breast cancer spreads, it typically goes first to nearby lymph nodes under the arm. It can also sometimes spread to lymph nodes near the collarbone or near the breast bone (the front center of the chest). Knowing if the cancer has spread to your lymph nodes helps doctors find the best way to treat your cancer.
If you have been diagnosed with breast cancer, it’s important to find out how far the cancer has spread. To help find out if the cancer has spread outside the breast, one or more of the lymph nodes under the arm (axillary lymph nodes) are removed and checked in the lab.
This is an important part of staging. If the lymph nodes have cancer cells, there is a higher chance that cancer cells have also spread to other parts of the body. More imaging tests might be done if this is the case.
Lymph node removal can be done in different ways, depending on whether any lymph nodes are enlarged, how big the breast tumor is, and other factors.
Biopsy of an enlarged lymph node
If any of the lymph nodes under the arm or around the collarbone are swollen, they may be checked for cancer with a needle biopsy, either a fine needle aspiration (FNA) or a core needle biopsy. Less often, the enlarged node is removed with surgery. If cancer is found in the lymph node, more nodes will need to be removed (see below).
Types of lymph node surgery
Even if the nearby lymph nodes are not enlarged, they will still need to be checked for cancer. This can be done in two ways:
- Most often, a sentinel lymph node biopsy (SLNB) is done, during which only a few lymph nodes are removed.
- In some cases, an axillary lymph node dissection (ALND), which removes more lymph nodes, might be needed.
Lymph node surgery is often done as part of the main surgery to remove the breast cancer, but sometimes it might be done as a separate operation.
Sentinel lymph node biopsy
In a sentinel lymph node biopsy (SLNB), the surgeon finds and removes the first lymph node(s) to which a cancer is likely to spread (called the sentinel nodes). To do this, a substance is injected into the tumor, the area around it, or the area around the nipple. This can be done with either:
- A radioactive substance and/or a blue dye, OR
- A liquid containing coated iron oxide particles
Lymph vessels will carry these substances along the same path that the cancer would likely take. The first lymph node(s) the substance travels to will be the sentinel node(s).
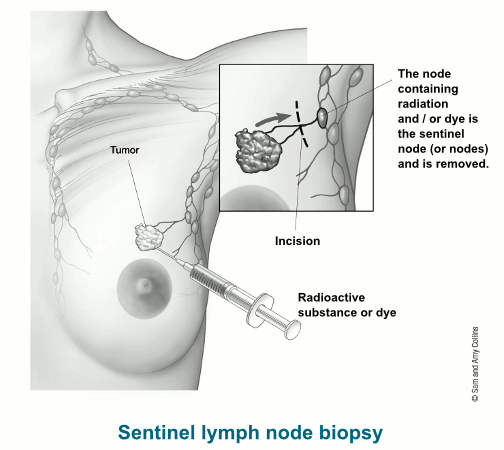
After the substance has been injected, the sentinel node(s) can be found by:
- Using a special machine to detect either radioactivity or iron oxide particles in the nodes
- Looking for nodes that have turned blue (or brown, if iron oxide particles are used)
Sometimes, both methods are used.
The surgeon cuts the skin over the lymph node area and removes the affected node(s).
The few removed lymph nodes are then checked closely in the lab for cancer cells by a pathologist. Sometimes, this is done during the surgery. Because there is a chance that other lymph nodes in the same area will also have cancer if cancer is found in the sentinel lymph node(s), the surgeon may go ahead with an axillary dissection (ALND) to remove more lymph nodes while you are still on the operating table. If no cancer cells are seen in the node(s) at the time of the surgery, or if they are not checked by a pathologist at the time of the surgery, they will be examined more closely over the next several days.
If cancer is found in the sentinel node(s) later, the surgeon may recommend an ALND at a later time to check more nodes for cancer. Studies have shown, however, that in some cases it may be safe to leave the rest of the lymph nodes behind. This is based on certain factors, such as the size of the breast tumor, what type of surgery is used to remove the tumor, and what treatment is planned after surgery, among other things.
Based on the studies that have looked at this, skipping the ALND may be an option for:
- Women with breast tumors 5 cm (about 2 inches) across or smaller who have no more than 2 positive sentinel lymph nodes, are having breast-conserving surgery followed by radiation, and did not get any chemotherapy before surgery.
- Women who have lymph nodes with a very small amount of cancer (no more than 2 mm) and are having a mastectomy.
If there is no cancer in the sentinel node(s), it's very unlikely that the cancer has spread to other lymph nodes, so no further lymph node surgery will be needed.
SLNB is often considered for women with early-stage breast cancer and is typically not used for women with inflammatory breast cancer. It might be used for women with locally advanced breast cancer in certain instances, such as after neoadjuvant treatment.
Although SLNB has become a common procedure, it requires a great deal of skill. It should be done only by a surgeon who has experience with this technique. If you are offered this type of biopsy, ask your surgeon if they do them regularly.
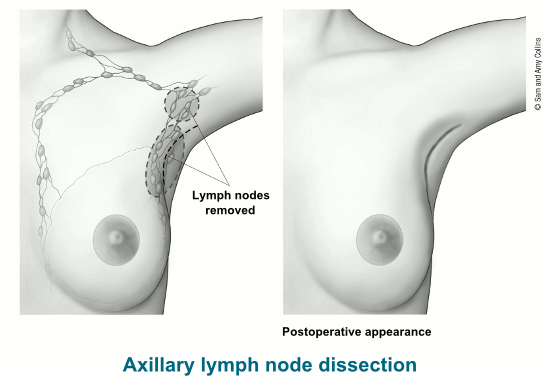
Axillary lymph node dissection (ALND)
In this procedure, anywhere from about 10 to 40 (though usually less than 20) lymph nodes are removed from the area under the arm (axilla) and checked for cancer spread. ALND is usually done at the same time as a mastectomy or breast-conserving surgery (BCS), but it can be done in a second operation. ALND may be needed:
- If a previous SLNB has shown 3 or more of the underarm lymph nodes have cancer cells
- If swollen underarm or collarbone lymph nodes can be felt before surgery or seen on imaging tests and a FNA or core needle biopsy shows cancer
- If the cancer has grown large enough to extend outside the lymph node(s)
- If the SLNB is positive for cancer cells after chemotherapy was given to shrink the tumor before surgery
Side effects of lymph node surgery
After lymph node surgery, pain, swelling, bleeding, blood clots, and infection are possible.
Lymphedema
A possible long-term effect of lymph node surgery is swelling in the arm or chest called lymphedema. Because any excess fluid in the arms normally travels back into the bloodstream through the lymph system, removing the lymph nodes sometimes blocks drainage from the arm, causing this fluid to build up.
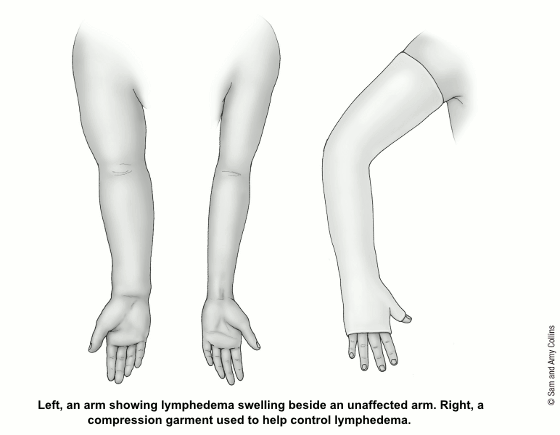
Lymphedema is less common after a sentinel lymph node biopsy (SLNB) than an axillary lymph node dissection (ALND). The risk is thought to be in the range of 5% to 17% in women who have a SLNB and around 20% to 30% in women who have an ALND. It may be more common if radiation is given after surgery or in women who have obesity. Sometimes the swelling lasts for only a few weeks and then goes away. But in some women, it lasts a long time. If your arm is swollen, tight, or painful after lymph node surgery, be sure to tell someone on your cancer care team right away.
Limited arm and shoulder movement
You might also have limited movement in your arm and shoulder after surgery. This is more common after ALND than SLNB. Your doctor may advise exercises to help keep you from having long-lasting problems (a frozen shoulder).
Some women notice a rope-like structure that begins under the arm and can extend down toward the elbow. This is sometimes called axillary web syndrome or lymphatic cording. It is more common after ALND than SLNB. Symptoms may not appear for weeks or even months after surgery. It can cause pain and limit movement of the arm and shoulder. This often goes away without treatment, although some women may find physical therapy helpful.
Numbness
Numbness of the skin on the upper, inner arm is a common side effect because the nerve that controls sensation (feeling) here travels through the lymph node area.
- Written by
- References

The American Cancer Society medical and editorial content team
Our team is made up of doctors and oncology certified nurses with deep knowledge of cancer care as well as editors and translators with extensive experience in medical writing.
Henry NL, Shah PD, Haider I, Freer PE, Jagsi R, Sabel MS. Chapter 88: Cancer of the Breast. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa: Elsevier; 2020.
Jagsi R, King TA, Lehman C, Morrow M, Harris JR, Burstein HJ. Chapter 79: Malignant Tumors of the Breast. In: DeVita VT, Lawrence TS, Lawrence TS, Rosenberg SA, eds. DeVita, Hellman, and Rosenberg’s Cancer: Principles and Practice of Oncology. 11th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2019.
Doscher ME, Schreiber JE, Weichman KE, Garfein ES. Update on Post-mastectomy Lymphedema Management. Breast J. 2016 Sep;22(5):553-60.
Giuliano AE, Hunt KK, Ballman KV, et al. Axillary dissection vs no axillary dissection in women with invasive breast cancer and sentinel node metastasis. JAMA. 2011;305:569-575.
James TA, Coffman AR, Chagpar AB, et al. Troubleshooting Sentinel Lymph Node Biopsy in Breast Cancer Surgery. Ann Surg Oncol. 2016;23(11):3459–3466. doi:10.1245/s10434-016-5432-8.
Lawenda BD, Mondry TE, Johnstone PA. Lymphedema: A primer on the identification and management of a chronic condition in oncologic treatment. CA Cancer J Clin. 2009; 59:8–24.
National Cancer Institute. Physician Data Query (PDQ). Lymphedema – Health Professional Version. 2019. Accessed at https://www.cancer.gov/about-cancer/treatment/side-effects/lymphedema/lymphedema-hp-pdq on July 12, 2021.
National Comprehensive Cancer Network (NCCN). Practice Guidelines in Oncology: Breast Cancer. Version 5.2021. Accessed at https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf on July 12, 2021.
National Comprehensive Cancer Network (NCCN). Practice Guidelines in Oncology: Survivorship. Version 2.2021. Accessed at https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf on July 12, 2021.
OJ Vilholm, S Cold, L Rasmussen and SH Sindrup. The postmastectomy pain syndrome: an epidemiological study on the prevalence of chronic pain after surgery for breast cancer. British Journal of Cancer (2008) 99, 604 – 610.
Last Revised: January 3, 2023
American Cancer Society medical information is copyrighted material. For reprint requests, please see our Content Usage Policy.
American Cancer Society Emails
Sign up to stay up-to-date with news, valuable information, and ways to get involved with the American Cancer Society.



